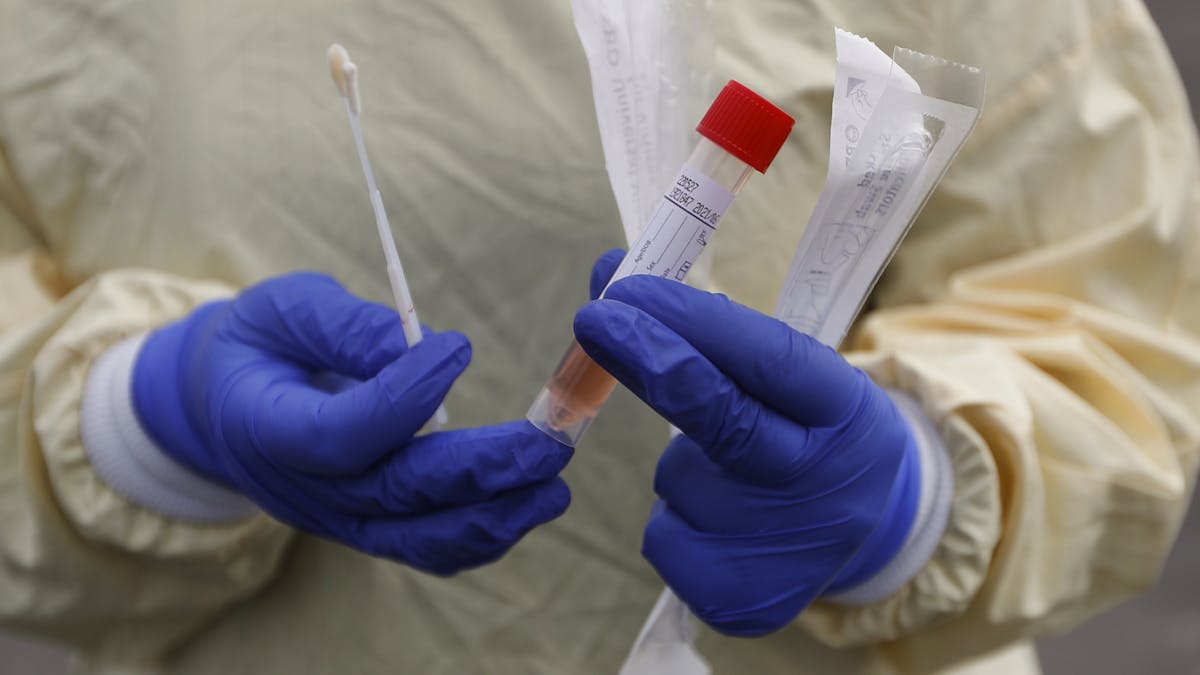
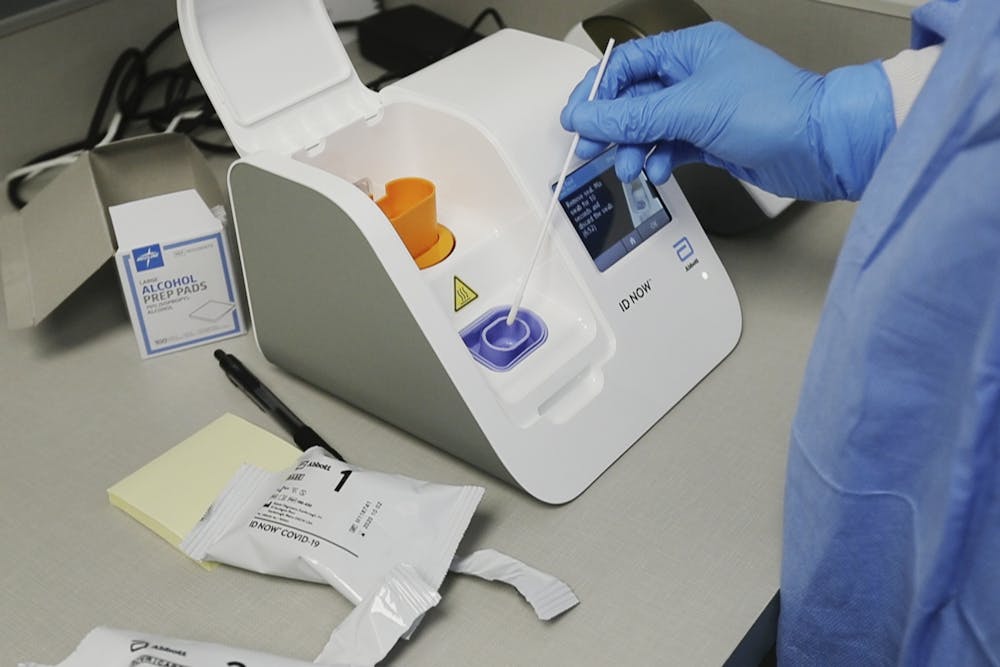
The image of scientists standing beside governors, mayors or the president has become common during the pandemic. Even the most cynical politician knows this public health emergency cannot be properly addressed without relying on the scientific knowledge possessed by these experts.
Yet, ultimately, U.S. government health experts have limited power. They work at the discretion of the White House, leaving their guidance subject to the whims of politicians and them less able to take urgent action to contain the pandemic.
The Centers for Disease Control and Prevention has issued guidelines only to later revise them after the White House intervened. The administration has also undermined its top infectious disease expert, Dr. Anthony Fauci, over his blunt warnings that the pandemic is getting worse – a view that contradicts White House talking points.
And most recently, the White House stripped the CDC of control of coronavirus data, alarming health experts who fear it will be politicized or withheld.
In the realm of monetary policy, however, there is an agency with experts trusted to make decisions on their own in the best interests of the U.S. economy: the Federal Reserve. As I describe in my recent book, “Stewards of the Market,” the Fed’s independence allowed it to take politically risky actions that helped rescue the economy during the financial crisis of 2008.
That’s why I believe we should give the CDC the same type of authority as the Fed so that it can effectively guide the public through health emergencies without fear of running afoul of politicians.
The paradox of expertise
There is a paradox inherent in the relationship between political leaders and technical experts in government.
Experts have the training and skill to apply scientific knowledge in complex biological and economic systems, yet democratically elected political leaders may overrule or ignore their advice for ill or good.
This happened in May when the CDC, the federal agency charged with controlling the spread of disease, removed advice regarding the dangers of singing in church choirs from its website. It did not do so because of new evidence. Rather, it was because of political pressure from the White House to water down the guidance for religious groups.
Similarly, the White House undermined the CDC’s guidance on school reopenings and has pressured it to revise them. So far, it seems the CDC has rebuffed the request.
The ability of elected leaders to ignore scientists – or the scientists’ acquiescence to policies they believe are detrimental to public welfare – is facilitated by many politicians’ penchant for confident assertion of knowledge and the scientist’s trained reluctance to do so.
Compare Fauci’s repeated comment that “there is much we don’t know about the virus” with President Donald Trump’s confident assertion that “we have it totally under control.”
Experts with independence
Given these constraints on technical expertise, the performance of the Fed in the financial crisis of 2008 offers an informative example that may be usefully applied to the CDC today.
The Federal Reserve is not an executive agency under the president, though it is chartered and overseen by Congress. It was created in 1913 to provide economic stability, and its powers have expanded to guard against both depression and crippling inflation.
At its founding, the structure of the Fed was a political compromise designed make it independent within the government in order to de-politicize its economic policy decisions. Today its decisions are made by a seven-member board of governors and a 12-member Federal Open Market Committee. The members, almost all Ph.D. economists, have had careers in academia, business and government. They come together to analyze economic data, develop a common understanding of what they believe is happening and create policy that matches their shared analysis. This group policymaking is optimal when circumstances are highly uncertain, such as in 2008 when the global financial system was melting down.
The Fed was the lead actor in preventing the system’s collapse and spent several trillion dollars buying risky financial assets and lending to foreign central banks – decisions that were pivotal in calming financial markets but would have been much harder or may not have happened at all without its independent authority.
The Fed’s independence is sufficiently ingrained in our political culture that its chair can have a running disagreement with the president yet keep his job and authority.
Putting experts at the wheel
A health crisis needs trusted experts to guide decision-making no less than an economic one does. This suggests the CDC or some re-imagined version of it should be made into an independent agency.
Like the Fed, the CDC is run by technical experts who are often among the best minds in their fields. Like the Fed, the CDC is responsible for both analysis and crisis response. Like the Fed, the domain of the CDC is prone to politicization that may interfere with rational response. And like the Fed, the CDC is responsible for decisions that affect fundamental aspects of the quality of life in the United States.
Were the CDC independent right now, we would likely see a centralized crisis management effort that relies on the best science, as opposed to the current patchwork approach that has failed to contain the outbreak nationally. We would also likely see stronger and consistent recommendations on masks, social distancing and the safest way to reopen the economy and schools.
Independence will not eliminate the paradox of technical expertise in government. The Fed itself has at times succumbed to political pressure. And Trump would likely try to undermine an independent CDC’s legitimacy if its policies conflicted with his political agenda – as he has tried to do with the central bank.
But independence provides a strong shield that would make it much more likely that when political calculations are at odds with science, science wins.