

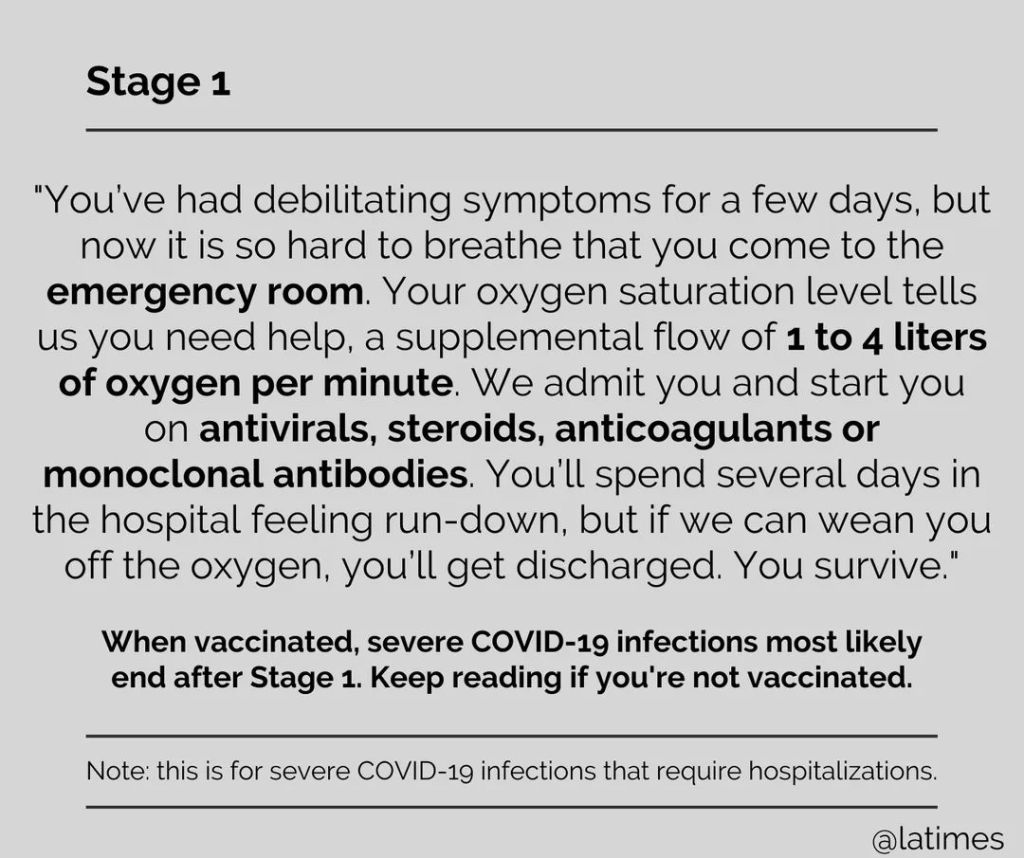



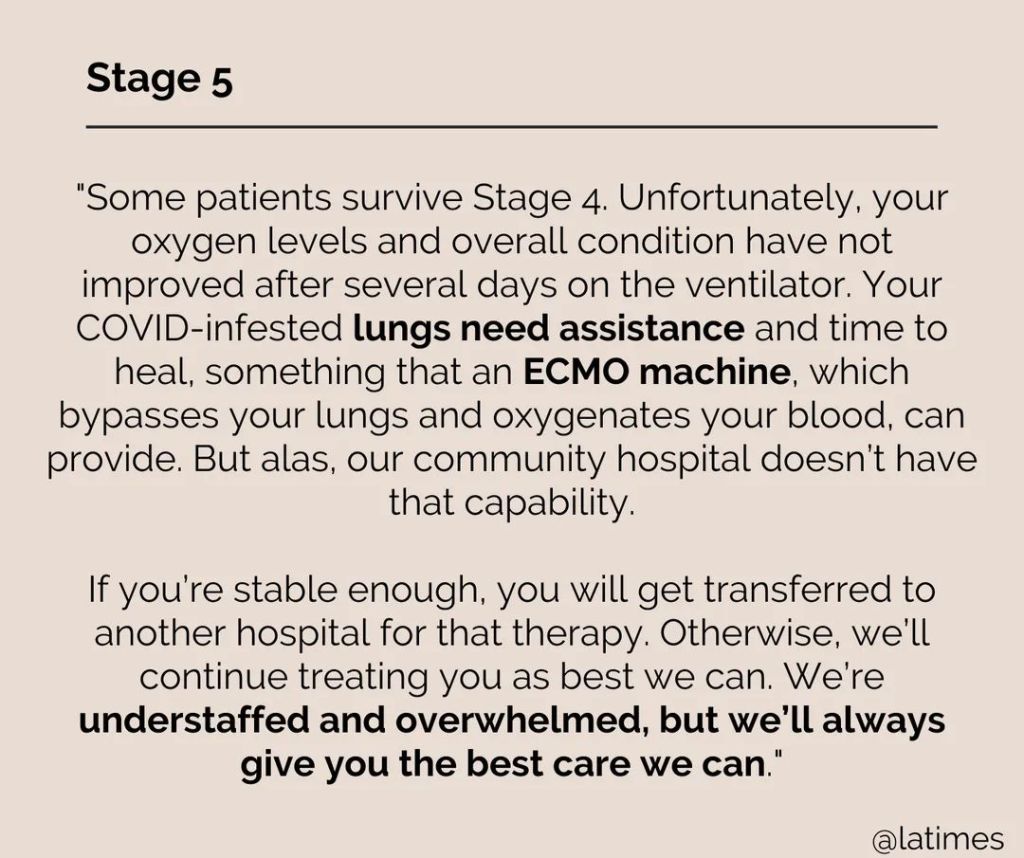
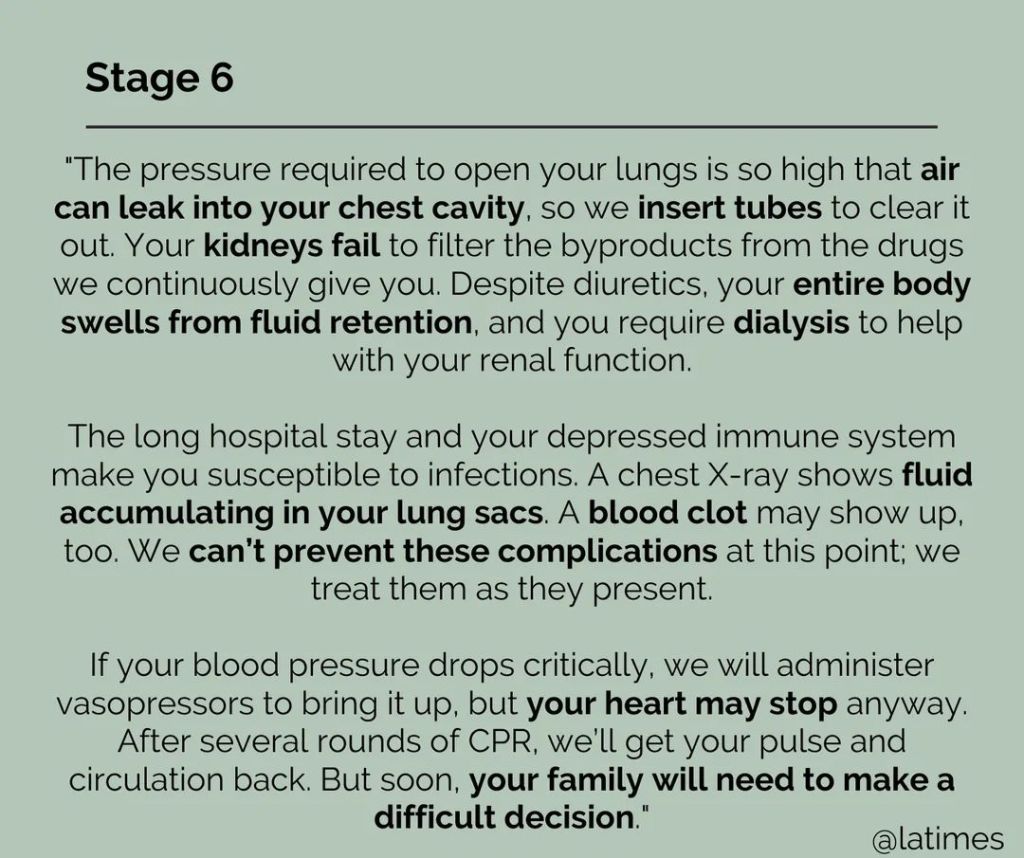



Health system leaders use benchmarking as a way to determine how their organizations stack up against both local and regional peers.
Below are 67 financial benchmarks, including key ratios for health systems, as well as revenue and margin metrics, broken down by rating category.
Key balance sheet metrics, ratios:
Source: Fitch Ratings’ “2021 Median Ratios: Not-for-Profit Hospitals and Healthcare Systems” report. It was released Aug. 3.
1. Cash on hand: 255 days
2. Accounts receivable: 44.6 days
3. Cushion ratio: 29x
4. Current liabilities: 95 days
5. Cash to debt: 169.9 percent
6. Cash to adjusted debt: 161.1 percent
7. Operating margin: 1.3 percent
8. Operating EBITDA margin: 6.7 percent
9. Excess margin: 3.1 percent
10. EBITDA margin: 8.5 percent
11. Net adjusted debt to adjusted EBITDA: -2.6 percent
12. Personnel costs as percent of total operating revenue: 55 percent
13. EBITDA debt service coverage: 3.9x
14. Operating EBITDA debt service coverage: 3.2x
15. Maximum annual debt service as percent of revenues: 2.2 percent
16. Debt to EBITDA ratio: 4.4x
17. Debt to capitalization: 35.2 percent
18. Average age of plant: 11.4 years
19. Capital expenditures as percent of depreciation expense: 110.1 percent
Margins, revenue financial benchmarks broken down by rating category:
Source: S&P Global Ratings “U.S. Not-For-Profit Health Care System Median Financial Ratios — 2019 vs. 2021″ report.” The report was released Aug. 30.
“AA+” rating
20. Net patient service revenue: $4.16 billion
21. Total operating revenue: $4.43 billion
22. Operating margin: 4.5 percent
23. Operating EBIDA margin: 11.3 percent
24. Excess margin: 5.5 percent
25. EBIDA margin: 12.2 percent
“AA” rating
26. Net patient service revenue: $3.98 billion
27. Total operating revenue: $4.95 billion
28. Operating margin: 3.2 percent
29. Operating EBIDA margin: 8.3 percent
30. Excess margin: 5.8 percent
31. EBIDA margin: 10.7 percent
“AA-” rating
32. Net patient service revenue: $3.08 billion
33. Total operating revenue: $3.41 billion
34. Operating margin: 1.9 percent
35. Operating EBIDA margin: 7.1 percent
36. Excess margin: 4.1 percent
37. EBIDA margin: 9.2 percent
“A+” rating
38. Net patient service revenue: $2.26 billion
39. Total operating revenue: $2.55 billion
40. Operating margin: 3 percent
41. Operating EBIDA margin: 7.1 percent
42. Excess margin: 5.5 percent
43. EBIDA margin: 10.9 percent
“A” rating
44. Net patient service revenue: $2.69 billion
45. Total operating revenue: $3.07 billion
46. Operating margin: 0.7 percent
47. Operating EBIDA margin: 6.6 percent
48. Excess margin: 5.5 percent
49. EBIDA margin: 2.3 percent
“A-” rating
50. Net patient service revenue: $2.08 billion
51. Total operating revenue: $2.69 billion
52. Operating margin: 0.6 percent
53. Operating EBIDA margin: 6.7 percent
54. Excess margin: 2.4 percent
55. EBIDA margin: 8 percent
“BBB+” rating
56. Net patient service revenue: $1.85 billion
57. Total operating revenue: $2.27 billion
58. Operating margin: -0.2 percent
59. Operating EBIDA margin: 5 percent
60. Excess margin: 0.5 percent
61. EBIDA margin: 6 percent
“BBB” rating
62. Net patient service revenue: $2.96 billion
63. Total operating revenue: $4.11 billion
64. Operating margin: -3.2 percent
65. Operating EBIDA margin: 1.6 percent
66. Excess margin: -2 percent
67. EBIDA margin: 2.8 percent

Providence is investing $220 million to fill open positions and give bonuses to current employees, the Renton, Wash.-based system announced Sept. 3.
The health system is giving a $1,000 bonus to every caregiver who has been with the organization for at least 90 days. The bonuses, which will be given to workers up to and including the director level, will be paid in two installments in September and December.
Providence is also making investments to rapidly fill 17,000 job openings. The system said it is offering sign-on bonuses to front-line workers with the goal of filling positions quickly and alleviating the stress and burnout many clinicians are experiencing. Current employees are eligible for referral bonuses of between $1,000 and $7,500.
“Our caregivers are the core of who we are, and we have been committed to supporting their health and well-being throughout the pandemic,” Providence President and CEO Rod Hochman, MD, said in a news release. “Now, as we enter month 21 of our COVID-19 response, it’s even more imperative to continue to care for and bolster those who make our mission possible.”
https://mailchi.mp/13ef4dd36d77/the-weekly-gist-august-27-2021?e=d1e747d2d8

There’s been a lot of hand wringing over the ongoing feeding frenzy among private equity (PE) firms for physician practice acquisition, which has caused health system executives everywhere to worry about the displacement effect on physician engagement strategies (not to mention the inflationary impact on practice valuations).
While we’ve long believed that PE firms are not long-term owners of practices, instead playing a roll-up function that will ultimately end in broader aggregation by vertically-integrated insurance companies, a recent conversation with one system CEO reframed the phenomenon in a way we hadn’t thought of before. It’s all about a demographic shift, she argued.
There’s a generation of Boomer-aged doctors who followed their entrepreneurial calling and started their own practices, and are now nearing retirement age without an obvious path to exit the business. Many didn’t plan for retirement—rather than a 401(k), what they have is equity in the practice they built.
What the PE industry is doing now is basically helping those docs transition out of practice by monetizing their next ten years of income in the form of a lump-sum cash payout. You could have predicted this phenomenon decades ago.
The real question is what happens to the younger generations of doctors left behind, who have another 20 or 30 years of practice ahead of them? Will they want to work in a PE-owned (or insurer-owned) setting, or would they prefer health system employment—or something else entirely?
The answer to that question will determine the shape of physician practice for decades to come…at least until the Millennials start pondering their own retirement.

The hourly mean wage for registered nurses in the U.S. is $38.47, according to the U.S. Bureau of Labor Statistics’ latest occupational employment and wage statistics survey.
Among 10 metropolitan areas with the highest employment level in registered nurses, registered nurses have the highest hourly mean wage in the Los Angeles area and the lowest in the Miami area.
Ten hourly mean wages for RNs by metropolitan area, in descending order:
1. Los Angeles: $54.38
2. Boston: $47.79
3. New York City: $45.63
4. Houston: $40.85
5. Washington, D.C.: $40.14
6. Philadelphia: $38.45
7. Dallas: $37.50
8. Chicago: $37.48
9. Detroit: $36.64
10. Miami: $34.76
Scripps Health is temporarily postponing some medical procedures because of significant staffing shortages and a jump in COVID-19 cases, the San Diego, Calif.-based system said Aug. 20, according to CBS News 8.
Medical staff is deciding which procedures to delay based on clinical factors and emergency status, with time-sensitive care still being delivered, Scripps leaders said.
The health system said it is also considering temporarily consolidating some ambulatory care sites due to workforce shortages.
At present, Scripps said it is looking to fill 1,309 open positions. In August 2019, the system had just 832 openings. About 430 of the openings are for nursing positions, up from 220 open positions in 2019, according to the report.
At the same time, the health system is seeing its COVID-19 patient volume grow. Scripps has 173 patients admitted at its five hospitals, up from 13 patients on June 13.
“The COVID pandemic has taken a serious toll on healthcare workers across the nation, and many have decided to leave the field entirely for reasons such as fatigue and burnout,” said Scripps’ President and CEO Chris Van Gorder, according to CBS News 8. “We’re doing all we can to fill open positions and shifts, but options are currently limited across the board in healthcare, so we’re doing what’s necessary to ensure we have staff available for our most urgent cases.”
To view the full article, click here.

Janesville, Wis.-based Mercyhealth has fired a vice president in charge of marketing and public relations over an alleged kickback scheme with a vendor, the Janesville Gazette reported Aug.16, citing a letter from the health system’s CEO.
The vice president, Barb Bortner, was fired after health system leaders learned of a $3 million fraudulent invoice and kickback scheme that she was allegedly involved in, Mercyhealth President and CEO Javon Bea said in the letter obtained by the Gazette.
“Our patients and communities we serve expect us to conduct our business affairs with the highest degree of integrity. We are all deeply saddened and disappointed that a member of our team has betrayed that trust,” Mr. Bea wrote in the letter, according to the Rockford Register Star.
Mr. Bea said Mercyhealth officials suspect Ms. Bortner is responsible for fraudulent and “improper” arrangements with an unnamed vendor, and the alleged fraud was linked to the system’s marketing division. Mercyhealth is severing ties with the vendor believed to be involved, the Gazette reported.
The fraud does not appear to have impacted patient care, and the system is taking “all necessary steps to improve Mercyhealth procedures,” Mr. Bea wrote, according to the report.
Read the full Gazette article here.
As some states set Covid-19 hospitalization records, many overwhelmed hospitals are outsourcing patients on planes, helicopters, and ambulances to distant cities and states for treatment, Heather Hollingsworth and Jim Salter write for the Associated Press.
As of last week, the number of Covid-19 patients in most hospitals remained below winter surge levels, Hollingsworth and Salter report. However, Florida, Arkansas, Oregon, Hawaii, Louisiana, and Mississippi recently set pandemic hospitalization records.
And unlike in the winter surge, many hospitals were already strained this summer due to patients catching up on previously deferred care, according to Hollingsworth and Salter.
“We are seeing Covid patients and we are seeing car accidents and we are seeing kids come in with normal seasonal viral infections. And we are seeing normal life come into the emergency department along with the extra surge of Covid patients, so it is causing that crisis,” said Mark Rosenberg, president of the American College of Emergency Physicians.
Amid the influx of patients, many of these overwhelmed hospitals are looking to neighboring cities and states for relief. For instance, in Arizona, a Covid-19 hotline is receiving calls from hospitals in Wyoming, Arkansas, Texas, and California in search of bed space, Hollingsworth and Salter report—although the hotline often cannot provide any help.
In Kansas, officials at the Wilson Medical Center in Kansas had to call 40 other facilities in several states seeking a bed for a Covid-19 patient before finally finding an available bed about 220 miles away. Across the state, according to Motient, a company contracting with Kansas to manage transfers, Covid-19 patients generally have to wait an average of 10 hours before being flown to another hospital location, which could be in Wisconsin, Illinois, Colorado, or Texas.
“That is just the worst day that you can have in the emergency room as a provider,” Richard Watson, Motient’s founder, said, “to be taking care of a patient that you are totally helpless to give them what you know they need.”
Similarly, in Washington state, the 25-bed Prosser Memorial Hospital, doesn’t have an intensive care unit, so critically ill patients are being sent as far as eastern Idaho—600 miles away.
Finding a hospital to take in patients has become more difficult due to recent staffing shortages, according to Robin Allaman, CNO at the Kearny County Hospital in Kansas.
“Most [hospitals] are saying it isn’t that they don’t have an open bed, it is that they don’t have nursing staff to care for them,” he said. Officials at his hospital called health systems in Nebraska, Oklahoma, and New Mexico before one in Colorado Springs, Colo.—200 miles away—agreed to take a recent patient.
Watson said these delayed transfers can have dire consequences for patients, especially those who need to see specialists, who often are available only in larger hospitals. “Imagine being with your grandma in the ER who is having a heart attack in western Kansas and you are saying, ‘Why can’t we find a bed for her?’ We are watching this happen right in front of us. ‘This is America. Why don’t we have hospital bed for her?’ Well, here we are,” he said.
And while experts had hoped that the vaccines would prevent hospitals from becoming overwhelmed again, Justin Lessler, a professor of epidemiology at Johns Hopkins University, said there hasn’t been the reduction in hospitalizations that officials had hoped for. That’s in part because the delta variant seems to be more severe, particularly in younger people, whose vaccination rates are lower.
Steve Edwards—CEO of CoxHealth, whose hospital in Springfield, Mo., is treating patients from as far away as Alabama—added, “Just imagine not having the support of your family near, to have that kind of anxiety if you have someone grow acutely ill.”