
Cartoon – Agreeing on the Numbers
Cartoon – Six Figure Return
Increasing denials, unfavorable payer mix among top RCM concerns: report
Revenue cycle challenges “seem to have intensified over the past year,” according to Kaufman Hall’s “2022 State of Healthcare Performance Improvement” report, released Oct. 18.
The consulting firm said that in 2021, 25 percent of survey respondents said they had not seen any pandemic-related effects on their respective revenue cycles. This year, only 7 percent said they saw no effects.
The findings in Kaufman Hall’s report are based on survey responses from 86 hospital and health system leaders across the U.S.
Here are the top five ways leaders said the pandemic affected the revenue cycle in 2022:
1. Increased rate claim denials — 67 percent
2. Change in payer mix: Lower percentage of commercially insured patients — 51 percent
3. Increase in bad debt/uncompensated care — 41 percent
4. Change in payer mix: Higher percentage of Medicaid patients — 35 percent
5. Change in payer mix: Higher percentage of self-pay or uninsured patients — 31 percent
CFOs experienced in cutting costs, restructuring in high demand

Fall is typically a period of increased CFO turnover as hospitals and health systems begin searches for new executives for the beginning of the following year, but the pressures associated with high inflation, a projected recession and the continued effects of the pandemic have led to more churn than usual for top financial positions, The Wall Street Journal reported Oct. 23
Many economists and financial experts are expecting a recession to hit the U.S. in early- to mid-2023. This is pushing some executives to switch roles now before the labor market changes. Many healthcare organizations are also preparing for a potential economic downturn by searching for CFOs who are experienced in cutting costs or restructuring operations, according to the report.
Recession planning in healthcare is challenging because it can have both negative (payer mix, patient volume) and positive effects (decrease in labor and supply inflation) on financial performance, according to Daniel Morash, senior vice president of finance and CFO for Boston-based Brigham and Women’s Hospital.
“The best advice I would give is that hospitals need to consider recession scenarios when making long-term commitments on wage increases, capital expenditures and planning for capacity for patient access,” Mr. Morash told Becker’s Hospital Review. “Most of our focus needs to be on the acute challenges we are facing. Still, it’s important to be careful not to overreact or overcommit financially when a recession could change a number of trends we’re seeing now.”
The Coming Insurance Storm
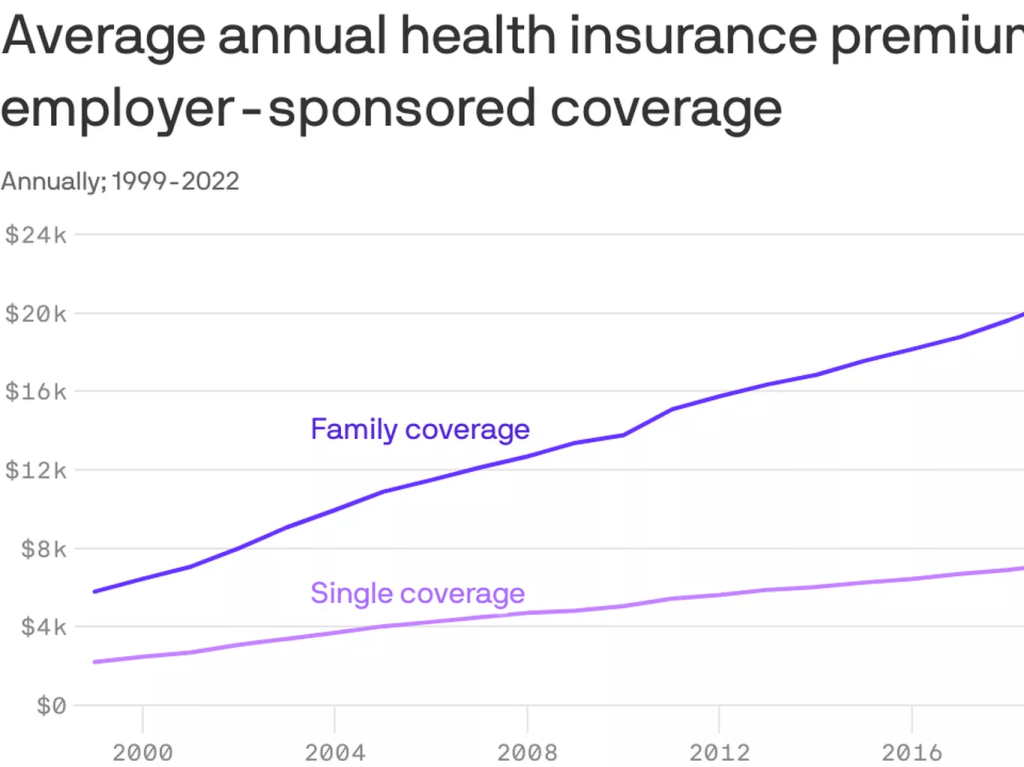
Employers face a brutal increase in health-insurance premiums for 2023, Axios’ Arielle Dreher writes from a Kaiser Family Foundation report out this morning.
- Why it matters: Premiums stayed relatively flat this year, even as wages and inflation surged. That reprieve was because many 2022 premiums were finalized last fall, before inflation took off.
“Employers are already concerned about what they pay for health premiums,” KFF president and CEO Drew Altman said.
- “[B]ut this could be the calm before the storm … Given the tight labor market and rising wages, it will be tough for employers to shift costs onto workers when costs spike.”
🧠 What’s happening: Nearly 159 million Americans get health coverage through work — and coverage costs and benefits have become a critical factor in a tight labor market.
- Premiums have increased by 20% over the past five years, KFF says in its annual Employer Health Benefits Survey.
🔎 Between the lines: In the tight labor market, some employers absorbed rising costs of coverage instead of passing them on to workers.
- An October survey of 1,200 small businesses found that nearly half had raised prices to offset rising costs of health care.
🧮 By the numbers: It cost an average of $22,463 to cover a family through employer-sponsored health insurance in 2022, KFF found.
- Workers contributed an average of $6,106.
U.S. economy returned to growth in Q3

The U.S. economy expanded at a 2.6% annual rate in the third quarter, ending the streak of back-to-back contractions that raised fears the country had entered a recession.
Why it matters: Gross domestic product got a boost from trade dynamics, but the underlying details — including weaker housing and decelerating consumer spending — point to an economy that’s slowing.
- The first estimate of GDP, released by the Commerce Department on Thursday, will be revised in the coming months as the government gets more complete data.
- The report comes on the heels of negative GDP growth during the first half of the year. In the January through March period, the economy contracted at a 1.6% annual rate. In the second quarter, the economy shrank at a 0.6% annualized pace.
Between the lines: The latest GDP report is among the final major economic data releases before the midterm elections, where voters have ranked the economy as a critical issue.
- The labor market is solid, with the unemployment rate at the lowest level in over 50 years. But soaring inflation has eaten away at Americans’ wage gains.
The backdrop: The Federal Reserve is trying to engineer an economic slowdown in a bid to crush high inflation. It has swiftly raised borrowing costs five times this year, with another big increase likely ahead at its upcoming policy meeting next week.
What they’re saying: “For months, doomsayers have been arguing that the US economy is in a recession and Congressional Republicans have been rooting for a downturn,” President Biden said in a statement. “But today we got further evidence that our economic recovery is continuing to power forward.”
Cartoon – Artificial Intelligence
Fitch: Nonprofit hospitals face prolonged labor challenges despite recent respite

Nonprofit hospitals are bracing for a challenging few months as healthcare and social assistance job vacancies remain high against a backdrop of low unemployment, Fitch Ratings said in an Oct. 25 update.
Healthcare and social assistance job openings fell for two consecutive months to 7.7 percent as of August, but the number of openings remains above the highest level recorded before the COVID-19 pandemic.
One encouraging sign is the slowly declining number of quits — 2.3 percent (486,000 quits) in August 2022 compared with a peak of 3.1 percent (626,000 quits) in November 2021. However, current quit rates remain high and are on track to exceed last year, according to Fitch.
“[not-for-profit] hospital quits will need to normalize to well below pre-pandemic levels in order to reduce staffing shortages and a reliance on contract/temporary labor,” Fitch Director Richard Park said in the news release.
The labor shortage saw hospital employees’ average weekly earnings increase 21.1 percent since February, significantly higher than the 13.6 percent earnings growth of overall private sector employees, according to Fitch. But ambulatory healthcare services employees’ earnings increased by only 12.6 percent over the same period.
“Wage increases and employee recruitment challenges may amplify the role of ambulatory care in the overall healthcare sector and continue the acceleration of inpatient care to outpatient settings,” Mr. Park said.
H.R.8800 – Supporting Medicare Providers Act of 2022

Due to the ongoing recess leading to the midterm elections, very important legislation introduced in September, H.R. 8800 – Supporting Medicare Providers Act of 2022, has stalled.
This critical, bipartisan legislation would stabilize Medicare for physicians and patients because it:
- Stops the 4.42% of the Medicare cuts related to the budget neutrality adjustment in the Medicare Physician Fee Schedule (MPFS), helping to buoy physician practices that are still recovering from the pandemic;
- Protects patients access to care, particularly in underserved communities; and
- Provides a commitment to long-term Medicare payment reform.




