While healthcare is delivered locally, the business of healthcare
is regional, and the regions are only getting bigger. Hospital
and health system mergers alike have continued to shift from
local to regional, and the recently announced merger between Advocate Aurora
Health and Atrium Health clearly highlights that the regions are only getting
bigger.
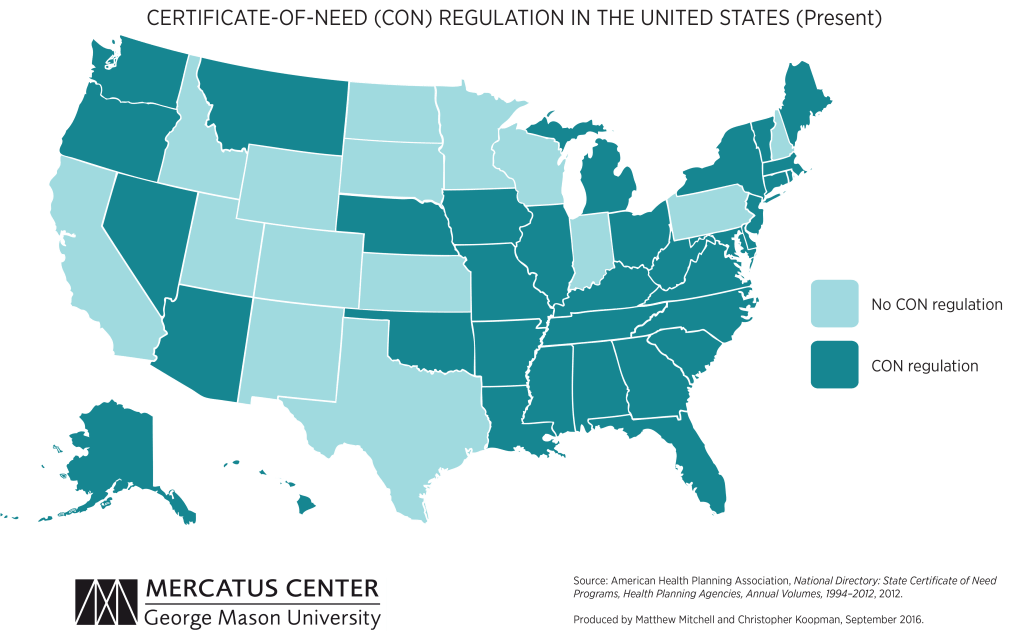
Advocate Aurora, with a presence in Illinois and Wisconsin, and Atrium Health,
with a presence in North Carolina, South Carolina, Georgia, and Alabama, will
combine to create a $27 billion health system that will span six states and make it
one of the leading healthcare delivery systems in the country. The combined
organization, which will transition to a new brand, Advocate Health, will operate
67 hospitals and over 1,000 sites of care, employ nearly 150,000 teammates, and
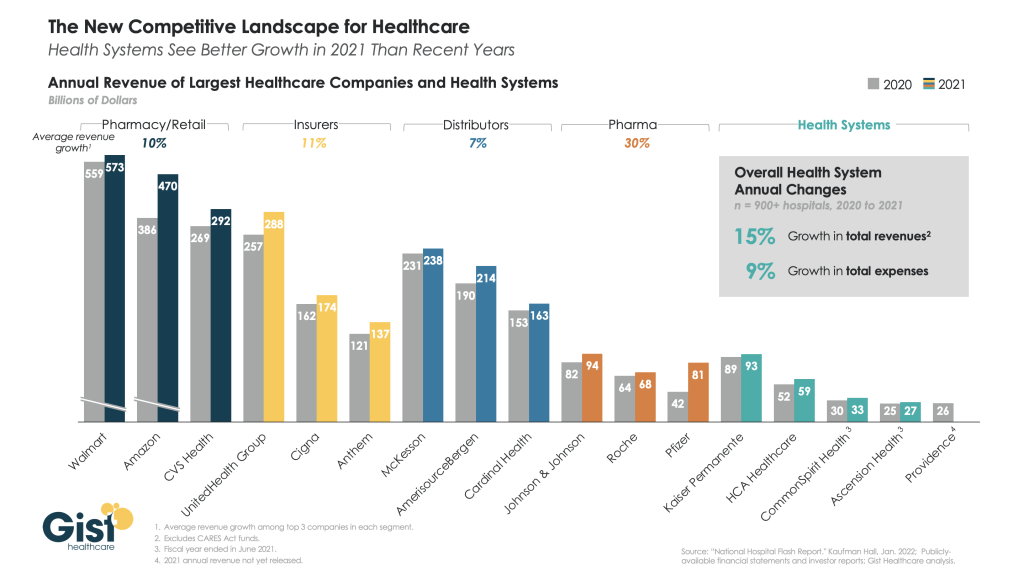
serve 5.5 million patients. Together, Advocate Health will become the 6th largest
system in the country behind Kaiser Permanente, HCA Healthcare, CommonSpirit
Health, Ascension, and Providence.
We have seen a number of large health systems come together recently,
including Intermountain Healthcare + SCL Health to create a $15 billion revenue
system, Spectrum Health + Beaumont ($14 billion), NorthShore University Health
System + Edward-Elmhurst Healthcare ($5 billion), LifePoint Health + Kindred
Healthcare ($14 billion), and Jefferson Health + Einstein Healthcare Network ($8
billion).
The exact reasoning for each merger differs slightly, but one of the common
threads across all is scale. But not scale in the traditional M&A sense. Rather,
scale in covered lives; scale in physician infrastructure and alignment; scale in
clinical and operational capabilities; scale in technology, innovation, and
partnerships with non-traditional players; scale for capital access; and scale for
insurance risk to compete in a value-based world. It is no longer the strong
acquiring the weak. Rather, strong players are coming together to gain scale to
face the headwinds in a unified manner.
For Advocate Aurora and Atrium, coming together is about leveraging their combined clinical excellence,
advancing data analytics capabilities and digital consumer infrastructure, improving affordability, driving health equity, creating a next-generation workforce, research, and environmental sustainability. Together, they have pledged $2 billion to disrupt the root causes of health inequities across underserved communities and create more than 20,000 new jobs.
Both Advocate Aurora and Atrium are no strangers to mergers. Advocate and Aurora came together in 2018, and prior to that Advocate was intending to merge with NorthShore before being blocked due to anti-trust. Atrium has grown over the years, merging with systems such as Navicent Health in Georgia in 2018, Wake Forest Baptist Health in North Carolina 2020, and Floyd Health System in Georgia in 2021. In the newly proposed merger, Advocate Aurora and Atrium are coming together via a joint operating arrangement where each entity will be responsible for their own liabilities and maintain ownership of their respective assets but operate together under the new parent entity and board. This may allow the combined entity more flexibility in local decision-making. The current CEOs, Jim Skogsbergh and Eugene Woods will serve as co-CEOs for the first 18 months, at which point Skogsbergh will retire, and Woods will take over as the sole CEO.
Mergers can come in various shapes and structures, but the driving forces behind consolidation are not unique. With the need to compete in value-based care, adequately manage risk, gain scale across covered lives, physicians, and points of access, successfully deliver affordable high-quality care, and the need to deal with the vertical and horizontal consolidation of the large-scale payers, the markets that health systems operate in must be large enough to be effective and relevant. We fully expect to see more of these larger scale health system mergers in the near term.
The physical delivery of healthcare is local, but, again, the business of healthcare is not; it is regional, and the regions are only getting bigger.