Cartoon – Yes We need to Talk

Cartoon – Budget Defined

Cartoon – This Year’s Budget

Cartoon – Budgeting Decisions

Importance of Honor
The magic of 70% and masks.

This chart shows that once 70% of the population gets at least one shot and mask compliance is very good: you can beat this virus.
What strategies will help to deliver telemedicine “at scale”?
https://mailchi.mp/72a9d343926a/the-weekly-gist-september-24-2021?e=d1e747d2d8
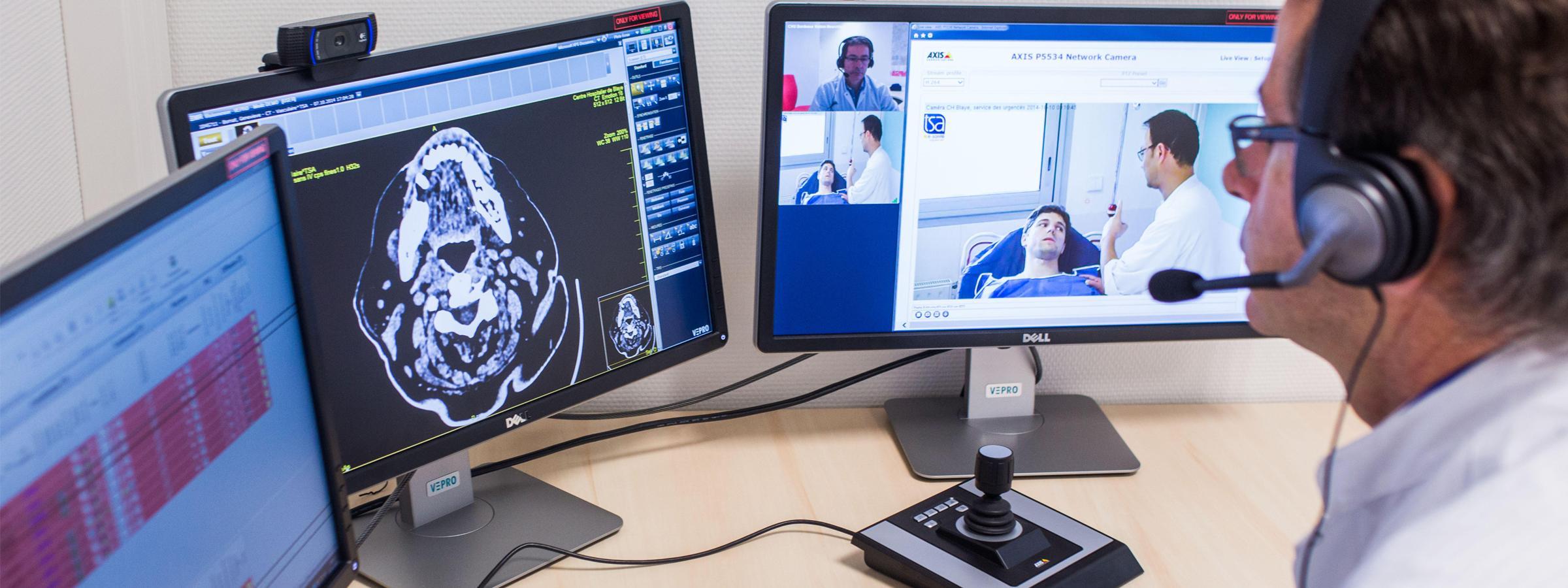
Every health system and physician group is now focused on strategies to make telemedicine more scalable across their networks. When we spoke recently with a chief medical information officer (CMIO) leading his system’s telemedicine strategy, he shared, “If there is one thing I wish executives would understand about telemedicine, it’s that it will never make doctors more efficient.”
His data show the average video visit takes just as long as an in-person encounter. True, there is no physical exam, but the virtual conversations can be lengthy. And adding in time lost to helping patients troubleshoot technology, some of his colleagues report that virtual visits may actually take a little longer.
He went on to explain that other kinds of virtual encounters, specifically asynchronous communication with a provider, sometimes supported by automated symptom triage engines like Zipnosis, are far more time-efficient ways to communicate with patients. Certain clinical situations may better lend themselves to these types of “e-visits”. Take dermatology, where sending a high-resolution picture of a rash to the clinician is more valuable than trying to view the problem live on a Zoom call.
Of course, video visits can be far more convenient for patients—and there is huge value in in providing access to patients wherever they are. But delivering telemedicine “at scale” to meet rising consumer expectations will require finding the right balance of asynchronous communication, telemedicine, and in-person visits to best fit specific clinical circumstances.
And we’ll need to rethink clinical workflow—centralizing some telemedicine delivery at the system level across individual practices.
Preparing for generations of Medicare growth
https://mailchi.mp/72a9d343926a/the-weekly-gist-september-24-2021?e=d1e747d2d8

The healthcare industry is now at the peak of the long-awaited transition of the Baby Boom generation into Medicare. The “greying” of the Boomers will continue to bring a rapid influx of new Medicare beneficiaries, but this is just the beginning of a protracted period of growth for the program, with the number of Medicare-eligible Americans increasing by more than 50 percent over the next three decades.
Using data from the US Census Bureau, the graphic above shows how the generational makeup of the Medicare population will change across time. The next decade will bring the fastest growth, as the latter half of the Baby Boom generation turns 65. Over that time, the Medicare-eligible population will increase by almost a third. Gen X will begin to age into Medicare in 2029. (Go ahead, take a minute. It hurts.) While fewer in number, Gen X beneficiaries, combined with the longer lifespan of Baby Boomers, will bring no respite from Medicare growth, with enrollment still increasing 11 percent between 2030 and 2040.
As the country looks at a prolonged period of Medicare cost growth, we’ll be counting on a ballooning workforce of Millennials and Gen Z youngsters—each part of generations even larger than the Baby Boom—to continue to fund the Medicare trust across the next 25 years, when the first Millennials will receive their Medicare cards. (See how it feels?)
Intermountain, SCL Health to create $11B system
https://mailchi.mp/72a9d343926a/the-weekly-gist-september-24-2021?e=d1e747d2d8
Salt Lake City-based Intermountain Healthcare announced plans to merge with Broomfield, CO-based SCL Health to form a 33-hospital, $11B dollar system working in six states. The combined system will keep the Intermountain name, be based in Salt Lake City, and be led by Intermountain CEO Dr. Marc Harrison.
Harrison said that the merger will accelerate the evolution toward population health and value, and “swiftly advance that cause across a broader geography”—a similar value proposition to the system’s previously proposed combination with South Dakota-based Sanford Health, which fell apart last December after Sanford’s CEO stepped down following his controversial comments about mask-wearing.
Intermountain has long been regarded as a national leader in clinical quality, and its integrated payer-provider approach is often cited as a model for US healthcare. The merger with SCL Health will enable expansion of its SelectHealth insurance plan and integrated care model into Colorado, Montana and Kansas, including the fast-growing Denver metropolitan area, making the combined system a formidable player across the Mountain West.
But as we’ve written before, achieving that vision will require a level of integration not often realized in similar mergers, and the burden of proof is on health systems to demonstrate that the merger will create meaningful value for patients and consumers.
We’ll be watching closely to better understand their plans for lowering costs and improving access and quality for patients across the region.


