
Cartoon – Thinking About Something Useful





https://www.washingtonpost.com/health/2021/12/28/nursing-home-hospital-staff-shortages/
At the 390-bed Terrace View nursing home on the east side of Buffalo, 22 beds are shut down. There isn’t enough staff to care for a full house, safely or legally.
That means some fully recovered patients in the adjacent Erie County Medical Center must stay in their hospital rooms, waiting for a bed in the nursing home. Which means some patients in the emergency department, who should be admitted to the hospital, must stay there until a hospital bed opens up. The emergency department becomes stretched so thin that 10 to 20 percent of arrivals leave without seeing a caregiver — after an average wait of six to eight hours, according to the hospital’s data.
“We used to get upset when our ‘left without being seen’ went above 3 percent,” said Thomas Quatroche, president and chief executive of the Erie County Medical Center Corp., which runs the 590-bed public safety net hospital.
Nursing home bed and staff shortages were problems in the United States before the coronavirus pandemic. But the departure of 425,000 employees over the past two years has narrowed the bottleneck at nursing homes and other long-term care facilities at the same time that acute care hospitals are facing unending demand for services due to a persistent pandemic and staff shortages of their own.
With the omicron variant raising fears of even more hospitalizations, the problems faced by nursing homes are taking on even more importance. Several states have sent National Guard members to help with caregiving and other chores.
Hospitalizations, which peaked at higher than 142,000 in January, are rising again as well, reaching more than 71,000 nationally on Thursday, according to data tracked by The Washington Post. In some places, there is little room left in hospitals or ICUs.
About 58 percent of the nation’s 14,000 nursing homes are limiting admissions, according to a voluntary survey conducted by the American Health Care Association, which represents them. According to the U.S. Bureau of Labor Statistics, 425,000 employees, many of them low-paid certified nursing assistants who are the backbone of the nursing home workforce, have left since February 2020.
“What we’re seeing on the hospital side is a reflection of that,” said Rob Shipp, vice president for population health and clinical affairs at the Hospital Association of Pennsylvania, which represents medical providers in that state. The backups are not just for traditional medical inpatients ready for follow-up care, he said, but psychiatric and other patients as well.
A handful of developmentally disabled patients at Erie County Medical Center waited as long as a year for placement in a group setting, Quatroche said. Medical patients recovered from illness and surgery who cannot go home safely may wait days or weeks for a bed, he said.
“I don’t know if everyone understands how serious the situation is,” Quatroche said. “You really don’t know until you need care. And then you know immediately.”
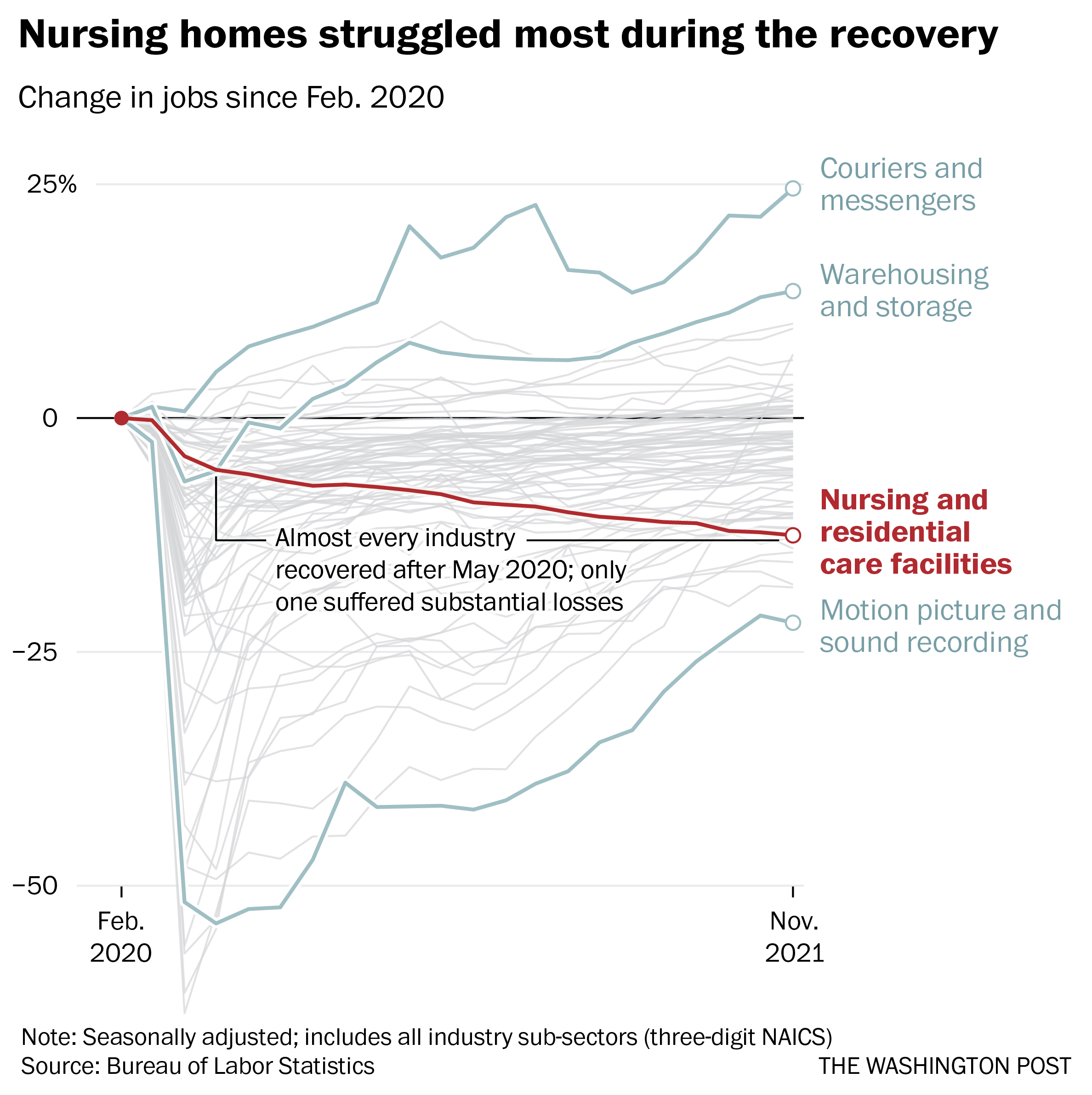
Remarkably, despite the horrific incidents of death and illness in nursing homes at the outset of the pandemic, more staff departures have come during the economic recovery. As restaurants and shops reopened and hiring set records, nursing homes continued to bleed workers, even as residents returned.

Nearly 237,000 workers left during the recovery, data through November show. No other industry suffered anything close to those losses over the same period, according to the Bureau of Labor Statistics.
Workers in the broader health-care industry have been quitting in record numbers for most of the pandemic, plagued by burnout, vulnerability to the coronavirus and poaching by competitors. Low-wage workers tend to quit at the highest rates, Labor Department data show, and nursing home workers are the lowest paid in the health sector, with nonmanagerial earnings averaging between $17.45 an hour for assisted living to $21.19 an hour for skilled nursing facilities, according to the BLS.
Nursing home occupancy fell sharply at the start of the pandemic, but inched back upward in 2021, according to the nonprofit National Investment Center for Seniors Housing and Care. One major force that held it back was worker shortages.

“Operators in the business have said we could admit more patients, but we cannot find the staff to allow that to happen,” said Bill Kauffman, senior principal at the organization.
Shortages have spawned fierce talent wars in the industry, Brookdale Senior Living Chief Executive Officer Cindy Baier said in a recent earnings call. When they don’t have enough workers, restaurants can reduce service hours and hospitals can cut elective surgeries, but nursing homes don’t have the option of eliminating critical services, she said. They must close beds.
“We are in the ‘people taking care of people’ business around-the-clock, 365 days a year,” she said.
Nursing homes tend to gain workers during a recession but can struggle to hire during expansions, according to an analysis of county-level data from the Great Recession recently published in the health care provision and financing journal Inquiry.
Steady income from their resident population and government programs such as Medicaid makes them recession-proof, and their low pay and challenging work conditions mean they’re chronically understaffed, said one of the study’s authors, Indiana University health-care economist Kosali Simon.
When recessions occur, nursing homes go on a hiring spree, filling holes in their staff with qualified workers laid off elsewhere.
“People during a recession may lose their construction jobs or jobs in retail sectors, and then look for entry-level positions at places like nursing homes where there is always demand,” Simon said.
Now, amid the “Great Resignation” and the hot job market, the opposite is happening. In sparsely populated areas and regions where pay is lower, the problem is even worse.
The Diakonos Group, which operates 26 nursing homes, assisted-living facilities and group homes in Oklahoma, closed an 84-bed location for seniors with mental health needs in May “simply because we couldn’t staff it any longer,” said Chief Executive Officer Scott Pilgrim. Patients were transferred elsewhere, including Tulsa and Oklahoma City, he said.
The home in rural Medford, which depended entirely on Medicaid payments, “was never easy to staff, but once we started through covid and everything, our staff was just burned out.”
Diakonos boosted certified nursing assistants’ pay from $12 an hour and licensed practical nurses’ pay from $20 an hour, used federal and state assistance to offer bonuses and employed overtime, but workers kept leaving for better health-care jobs and positions in other industries, he said.
“I’ve never been able to pay what we ought to pay,” Pilgrim said. Eventually he began to limit admissions and eventually was forced to close.
“The hospitals are backed up,” he said. “They’re trying to find anywhere to send people. We get referrals from states all around us. The hospitals are desperate to find places to send people.”
In south central Pennsylvania, SpiriTrust Lutheran is not filling 61 of its 344 beds in six facilities because of the worker shortage, said Carol Hess, the company’s senior vice president.
“I have nurses who went to become real estate agents,” she said. “They were just burned out.”
Pay raises of $1 to $1.50 an hour and bonuses brought the lowest-paid workers to about $15 an hour, Hess said, and the company is planning a recruiting drive after Jan. 1. But the prognosis is still grim.
“We’re competing with restaurants for our dining team members,” Hess said. “We’re competing with other folks for cleaning and laundry and others.” In the area around Harrisburg where SpiriTrust employees live, some schools that turned out certified nurse assistants closed during the pandemic and haven’t reopened.
The nursing homes have begun borrowing licensed practical nurses from WellSpan Health, the nearby hospital system that discharges many of its patients to SpriTrust after they recover. About 15 have began their orientations this month, she said, and the two systems are collaborating to pay them.
The bed shortage is causing backups that can average several days in the hospital, said Michael Seim, the hospital system’s chief quality officer. That gives the hospitals an interest in helping any way they can, he said.
“We have between 80 and 100 patients waiting for some type of skilled care,” Seim said this month. The hospital has begun caring for more people at home, enrolling 400 people so far in a program that sends clinicians to check on them there. More than 90 percent have said they are happy with the program.
“I think the future of hospital-based care is partnerships,” Seim said. “It’s going to be health systems partnering across their service areas … to disrupt the model we have.”
https://www.washingtonpost.com/health/2021/12/28/omicron-how-severe-us/

Healthy individuals who have been vaccinated, and especially those who have been boosted, appear unlikely to develop severe infections from the omicron variant that would land them in the hospital, say medical experts who have monitored the effects of the newest coronavirus variant since it was identified over four weeks ago.
While omicron has sent U.S. infections soaring to levels not seen since last winter’s wave, it appears to have less severe effects than the delta variant, according to a handful of international studies and early data from several U.S. hospitals.
Those infected by the omicron variant are 15 to 20 percent less likely to go to an emergency room, and 40 percent less likely to be hospitalized overnight, compared with those infected with delta, according to English data analyzed by scientists from Imperial College London. That aligns with early U.S. data from some hospitals.
At the Houston Methodist hospital system, about 15 percent of symptomatic individuals have ended up hospitalized — around a 70 percent reduction compared with those infected by the delta variant, said James Musser, chair of pathology and genomic medicine.
A separate study from Britain, which is not yet peer reviewed, found that people infected with omicron were almost 60 percent less likely to enter the hospital than those infected with delta.
“What is absolutely clear is there is lower rate of hospitalization with our omicron patients in our hospital system,” Musser said. “That does not necessarily mean that this variant is quote-unquote ‘less virulent.’ The jury’s still out on that. What we know now is that … if you are immunized and, more importantly, if you are boosted, you’re going to stay out of substantial trouble.”
He and other experts warn against complacency, however, cautioning that millions of Americans, particularly the unvaccinated, remain vulnerable to more serious disease from the most transmissible coronavirus variant to date.
Other factors that might lead to greater risk include an individual’s age, the type of vaccine or booster they received, and whether they have underlying health problems, such as heart disease or obesity, said Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota and a member of President Biden’s covid-19 transition task force.
“Have you previously had infection? Were you vaccinated? How many doses of vaccine, and was it more than six months ago? So in some ways this is almost like a calculus problem. It’s got a lot of moving parts to it and we’re trying to figure it out,” Osterholm said.
Doctors also caution that far more people will become infected with omicron simply because of its transmissibility. If even a small fraction of those land in the hospital, they worry that health care systems that are already short-staffed because of delta infections could be overwhelmed — with potentially dire results for those needing critical care as a result of car accidents, heart attacks, strokes, or any number of things that bring people to emergency rooms.
“We need to be respectful of the fact that our hospital system has been under this kind of duress for such a long time,” said Larry Corey, a virologist at the Fred Hutchinson Cancer Research Center in Seattle. “We need to do everything we can to not allow the situation, where there’s such crowding and such intensity that we can’t optimally take care of the people who get severe disease.”
Anthony S. Fauci, Biden’s chief medical adviser, said the rapid increase in the numbers of people getting infected with the omicron variant will invariably put additional strain on the system.
“We’re going to have a real challenge to the health-care delivery system — namely the number of beds, the number of ICU beds and even the number of health care providers,” Fauci said in an interview. “Even vaccinated people are getting breakthrough infections. So if you get enough nurses and doctors infected, they are going to temporarily be out of action. And if you get enough of them out of action, you could have a double stress on the health care system.”
The welcome news for most people who are vaccinated and boosted is that omicron infections often mimic the symptoms of the common cold. Those with two shots of vaccine, but no booster, also appear to fare relatively well, though they may develop more intense symptoms that may last longer, experts said.
Of the 205 million Americans who have been vaccinated, about 66 million, or 32 percent, have received a booster dose, according to the Centers for Disease Control and Prevention.
In a series of Twitter posts, Craig Spencer, who teaches emergency medicine at Columbia University Medical Center, said every boosted patient he has seen in the emergency room has had no difficulty breathing or shortness of breath. Those who have had two doses of either the Pfizer or Moderna vaccines also have had mild symptoms, he said, “but more than those who had received a third dose.”
But almost every patient who had to be hospitalized was unvaccinated, he said.
“No matter your political affiliation, or thoughts on masks, or where you live in this country, as an ER doctor you’d trust with your life if you rolled into my emergency room at 3am, I promise you that you’d rather face the oncoming Omicron wave vaccinated,” Spencer wrote.
Children are also filling up hospital beds in many parts of the country, especially in New York. State officials issued a warning on Christmas Eve after a fourfold increase in hospitalizations in children under 18 in New York City between Dec. 5 and last week. About half of the admissions were children under 5, who are not eligible for vaccination, according to the New York Department of Health.
Experts cautioned that those at higher risk of severe infection to previous variants probably remain vulnerable to this one.
It’s not yet clear whether older, boosted individuals and those with underlying conditions, such as diabetes and heart disease, face the same lowered risk with omicron. Answering such questions is key to assessing the likely trajectory of the variant in the U.S. since it is older and less healthy than many of its global peers.
So far, though, early U.S. data echoes what has been seen in South Africa and Britain, where omicron waves are slightly ahead of this country’s.
A group of Scottish scientists said recently that vaccinated people appear to have some protection against symptomatic infection from omicron, although less than they did against delta. A third dose or booster of an mRNA vaccine was associated with a 57 percent reduction in the odds of developing a symptomatic omicron case.
In the Johns Hopkins Hospital emergency department, physicians are seeing more infections than atany other point in the pandemic, but most of the cases are not severe, said Stuart Ray, a professor of medicine in the division of infectious diseases. But he warned that there is not yet “reassuring evidence” the United States will be spared from a disruptive wave of infections and complications.
The country faces other challenges with omicron in terms of its medicine cabinet. Two of the three existing intravenous treatments called monoclonal antibodies — those from Regeneron and Eli Lilly — do not work against the variant. Some Republican governors had touted the ability of those with covid-19 to receive monoclonal antibodies, spurring some Americans to see those treatments as an alternative to getting vaccinated.
The only monoclonal antibody that does work, sotrovimab from Vir Biotechnology and GlaxoSmithKline, is in short supply and will not be available to many of those who become infected. The Food and Drug Administration authorized two easy-to-take antiviral pills last week and one has high efficacy against omicron, but it will be in initial short supply. Distribution of the pills is expected to begin shortly.
It is also unclear whether the surge in the United States will follow the same pattern as South Africa’s, which rapidly passed the peak of omicron cases last week.
South Africa’s population is significantly younger and has far lower vaccination rates, with about 35 percent of the population immunized, and virtually no oneboosted.The country also grappled with a delta variant wave that infected a far greater portion of the population than it did in the United States.
The significant number of South African residents infected with delta compared with the United States could prove to be an important distinction that might make more Americans vulnerable to omicron, said Chris Beyrer, an epidemiologist at the Johns Hopkins Bloomberg School of Public Health.
Beyrer also noted that infections in the United States, Britain and Germany seemed to be increasing at a significantly faster rate than they were in South Africa.
“This is an incredibly infectious virus and it is moving right along,” Beyrer said. He added that the United States has numerous tools — including ready access to vaccines and booster shots, the new antiviral medicines, testing and masking — that could help curb its effects.
But referring to those who have refused to follow public health guidelines, Beyrer said, “We have a lot of resistance so that makes us vulnerable to infection.”

The number of children with covid-19 recently hospitalized in New York City has increased by nearly five times this month, state officials said at a news conference Monday.
For the week from Dec. 5, 22 children with covid-19 were admitted to hospitals in the city. During a five-day period beginning on Dec. 19, that figure rose to 109, reflecting a broader national surge in coronavirus infections driven in part by the omicron variant. Daily case counts in recent days have climbed to levels not seen since last winter, when coronavirus vaccines weren’t widely available, though the total number of hospitalizations is still significantly lower.
The increase in pediatric covid patients in New York City has been mirrored nationwide. As of last week, nearly 2,000 confirmed or suspected pediatric covid patients were hospitalized nationally, a 31 percent jump in 10 days.
New York City officials are hoping a city mandate that took effect Monday requiring workers at an estimated 184,000 businesses to get at least one vaccine dose will curb infections. “We need more and more people vaccinated,” Mayor Bill de Blasio (D) told reporters. “We need to keep doubling down on vaccination to get out of the covid era once and for all.”
De Blasio’s office announced the mandate earlier this month, just days after health officials disclosed the first case of the more transmissible omicron variant in the United States. But the mayor leaves office in a few days. Kathryn Wylde, president of the Partnership for New York City, a major corporate advocacy group, said she hopes Mayor-elect Eric Adams (D) will show flexibility in enforcement, the Associated Press reported.
Roughly 92 percent of the city’s adult population has received at least one dose of a vaccine, municipal data show, while 83 percent of adults are considered fully immunized. Youth vaccination rates remain lower: Nearly half the children ages 5 to 17 have not yet received a single dose, according to the city government.
Experts say COVID-19 cases don’t tell whole story
For nearly two years, Americans have looked carefully at coronavirus case numbers in the country and in their local states and towns to judge the risk of the disease.
Surging case numbers signaled growing dangers, while falling case numbers were a relief and a signal to let one’s guard down in terms of gathering with friends and families and taking part in all kinds of events.
But with much of the nation’s population vaccinated and boosted and the country dealing with a new COVID-19 surge from omicron — a highly contagious variant that some studies suggest may not be as severe as previous variants — public health officials are debating whether the nation needs to shift its thinking.
Many people are going to get omicron — but those that are vaccinated and boosted are unlikely to suffer dire symptoms.
As a result, hospitalizations and deaths are the markers that government officials need to monitor carefully to ensure the safety of communities as the nation learns to live with COVID-19.
“This is the new normal,” said Leana Wen, a public health professor at George Washington University and former Baltimore health commissioner. “This is what we will have to accept as we transition from the emergency of COVID-19 to living with it as part of the new normal.”
David Dowdy, an epidemiologist at Johns Hopkins Bloomberg School of Public Health, said that Americans all need to shift to focus on hospitalizations over cases as we enter into another year of the pandemic.
“I think that we need to start training ourselves to look, first of all, at hospitalizations. I think hospitalizations are a real-time indicator of how serious things are,” he said.
Rising case numbers still say something about the disease, and the spikes from omicron are leading to real concerns.
Anthony Fauci, the government’s top infectious disease expert, noted on Sunday that even if omicron leads to less severe cases of COVID-19, if it infects tens of millions it will have the potential of straining resources in hospitals.
“If you have many, many, many more people with a less level of severity, that might kind of neutralize the positive effect of having less severity when you have so many more people,” he said during an appearance on ABC’s “This Week.”
At the same time, the nation must get used to dealing with the coronavirus as it would deal with an annual flu season. It’s a challenge for most parts of American life, from schools and businesses that have to consider worker and student safety, to professional sports leagues that must decide how long someone sits out after a positive test — even if the person is vaccinated and not symptomatic.
“Omicron in a way is the first test of what it means to live with COVID-19,” said Wen. “And by that I mean we are going to see many people getting infected but as long as our hospital systems are not overwhelmed and as long as vaccinated people are generally protected against severe outcomes, that is how we end the pandemic phase and switch into the endemic phase.”
The omicron strain is so infectious that once the current surge has faded in the United States, it’s likely a large majority of the population will either have been vaccinated against COVID-19 or have been infected, experts say. At that point, the focus should shift away from preventing infection to preventing serious illness, multiple experts said, a message already being echoed in some corners of the White House.
Many states have been seeing staggering numbers of positive tests and lines for COVID-19 testing that stretch for several blocks. Washington, D.C., and New York state have set records in recent days for the number of new cases reported as omicron barrels through the population.
But even with case totals surpassing last year’s numbers, President Biden and White House officials have been quick to point out that hospitalizations haven’t been as high as the numbers seen in the winter of 2020.
“Because we have so many vaccinated and boosted, we’re not seeing hospitalizations drive as sharply as we did in March of 2020 or even this past fall. America has made progress; things are better,” Biden said on Monday on a White House COVID-19 response team call with the National Governors Association to discuss the administration’s response to the omicron variant.
“But we do know that with rising cases, we still have tens of millions of unvaccinated people and we’re seeing hospitalizations rise,” he added, saying that some hospitals are going to get overrun both in terms of equipment and staff.
The White House pointed to Biden’s remarks last week when asked about whether the president wants Americans and health experts to take the emphasis off of case numbers and put it on hospitalizations.
“Because omicron spreads so easily, we’ll see some fully vaccinated people get COVID, potentially in large numbers. There will be positive cases in every office, even here in the White House, among the vaccinated … from omicron. But these cases are highly unlikely to lead to serious illness,” Biden said on Dec. 21.
Chief of staff Ron Klain on Monday retweeted a CNN report about how hospitalizations are about 70 percent less than what they were around the last peak in September, but that COVID-19 cases in unvaccinated Americans could end up overwhelming health systems.
Health experts have suggested the White House’s shift in messaging away from a focus on the number of cases is a sign of what’s to come as the pandemic eventually becomes endemic.
“For two years, infections always preceded hospitalizations which preceded deaths, so you could look at infections and know what was coming,” Ashish Jha, dean of the Brown University School of Public Health, said Sunday on ABC. “Omicron changes that. This is the shift we’ve been waiting for in many ways.”
Dowdy said positive tests are also up because people are getting tested before visiting relatives.
“If a lot of people are testing positive because they are asymptomatic and wanting to make sure that they can travel etc., having a lot of those kinds of cases is not a big problem,” he said.
“In fact, that’s a good thing. It means that we’re doing the right thing as a country to define those cases,” Dowdy added.
Lawrence Gostin, a professor of global health at Georgetown University, said the shift away from tracking case numbers as a way to measure the pandemic means devoting more resources toward treatment options like the Pfizer antiviral pill.
Gostin also said testing should increasingly be used to self-diagnose so individuals can get proper treatment, rather than testing for the purpose of stopping the spread of the virus.
“The White House has got a very difficult balancing act. Certainly for now it’s going to have to emphasize the idea of masking and distancing for the purpose of protecting the health system,” Gostin said.
“We can’t live our lives in a bubble to prevent us from getting a pathogen that’s so contagious that you can’t avoid it if you’re going to be circulating and living a life in this world,” he continued. “What it means to transition to a normal life or more normal life is you have to focus not so much on preventing cases, but on preventing hospitalizations and deaths.”

Another challenging year defined by the continued COVID-19 fight and vaccination drives has created a unique healthcare landscape. Pandemic-induced telehealth booms, continued strain due to understaffing and pressure from big tech disruptors are just some of the issues that have presented themselves this year.
Here are five major trends that hospitals and health systems may see in 2022. While some present challenges, others present significant opportunities for healthcare facilities.
Workforce pressure
Record numbers of workers have quit their jobs in 2021, with some 4.4 million people quitting in September. That means that 1 in 4 people quit their jobs this year across all industries. Around 1 in 5 healthcare workers have left their positions, creating issues with understaffing and lack of resources in hospitals and health systems. Stress, burnout and lack of balance have all been cited as reasons for staff leaving their roles. An increase in violence toward medical professionals, continued COVID-19 surges and low pay and benefits have contributed to the exodus of healthcare workers. None of those problems seems poised to disappear come 2022, so the new year could bring continued workforce and staffing challenges.
Pressure from disruptors
Big tech and retail giants have continued their push into healthcare this year. Companies like Apple, Amazon and Google stepped up their game in the wearables market. Pharmacy and retail chains Walmart and CVS Health both detailed their intended expansions into primary care. The pandemic also encouraged big corporations outside the healthcare sector, like Pepsi and Delta Airlines, to consider hiring CMOs to make sense of public health regulations guide them on their policy. These moves all mean there is a tightening of competition for the top physicians and hospital executives. Going into 2022, health systems may be under pressure to hang onto top talent and keep patients from using other convenient health services offered by retail giants.
Health equity
The unequal toll of the pandemic on people of color both medically and economically helped shed a light on the rampant inequities in American healthcare and society at large. Indigineous, Black and Hispanic people were much more likely than white or Asian people to suffer severe illness or require hospitalization as a result of COVID-19. Increasing numbers of hospitals, health systems and organizations are starting initiatives to advance health equity and focus on the socioeconomic drivers of health. The American Medical Association launched a language guide to encourage greater awareness about the power of language. Z-code usage has also been encouraged by CMS to increase knowledge and data about the social determinants of health. Next year, the perspective of health as holistic instead of just a part of an individual’s life will continue, with special attention being paid to social drivers.
Telehealth expansion
The pandemic helped the telemedicine industry take off in a big way. Telehealth was often the only healthcare option for many patients during the height of the lockdown measures introduced during the pandemic. Despite a return to in-person visits, telehealth has retained its popularity with patients. Some advocates argue that telehealth can help increase access to healthcare and improve health equity. About 40 percent of patients said that telehealth makes them more engaged and interact more frequently with their providers. However, while Americans see telehealth as the future of healthcare, a majority still prefer in-person visits. Regardless of patient opinion, telehealth will remain a key part of health strategy. In late December, the FCC approved $42.7 million in funding for telehealth for 68 healthcare providers. This suggests that there are investments and subsidies available in the future for health systems to bolster their telehealth services.
Climate change
At the 2021 UN Climate Conference, Cop26, in Glasgow, Scotland, hospitals and health systems acknowledged the role they have to play in mitigating the effects of climate change. Hospitals and health systems shed light on the health-related effects of climate change, such as illness and disease from events like wildfires and extreme weather. Health systems are also becoming more aware of their own contributions to climate change, with the U.S. healthcare system emitting 27 percent of healthcare emissions worldwide. To that end, HHS created an office of climate change and health equity that will work alongside regulators to reduce carbon emissions from hospitals. More health systems too are taking charge and pledging net neutrality and zero carbon emissions goals, including Kaiser Permanente and UnitedHealth group. It’s expected that more systems will follow suit in the coming year and make more concrete plans to address emissions reduction.