
Hospital group wants prompt payment of 340B funds after Supreme Court win

The American Hospital Association wants HHS to act quickly to ensure that affected hospitals receive withheld 340B program funds.
The organization’s June 28 letter to HHS comes after the Supreme Court recently overturned a $1.6 billion 340B payment cut.
The case centered around whether CMS has the authority to make cuts to the program under its Medicare Outpatient Prospective Payment System. Under the payment rule, HHS cut the reimbursement rate for covered drugs by 28.5 percent in 2018, but it later lowered the cut to 22.5 percent. The Supreme Court reversed a federal appeals court’s 2020 ruling that HHS had the authority to make the $1.6 billion annual reimbursement cut.
“Given the vital role that 340B hospitals play in serving vulnerable communities, they should be repaid the funds that have been withheld from them without delay,” the American Hospital Association said in the letter. “They also should be paid for all of the years (2018-2022) in which the Centers for Medicare & Medicaid Services (CMS) illegally cut reimbursement rates.”
The hospital group said it is concerned that despite the Supreme Court’s decision, the resolution of these issues “could be bogged down in needless litigation, and that hospitals will not be appropriately compensated at a time when they are weathering significant financial challenges on many fronts.”
National Hospital Flash Report (June 2022)

Summary
U.S. hospitals and health systems continued to face difficult financial
and operational headwinds in May. Operating margins rose from April
but remained significantly lower than pre-pandemic levels and May 2021.
Volumes were up slightly from the previous month, with rising ED
visits close to numbers last seen in 2019 and earlier.
Gross operating revenues rose month-over-month and in comparison
to May 2021. But expenses — especially labor costs — were elevated
across nearly every metric month-over-month.
Margins
The median Kaufman Hall Year-To-Date (YTD) Operating Margin Index
reflecting actual margins was -0.33% through May.
The median change in Operating Margin was up 18.9% from last month
but down 45.6% from May 2021. The median change in Operating
EBITDA Margin was up 13.5% month-over-month, but down 36.1% from
May 2021.
Volumes
Patient volumes rose in May, with Length of Stay (LOS) up 2.3% from
April and 5.5% compared to May 2021. Patient Days increased by 4.8%
month-over-month but dropped 0.5% versus May 2021. Adjusted
Patient Days grew 3.5% from April to May and were 4% above May 2021
levels. Adjusted Discharges rose slightly, at 0.6% month-over-month,
but were down 0.3% compared to May 2021. Surgeries barely
fluctuated, with Operating Room Minutes down 1.0% from last month
and up just 0.1% YOY. Emergency Department (ED) Visits jumped 9.5%
from April to May and were up 4.5% YOY.
Revenues
Volume increases resulted in slightly improved revenue performance in
May. Gross Operating Revenue was up 3.4% from April and 7.6% YOY,
and is up 6.9% YTD. Similarly, Outpatient (OP) Revenue rose 2.2% from
April levels, 9.4% YOY and is up 9.1% YTD. Inpatient (IP) Revenue
climbed 3.5% from the previous month and 2.6% from May 2021, and is
up 4.2% YTD.
Expenses
Total Expenses continued to climb in May, rising 1.1% from April and
10.7% from May 2021. Inflation and labor shortages contributed to
total costs climbing 10.4% YTD.
Labor Expense per Adjusted Discharge inched up by 1.0% from April
and has surged 13.6% YTD, while Full-Time Employees Per Adjusted
Occupied Bed (FTEs per AOB), is down by 2.7% YTD, indicating that
hospitals are spending more on labor costs with fewer hours worked.
However, FTEs per AOB rose slightly in May, up 2.8% from April. Total
Expense per Adjusted Discharge increased by 0.3% from April, and
Labor Expense per Adjusted Discharge rose 1.0% from last month.
Non-Operating
The Federal Reserve raised its benchmark rate by 75 basis points in
mid-June, the most aggressive increase since 1994, as inflation hit a
40-year high of 8.6% in May. New projections show The Federal Open
Market Committee (FOMC) participants expect the Fed to raise rates to
at least 3% this year, with half indicating 3.375%. Labor metrics remain
strong with unemployment reading 3.6% in May and employers adding
390,000 new jobs.
Consumer sentiment hit a record low reading of 50.2 in early June,
comparable to the low point reached during the 1980 recession. US
equities ended May with marginal gains after weeks of volatile trading
due to economic data and corporate earnings sowing doubt over the
health of the US economy.
Takeaways at a Glance
- Nearly halfway through 2022, margins are cumulatively negative.
While some metrics have normalized, hospitals continue to perform below pre-pandemic levels,
and there is an uncertain outlook for the rest of the year. - Elevated labor costs remain a significant challenge.
Hospitals are still seeing higher labor costs and fewer hours worked, a sign of inflation and an
indicator that long-standing labor shortages are likely worsened by increased turnover. - Warmer temperatures and ED visits drove up volumes and revenues.
Patients often schedule elective procedures during the summer months, which may have
contributed to growing volumes. Emergency department visits also spiked this past month as
people spent more time outdoors. - Pent-up demand for hospital services also contributed to an increase in patients.
Sicker patients continued to schedule procedures they had previously postponed, suggesting
a return to normalcy as COVID-19 hospitalizations remained relatively low.
COVID vaccine strategy still murky after FDA experts meet
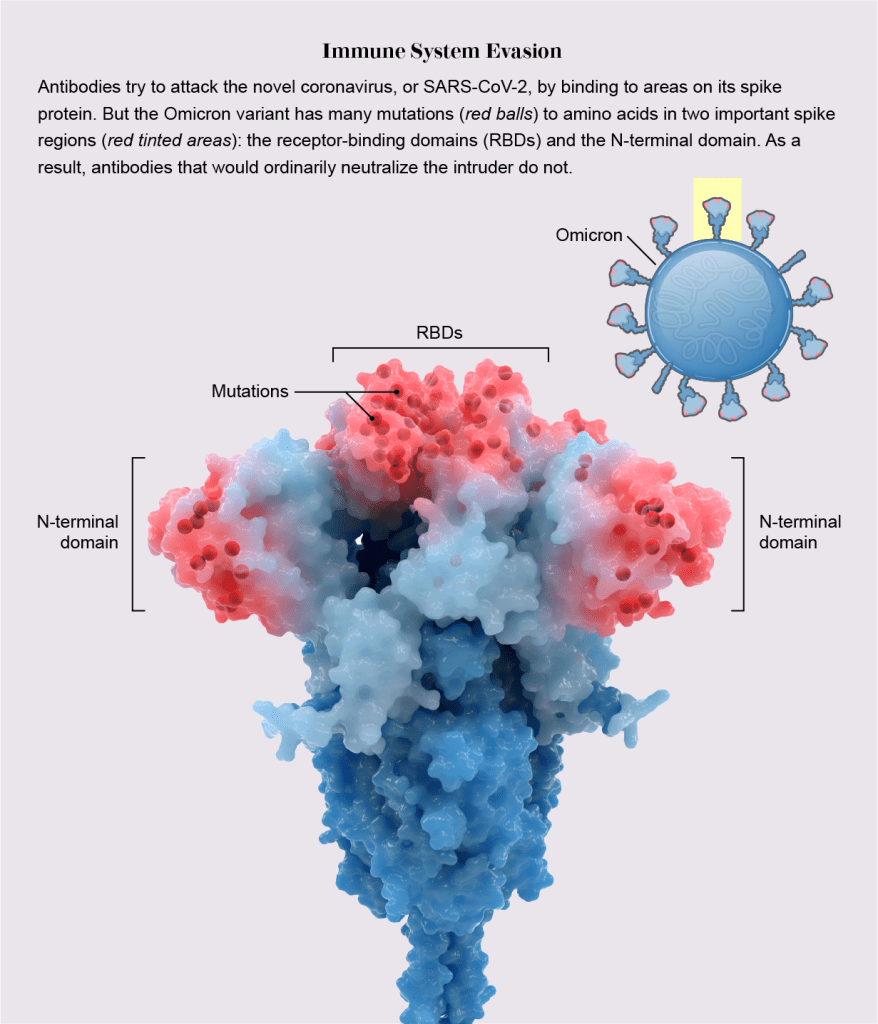
The COVID-19 vaccine strategy for the fall remains beset with unanswered questions after an FDA expert panel on Tuesday spent hours debating how and whether to update the shots.
Why it matters: Time is running short to develop a game plan with existing vaccines losing effectiveness against new variants and more than half of Americans still without a booster dose.
Driving the news: The Vaccines and Related Biological Products Advisory Committee voted 19-2 to recommend an Omicron-specific update to COVID-19 booster vaccines expected to be rolled out within the next few months.
But key questions were left unanswered:
- The panel didn’t formally decide whether to update shots with the prevalent Omicron strain in circulation, currently the fast-spreading BA.4 and BA.5 subvariants, or the BA.1 lineage that emerged late last year, as the World Health Organization recommended.
- The consensus appeared to be for a bivalent, or combination, booster combining the original COVID-19 strain that emerged in late 2019 with BA.4 and BA.5.
- The FDA will continue to evaluate what to do about the primary series of vaccines for the fall.
- Experts were split on whether there was enough data to recommend the updated shots for kids, or whether more studies are needed on dosage and possible side effects.
- There also were concerns about what effect an updated vaccine would have on developing nations’ willingness to use older COVID shots to inoculate their populations.
- And above all, it’s unclear whether all the questions about who gets which shot when will add to public confusion and apathy that’s dogged the vaccination effort in recent months.
What they’re saying: “None of us has a crystal ball and we’re trying to use every last ounce of what we can from predictive modeling and data that’s emerging to try to get ahead of a virus that’s very crafty,” said top FDA vaccine regulator Peter Marks.
- “Unfortunately, looking in the past doesn’t help us a great deal to look in the future for [a] virus that has baffled a lot of us and made predictions almost irrelevant,” said acting panel chairman Arnold Monto, a University of Michigan epidemiologist.
The timetable: Pfizer-BioNTech said an updated mRNA vaccine could be ready in October if regulatory uncertainties are ironed out. Moderna said it could have large amounts ready in late October or early November. Novavax is still awaiting emergency use authorization for its protein-based shot, but said it could have an updated vaccine by the fourth quarter.
It’s time to protect patients from short-term health plans
https://www.lls.org/advocate/protecting-patients-junk-insurance
Leukemia Lymphoma Society (LLS) supports actions that regulate or prohibit “junk insurance” plans that discriminate against people with pre-existing conditions, offer no meaningful coverage in the case of a cancer diagnosis or neglect to cover essential healthcare services like prescription drugs
The problem
LLS advocate Sam Bloechl thought he was doing everything right. After experiencing back pain that wouldn’t go away, he spoke to an insurance broker about upgrading his insurance plan to better cover any treatment he might need. Sam’s broker insisted she had the perfect plan for him. It wasn’t.
A month later, Sam was diagnosed with non-Hodgkin lymphoma. After chemotherapy and radiation, Sam achieved remission. But his health plan refused to cover the bill, leaving Sam with more than $800,000 in medical debt. It turns out he was sold a short-term, limited-duration plan—a type of “junk insurance.”
Sam isn’t alone. Patients with pre-existing conditions are penalized by low-quality policies, known as “junk insurance” Because such plans are exempt from important consumer protections, they can leave patients vulnerable when they most need timely access to quality, affordable care.
The patient impact
Most short-term, limited-duration plans leave patients on the hook for thousands of dollars if they face serious health problems—much more than they’d face if they had traditional health insurance, a recent Milliman study funded by LLS reveals. The plans often rely on misleading marketing and are misunderstood by consumers who buy them. And patients have no right to appeal plan decisions.
Moreover, junk plans drive up more than a patient’s out-of-pocket costs—they threaten prices across the health insurance market. As younger and healthier individuals choose these cheaper “junk plans” over comprehensive insurance, premiums for comprehensive insurance are expected to rise.
Solutions
LLS supports actions that regulate or prohibit “junk insurance” plans that discriminate against people with pre-existing conditions, offer no meaningful coverage in the case of a cancer diagnosis or neglect to cover essential healthcare services like prescription drugs. These plans include:
• Short-term, limited-duration insurance
• Health care sharing ministries
• Farm Bureau plans
• Grandfathered plans
• Multiple employer welfare arrangements and association health plans
• Spurious single-employer self-insured group health plans
• Minimum essential coverage-only plans
• Excepted benefit plans
A report published by 30 patient organizations, including LLS, explains these types of plans in depth—and details how state and federal lawmakers can help protect patients and consumers from these dangerous plans.
LLS works to stop policy proposals that would allow insurers to reinstitute lifetime limits, eliminate the current cap on patient cost-sharing and cover fewer essential services for cancer patients.
House hearing ups ante on Medicare Advantage reform

Political will seems to be growing to reshape the increasingly popular Medicare Advantage program.
At a House Energy and Commerce committee hearing on Tuesday, lawmakers on both sides of the aisle called for more oversight of MA following watchdog reports that found impediments to receiving covered care, including improper denials of prior authorization requests, and plans gaming the system in exchange for more funding from Medicare.
“Medicare Advantage is an important tool for helping seniors and we want it to succeed. We’re going to continue to conduct the oversight necessary,” said Oversight and Investigations Subcommittee Chair Diana DeGette, D-Colo.
Witnesses at the hearing — officials from the Government Accountability Office, HHS Office of Inspector General and congressional advisory board MedPAC — also pointed to higher rates of beneficiary disenrollment in their last year of life and opaque plan data, which can complicate oversight efforts.
Surveys have shown MA remains extremely popular with beneficiaries, attracted by lower co-pays and supplemental benefits like vision coverage and telehealth. In the program, Medicare pays private plans a capitated monthly rate to provide care for their beneficiaries based on the severity of their beneficiaries’ needs.
The hearing comes amid inflamed industry debate over the future of MA.
For-profit hospital lobby Federation of American Hospitals submitted a letter for the record sharing concerns over some MA plans denying patient care and having inadequate care networks.
Meanwhile, MA trade group Better Medicare Alliance sent a letter to the CMS on Monday urging the agency to safeguard the program as Congress mulls changes to Medicare.
But as Medicare’s hospital benefit — part of which funds MA — limps towards insolvency, lawmakers appear poised to target the growing MA program in a bid to crack down on improper payments and care denials.
“This is something that I think is very much bipartisan,” said Rep. Gary Palmer, R-Ala.
Coverage delays and denials
It’s not the first time lawmakers have zeroed in on MA oversight as a strategy to save Medicare money: In a Senate hearing on Medicare insolvency in February, Sen. Elizabeth Warren, D-Mass., said “the Medicare system is hemorrhaging money on scams and frauds” due to insurers taking advantage of the program’s rules to increase profits.
Even amid rising congressional criticism of MA, lawmakers on Tuesday reiterated their support for the program overall, which covered roughly 27 million Americans in 2021.
That’s more than a third of all Medicare beneficiaries, though MA is expected to swell to cover half of all Medicare members by 2030.
But lawmakers said they are increasingly concerned about disparities in the quality of coverage offered by Medicare Advantage plans compared to traditional Medicare plans, along with unscrupulous practices in the program resulting in higher reimbursement for MA organizations.
A GAO report found MA beneficiaries in their last year of life disenroll from MA in favor of traditional Medicare at a rate two times higher than other MA members, suggesting the plans may not support high-cost and specialized care, testified Leslie Gordon, GAO’s acting director for healthcare.
Gordon called it a “red flag” for the program that requires more scrutiny from CMS.
In addition, an HHS OIG report published April found MA organizations wrongly denied members care, with plans turning down 18% of payment requests that should have been approved.
Erin Bliss, OIG assistant inspector general in the Office of Evaluation and Inspection, testified plans sometimes use internal critical criteria that are not required by Medicare. In one example, an MA plan denied a medically necessary CT scan to diagnose a serious disease, citing that the patient hadn’t yet received an x-ray, Bliss said.
When appealed, plan denials were reversed 75% of time, a rate DeGette called “alarmingly high.”
“We are concerned that patients are receiving the timely care they need in those situations,” Bliss said.
OIG also found plans denied 13% of prior authorization requests that would have been approved under traditional Medicare.
Rep. Michael Burgess, R-Texas, suggested policymakers consider requiring insurers to forego prior authorization for doctors with a consistent track record of submitting accurate data. That strategy, called “gold carding,” is already used in some states, including Texas and West Virginia, to pare back on prior authorization delays.
MA payment reform
Along with coverage restrictions, lawmakers at Tuesday’s hearing asked witnesses about the scope and severity of improper MA payments in a bid to zero in on specific solutions Congress and the CMS can enact.
Though MA has potential to save the Medicare program money, “the current incentives for MA plans are not adequately aligned with the Medicare program,” said James Mathews, MedPAC executive director.
“Substantial reforms are urgently needed,” especially in light of Medicare’s “profound” financial problems, Mathews said.
In 2022, the average MA plan bid was 85% of fee-for-service spending, Mathews said. However, Medicare pays plans 104% of fee-for-service costs.
That imbalance is partially due to plans making patients appear sicker than they are to get extra payments from the government, witnesses said. The practice, called “coding intensity,” resulted in an estimated $12 billion in excess Medicare spending in 2020, according to MedPAC data.
Methods include chart reviews, where plans identify and add patient diagnoses that aren’t included in the service record, and health risk assessments, where plans contract with vendors to visit beneficiaries homes and conduct assessments, finding new diagnoses that often aren’t backed up by other records, according to Bliss.
GAO estimates that roughly a tenth of Medicare payments to MA plans in 2021 were improper, Gordon said.
To try to tamp down on coding intensity, the CMS should conduct targeted oversight of MA plans that routinely use these tools, and reassess whether chart reviews and in-home assessments are allowed to be sole sources of diagnoses for payment purposes, witnesses said. In addition, MA should improve care coordination for enrollees who receive health risk assessments.
The CMS should also consider replacing the quality bonus program and change its approach to calculating MA benchmarks, Mathews said.
In addition, the agency should require and validate data for completeness and accuracy before risk-adjusting payments through methods like medical record reviews, Gordon said.
Gordon also suggested the agency conduct more timely audits, as the CMS is currently missing out on recouping hundreds of millions of dollars in improper payments.
Policymakers appeared open witnesses’ suggestions to ensure MA is running as smoothly as possible, with Rep. Frank Pallone, D-N.J., calling for an additional hearing on the matter.
“This is bipartisan … You can be assured that we’re going to be following up,” DeGette said.
19 health systems with strong finances

Here are 19 health systems with strong operational metrics and solid financial positions, according to reports from Fitch Ratings, Moody’s Investors Service and S&P Global Ratings.
1. Morristown, N.J.-based Atlantic Health System has an “Aa3” rating and stable outlook with Moody’s. The health system has strong operating performance and liquidity metrics, Moody’s said. The credit rating agency expects Atlantic Health System to sustain strong performance to support capital spending.
2. Banner Health has an “AA-” rating and stable outlook with Fitch. The Phoenix-based health system’s core hospital delivery system and growth of its insurance division combine to make it a successful highly integrated delivery system, Fitch said. The credit rating agency said it expects Banner to maintain operating EBITDA margins of about 8 percent on an annual basis, reflecting the growing revenues from the system’s insurance division and large employed physician base.
3. Clearwater, Fla.-based BayCare has an “AA” rating and stable outlook with Fitch. The 14-hospital system has excellent liquidity and operating metrics, which are supported by its leading market position in a four-county area, Fitch said. The credit rating agency expects strong revenue growth and cost management to sustain BayCare’s operating performance.
4. CentraCare has an “AA-” rating and stable outlook with Fitch. The St. Cloud, Minn.-based system has a leading market position and solid operating margins, Fitch said. The credit rating agency said it expects CentraCare’s operating platform to remain strong.
5. Greensboro, N.C.-based Cone Health has an “AA” rating and stable outlook with Fitch. The health system has a leading market share and a favorable payer mix, Fitch said. The health system’s broad operating platform and strategic capital investments should enable it to return to stronger operating results, the credit rating agency said.
6. Franciscan Alliance has an “AA” rating and stable outlook with Fitch. The Mishawaka, Ind.-based health system has a very strong cash position and maintains leading market shares in seven of its nine defined primary service areas, Fitch said. The health system benefits from a good payer mix, the credit rating agency said.
7. Gundersen Health System has an “AA-” rating and stable outlook with Fitch. The La Crosse, Wis.-based health system has strong balance sheet metrics and a leading market position and expanding operating platform in its service area, Fitch said The credit rating agency expects the health system to return to strong operating performance as it emerges from disruption related to the COVID-19 pandemic.
8. Falls Church, Va.-based Inova Health System has an “Aa2” rating and stable outlook with Moody’s. The health system has a consistently strong operating cash flow margin and ample balance sheet resources, Moody’s said. Inova’s financial excellence will remain undergirded by its favorable regulatory and economic environment, the credit rating agency said.
9. Vineland, N.J.-based Inspira Health Network has an “AA-” rating and stable outlook with Fitch. The health system has strong operating performance, a leading market position in a stable service area and a growing residency program, Fitch said. The credit rating agency expects the system’s growing outpatient footprint and an increase in patient volumes to support its operating stability.
10. Oakland, Calif.-based Kaiser Permanente has an “AA-” rating and stable outlook with Fitch. The health system has a strong financial profile, and the system’s operating platform is “arguably the most emulated model” for nonprofit healthcare delivery in the U.S., Fitch said. By revenue base, Kaiser is the largest nonprofit health system in the U.S., and it is the most fully integrated healthcare delivery system in the country, according to the credit rating agency.
11. Mass General Brigham has an “Aa3” rating and stable outlook with Moody’s and an “AA-” rating and stable outlook with S&P. The Boston-based health system has an excellent clinical reputation, good financial performance and strong balance sheet metrics, Moody’s said. The credit rating agency said it expects Mass General Brigham to maintain a strong market position and stable financial performance.
12. Rochester, Minn.-based Mayo Clinic has an “Aa2” rating and stable outlook with Moody’s. The credit rating agency said Mayo Clinic’s strong market position and patient demand will drive favorable financial results. The health system “will continue to leverage its excellent reputation and patient demand to continue generating favorable operating performance while maintaining strong balance sheet ratios,” Moody’s said.
13. Methodist Health System has an “Aa3” rating and stable outlook with Moody’s. The Dallas-based system has strong operating performance, and investments in facilities have allowed it to continue to capture more market share in the fast-growing Dallas-Fort Worth, Texas, area, Moody’s said. The credit rating agency said it expects Methodist Health System’s strong operating performance and favorable liquidity to continue.
14. Traverse City, Mich.-based Munson Healthcare has an “AA” rating and stable outlook with Fitch. The health system has a strong market position, a good payer mix and robust cash-to-adjusted debt levels, Fitch said. The credit rating agency expects the system to weather an expected period of weakened operating cash flow margins.
15. Albuquerque, N.M.-based Presbyterian Healthcare Services has an “Aa3” rating and stable outlook with Moody’s and an “AA” rating and stable outlook with Fitch. Presbyterian Healthcare Services is the largest health system in New Mexico, and it has strong revenue growth and a healthy balance sheet, Moody’s said. The credit rating agency said it expects the health system’s balance sheet and debt metrics to remain strong.
16. Chicago-based Rush Health has an “AA-” rating and stable outlook with Fitch. The health system has a strong financial profile and a broad reach for high-acuity services as a leading academic medical center, Fitch said. The credit rating agency expects Rush’s services to remain profitable over time.
17. Stanford (Calif.) Health Care has an “AA” rating and stable outlook with Fitch. The health system has extensive clinical reach in a competitive market and its financial profile is improving, Fitch said. The health system’s EBITDA margins rebounded in fiscal year 2021 and are expected to remain strong going forward, the crediting rating agency said.
18. University of Chicago Medical Center has an “AA-” rating and stable outlook with Fitch. The credit rating agency said it expects University of Chicago Medical Center’s capital-related ratios to remain strong, in part because of its broad reach of high-acuity services.
19. University of Iowa Hospitals and Clinics has an “Aa2” rating and stable outlook with Moody’s. The Iowa City-based health system, the only academic medical center in Iowa, has strong patient demand and excellent financial management, Moody’s said. The credit rating agency said it expects the health system to continue to manage the pandemic with improved operating cash flow margins.
Stay Vigilant, CFOs: Your Compensation Strategy Matters More Than Ever

There’s been some speculation in the news lately that wage growth in the United States might be topping out. This could be the case for some employers, especially smaller companies that don’t have much more give in their current staffing budget. However, don’t think for a moment that compensation is suddenly losing its power as a tool to help secure top talent in a market where unemployment is low, the quits rate is high, and there are nearly twice as many open jobs as there are available workers.
The suggestion that employers are becoming more conservative in their salary offers also might be hopeful thinking for those trying to control rising inflation. Federal Reserve Chair Jerome Powell, for example, recently referred to the labor market as “unsustainably hot.”
While some big companies may be considering cooling down on hiring, some are paying higher wages to median-salaried employees than they did before the pandemic. (Significantly so, in some cases — think six figures.) And although the U.S. economy has seen some job-shedding in recent months, layoffs overall are at their lowest level on record.
The takeaway for chief financial officers (CFOs) is that you can’t afford to sit back and wait on wages. You can never really be sure when or if it will “top out,” especially in this unusual economy and candidate-driven hiring market. Your business needs to be prepared to provide standout compensation packages to hire stellar candidates — and keep your best people, too.
Compensation remains the not-so-secret weapon for besting competitors targeting the same talent, including the high performers who are already part of your organization. The trick is to use compensation as an offensive strategy that gives you more control. Following are three ways to help your organization make that pivot:
1. Review Current Employees’ Compensation Levels Now
While its name has been overexposed in the media, the Great Resignation is real and still in motion. Some are even referring to the phenomenon now as the “Forever Resignation”— a cycle of voluntary turnover that may never end. Buzzy labels aside, the pandemic has fundamentally changed the way people look at work, and what it means to them. They aren’t as willing to put up with things they don’t like about their job — like a low rate of pay. They know they have options, and they will seek them out.
Nearly two-thirds of U.S. workers who left their jobs in 2021 cited insufficient compensation as a reason for quitting, according to a Pew Research Center survey. To avoid turning your company’s valued staff into part of the “Class of 2022,” don’t wait for them to ask for a raise. Make sure to review their current compensation and if needed, bump it up, or extend another financial perk, like a spot bonus or paid time off.
And, if you find that employees are beating you to the punch, encourage an open discussion about pay. For example, if this person’s job responsibilities recently expanded or they’ve gained new skills, an immediate raise (or the promise of one soon) may be in order. If the employee is just feeling the crunch from inflation, offering a flexible work arrangement to reduce the burden of a costly commute might be an alternative solution for in-office workers.
2. Designate an Expert to Oversee the Compensation Process
In addition to taking stock of staff compensation levels as soon as possible, consider putting a formal process in place to ensure these levels will be monitored and adjusted proactively.
Compensation analysis will require, among other things, keeping tabs on the latest salary research and market trends, analyzing and updating job descriptions, and setting pay ranges and communicating them to staff. Look for someone in your human resources organization who could take the lead on managing this critical process. Because the market has changed so fast, it’s critical to keep continual tabs on what’s happening with pay rates and hiring dynamics for your company’s most mission-critical roles.
3. Watch Out for Pay Compression
The need to pay higher salaries to top candidates is in many cases resulting in new hires earning more than existing staff. Even small differences in pay between employees who are performing the same job, regardless of their skills or experience, can turn into big staffing headaches — namely, turnover. Feelings of resentment and disengagement can especially rise in the workforce when new hires with less experience are paid the same as, or more than, tenured employees in the same positions, or when individual contributors are paid more than their managers.
Inflation, competition for in-demand talent and the company’s failure to keep up with current market rates for compensation can all lead to pay compression. Conducting regular pay audits as described above and quickly bringing up the base salary of underpaid employees are solutions for resolving and, ideally, preventing, pay compression.
When raises aren’t an option, consider offering compelling non-monetary perks such as upskilling opportunities, better benefits, health and wellness programs, a more welcoming corporate culture, or all of the above.
That said, you can be sure that, no matter what, leading employers will continue to pay salaries that will attract the top talent they need to drive innovation and stay competitive.
Nonprofit hospitals face mounting financial pressures: 4 things to know

Not-for-profit hospitals and healthcare systems continue to face significant operating challenges as they attempt to keep revenues on pace with escalating operating expenses fueled by inflation, according to a June 27 report from S&P.
Highlights from the report:
- The first quarter of 2022 marked the toughest performance quarter on record for U.S. not-for-profit hospitals and health systems, highlighted by widespread inflationary pressures across the sector.
- High labor expenses are likely to cause sustained operating hurdles, and demands on cash flow combined with weaker investment market returns could reduce financial flexibility through the remainder of 2022 and into 2023.
- S&P notes that higher interest costs are likely to make borrowing options more expensive. Furthermore, the re-introduction of sequestration and the likely end of the public health emergency later this year will also have to be absorbed into cash flow.
- The regulatory environment is becoming tougher and eliminating mergers and acquisitions as an option for many providers. Given recent denials by the Federal Trade Commission and other regulatory agencies, this option may be increasingly difficult to deploy. If these denials affect organizations that are already struggling operationally, options could become increasingly limited for certain providers.
Read the full report here.
Former hospital executive convicted in $1.4B billing scheme

The former leader of a rural hospital chain has been convicted for his role in an elaborate pass-through billing scheme, the Justice Department announced June 27.
After a 24-day trial, Jorge Perez, 62, of Miami, was convicted of conspiracy to commit healthcare fraud and wire fraud, healthcare fraud and conspiracy to commit money laundering of proceeds greater than $10,000.
Prosecutors said Mr. Perez conspired with others to bill for $1.4 billion of medically unnecessary laboratory testing services. He used rural hospitals as billing shells to submit claims for services that were mostly performed at outside laboratories.
The evidence presented at trial showed that Mr. Perez and other defendants targeted and obtained control of financially distressed rural hospitals through management agreements and purchases. They targeted rural hospitals because they often get higher reimbursement rates for laboratory testing from private insurers, according to the Justice Department.
The defendants promised to save the rural hospitals from closure by turning them into laboratory testing sites, but instead billed for fraudulent laboratory testing. Through the scheme, Mr. Perez and others made it appear the laboratory testing was performed at the rural hospitals when, in most cases, it was done by outside testing laboratories owned by defendants, prosecutors said.
“After private insurance companies began to question the defendants’ billings, they would move on to another rural hospital, leaving the rural hospitals they took over in the same or worse financial status as before,” the Justice Department said. At least three of the hospitals were forced to close.
Ricardo Perez, 59, of Miami, was also convicted of conspiracy to commit healthcare fraud and wire fraud, healthcare fraud and conspiracy to commit money laundering of proceeds greater than $10,000 on June 27. He is Jorge Perez’s brother, according to Kaiser Health News.

