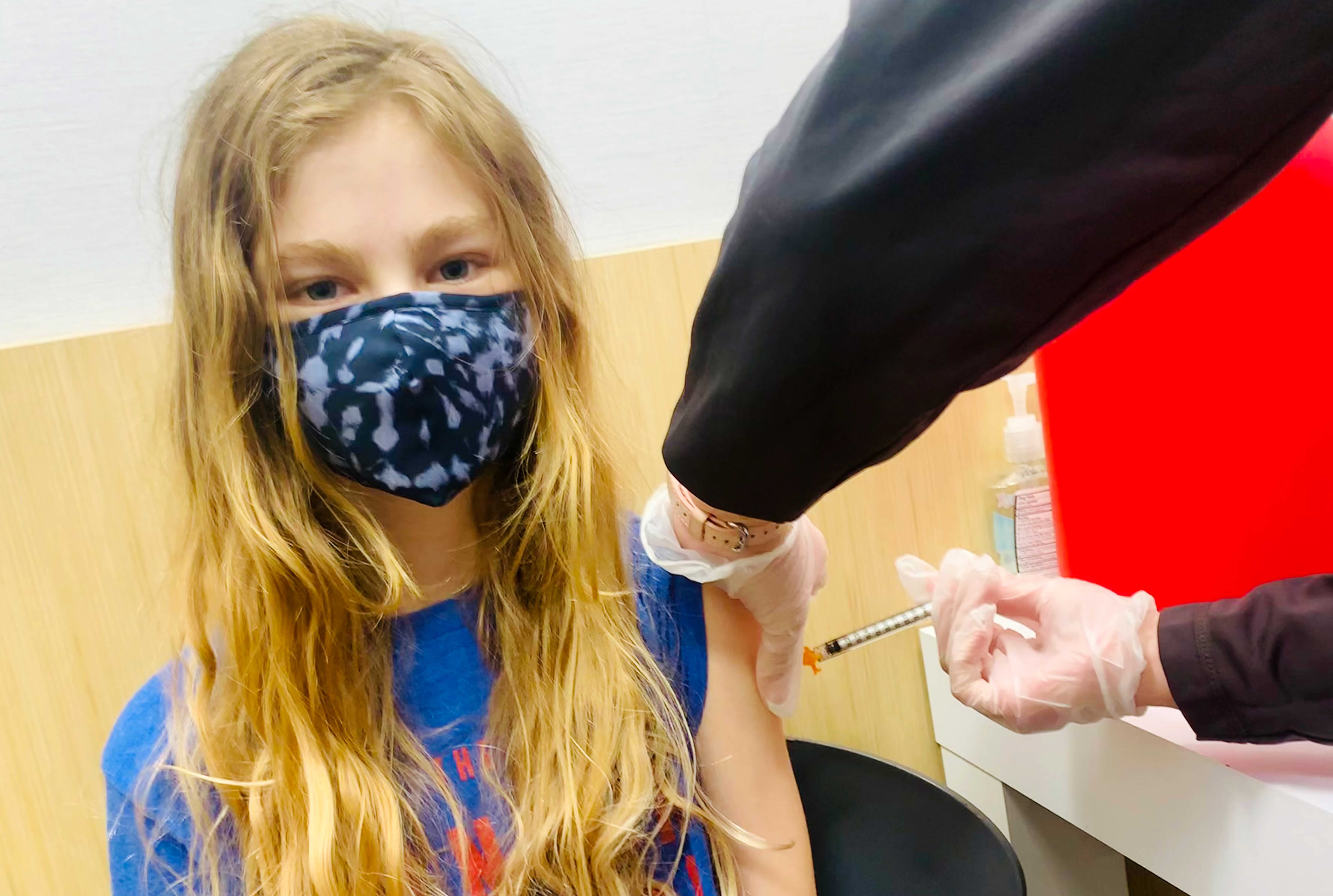
The COVID-19 pandemic revealed the need for substantial investment in public health. Journalist Anna Maria Barry-Jester, in an investigation published in California Healthline and the Los Angeles Times last week, reported that the need is pressing and that the time is ripe to formulate solutions.
“As we’ve continued to make progress in bringing the COVID-19 emergency under control, many California leaders are turning their attention to the future,” Barry-Jester wrote.
This year’s state budget set aside $3 million for an assessment of California’s public health infrastructure. “Public health leaders believe it will show that staffing and training are major issues,” Barry-Jester reported.
Starting in July 2022, annual state budgets will include $300 million to be spent to improve public health infrastructure.
The pandemic highlighted two significant public health needs in California. One is basic investment in public health infrastructure, as highlighted by Barry-Jester. The other is to address housing, diet, livable wages, and access to quality health care as part of an overarching public health strategy — a necessity highlighted by the stark racial, ethnic, and economic disparities among those who contracted and died from COVID-19.
Many Reasons for Staff Attrition
Before the pandemic, the state’s public health infrastructure already required shoring up. The COVID-19 crisis hammered the already underfunded and understaffed county and state public health systems.
In California, public health workers are leaving their jobs in droves. Counties are “losing experienced staffers to retirement, exhaustion, partisan politics, and higher-paying jobs,” Barry-Jester reported.
The exodus from public health predated this surge of resignations. Since the early days of the pandemic, experienced California public health leaders have been leaving the field, including 17 county public health officers and 27 county-level directors or assistant directors of public health. Both the director and the deputy director of the state’s department of public health resigned during the pandemic.
“Public health nurses, microbiologists, epidemiologists, health officers, and other staff members who fend off infectious diseases like tuberculosis and HIV, inspect restaurants, and work to keep communities healthy are abandoning the field,” Barry-Jester wrote. “The collective expertise lost with those departures is hard to overstate.”
Public health laboratories illustrate how much we rely on public health infrastructure for our everyday safety. The labs are largely invisible to the public but touch every aspect of daily life. “Public health labs sample shellfish to make sure it is safe for eating. They monitor drinking water and develop tests for emerging health threats such as antibiotic-resistant viruses. They also test for serious diseases, such as measles and COVID-19. And they typically do it at a fraction of the cost of commercial labs — and faster.”
Yet labs across the state are unable to hire and retain staff, and they are in danger of closing. “The biggest threat to [public health labs] right now is not the next emerging pathogen,” said Donna Ferguson, director of the public health lab in Monterey County, “but labs closing due to lack of staffing.”
Addressing Social Needs as Public Health Strategy
The pandemic highlighted the effects of income inequality and racial disparities on health in California. Data from the California Department of Public Health highlight the stark disparities in COVID-19 outcomes. The COVID-19 death rate for Latinx people is 19% higher than the statewide death rate, and the death rate for Black people is 16% higher. The case rate for Pacific Islanders is 45% higher than the statewide rate, while the rate of Pacific Islanders earning less than $40,000 annually is 33% higher than average.
Michael Goran, MD, professor of pediatric medicine at the University of Southern California, explained the connections among long-term health, social factors, and COVID-19 infection among Latinx people.
“There is an 80% higher rate of diabetes among Hispanics compared to non-Hispanic whites. We think early life nutrition is very important but also the environment where people live, which can include a combination of factors like poor access to healthy food, poor access to resources, air pollution, even chemical contaminants in the environment we found contribute to this disparity,” he told Los Angeles Times reporter Alejandra Reyes-Velarde.
These chronic diseases then put Latinx people at higher risk for worse COVID outcomes. “One of the most common recurring risk factors, not so much for rates of infection but the severity of the infection, is blood-glucose levels,” he said. “Individuals with higher blood-glucose levels seem to have a more severe response to COVID-19 infection, and of course, higher blood glucose is what contributes to diabetes.”
A Health Affairs study from the early days of the pandemic, which drew on data from California’s Sutter hospitals, noted that Black people are similarly at higher risk from the chronic illnesses that make people more susceptible to poor outcomes from COVID infections, including type 2 diabetes and congestive heart failure, as do other populations disproportionately harmed by COVID-19.
“Underfunded and Neglected”
A recent New York Times investigation highlights that California is not alone in dealing with a public health system pushed to the edge by the pandemic.
“Already underfunded and neglected even before the pandemic, public health has been further undermined in ways that could resound for decades to come,” wrote journalists Mike Baker and Danielle Ivory. The Times investigation of hundreds of health departments in all 50 states revealed that “local public health across the country is less equipped to confront a pandemic now than it was at the beginning of 2020.”
Threats, harassment, and anger directed at public health officials and workers drove many out of the field since the beginning of the pandemic and was identified as an ongoing problem by Baker and Ivory. “We have learned all the wrong lessons from the pandemic,” Adriane Casalotti told them. Casalotti is the chief of public and government affairs for the National Association of County and City Health Officials, an organization representing the nearly 3,000 local health departments across the nation. “We are attacking and removing authority from the people who are trying to protect us.”
Officials interviewed by Baker and Ivory noted that while additional funds are crucial to rebuilding public health departments, they aren’t sufficient to address the problems that have long weighed down the system or those that emerged during the pandemic.
Melissa Lyon, public health director for Erie County, Pennsylvania, put it this way: “If a ship is sinking, throwing treasure chests of gold at the ship is not going to help it float.”