
Cartoon – The Story is Thin



Delirium was linked to long-term cognitive decline in both surgical and nonsurgical patients, a meta-analysis showed.
Patients who experienced an episode of delirium were more than twice as likely to show long-term cognitive decline than patients without delirium (OR 2.30, 95% CI 1.85-2.86), reported Terry Goldberg, PhD, of Columbia University in New York City, and co-authors.
Delirium was associated with long-term cognitive decline with a Hedges g effect size of 0.45 (95% CI 0.34-0.57, P<0.001) in a meta-analysis of 23 observational studies (after one outlier study with an exceptionally high OR was excluded), they wrote in JAMA Neurology. Effect sizes were similar between surgical and nonsurgical groups.
“The connection between delirium and cognitive decline that we observed was highly significant and remarkably consistent,” Goldberg said.
“What we propose is that delirium is not simply a marker for those patients already on a downward trajectory, but may be causative in and of itself,” he told MedPage Today. “This may be especially relevant to COVID patients, many of whom experience delirium in the ICU.”
Delirium is “ubiquitous and spares no age groups or populations, occurring in 20% to 70% of hospitalized patients, with the higher numbers seen in critically ill patients on mechanical ventilation,” said Pratik Pandharipande, MD, co-director of the Critical Illness, Brain Dysfunction and Survivorship Center at Vanderbilt University in Nashville, who wasn’t involved with the meta-analysis.
“This study has great implications in the COVID era,” Pandharipande told MedPage Today. “Mechanically ventilated patients with COVID are at a much higher risk of developing delirium because they are subject to all the major risk factors — deeper levels of sedation, high severity of illness, often older age, and additionally, social isolation due to limited visitation rules in the hospital and the fact that the virus can directly affect the brain and lead to neuroinflammation.”
“The meta-analysis reported here shows a consistent message; all selected studies showed that delirium and longer duration of delirium were associated with cognitive impairment,” Pandharipande continued.
“While it is unclear if delirium causes dementia, there is mounting evidence — and the meta-analysis adds to this — that there are structural brain changes with delirium and this puts you at a worse cognitive trajectory,” he said.
“Incorporating strategies such as the ABCDEF bundle from the Society of Critical Care Medicine into the care of your patients — including mechanically ventilated COVID patients — is likely to reduce delirium and possibly its long-term consequences,” he added.
The meta-analysis included a systematic search of articles from 1965 through 2018. The researchers looked for studies that contrasted patients with and without delirium, had objective continuous or binary measures of cognitive outcome, and had a final time point of 3 months or later after the delirium episode.
Data from 24 observational studies, including 3,562 patients who experienced delirium and 6,987 controls who did not, were used. One study with an OR greater than 41 — an order of magnitude greater than any other study — was excluded from some analyses.
Mean study age was about 75 and mean follow-up after a delirium episode was 2.4 years. On average, men made up about 47% of the study populations. The Confusion Assessment Method (CAM) or CAM–intensive care unit was the most frequent delirium measure used, and the Mini-Mental State Examination was used most frequently as a cognitive outcome.
“In all studies, the group that experienced delirium had worse cognition at the final time point,” Goldberg and co-authors wrote.
Meta-regression did not show differences in cognitive outcomes between surgical and nonsurgical studies, suggesting “the underlying pathophysiological events associated with delirium may be similar and speculatively may be associated with inflammatory processes common to both contexts,” they added.
The researchers also did not find significant differences between cognition treated as a continuous variable based on neurocognitive test scores or as a binary variable based on the presence or absence of dementia.
The I2 measure of between-study variability in g was 0.81. Studies of longer duration yielded greater differences, while those with more covariates, and those without baseline cognitive matching, yielded smaller differences.
The observational studies used in this meta-analysis cannot show that delirium is a causative factor in subsequent cognitive decline, the researchers noted. Differences in cognitive outcome measures and the way dementia was diagnosed may be sources of variability, but meta-regressions did not find significant differences among them in terms of their effect on g, they added.
Importantly, the study could not evaluate delirium in the context of other factors, such as frailty, and unmeasured confounders may have influenced results.

Quest Diagnostics said its average turnaround time for a COVID-19 test is now at “seven or more days,” up from four to five days at the end of June.
Why it matters: Long backlogs make testing less useful — public health officials need to know what their local situation is like now, not what it was like a week ago. Delays are especially problematic if people who are infected continue to go about their lives while they wait for their results.
Between the lines: Quest told investors Monday that its second-quarter revenue will be down 6%, hovering around $1.83 billion, as coronavirus testing has supplanted other, more lucrative tests that had to be put off.

Roughly 5.4 million adults in the U.S. lost their health insurance from February to May after losing their jobs, according to a new estimate from Families USA, a group that favors the Affordable Care Act.
Why it matters: There are more adults under 65 without insurance in Southern states, which are the same states setting new records for single-day coronavirus infections along with rising hospitalizations, Axios’ Orion Rummler writes.
What they found: 3.9 million adults lost health insurance over one year during the Great Recession, per Families USA’s analysis. It only took four months in this current crisis for an estimated 5.4 million Americans to lose health insurance.
The backdrop: 21 million Americans were unemployed in May, according to the Bureau of Labor Statistics’ nonfarm payrolls report.
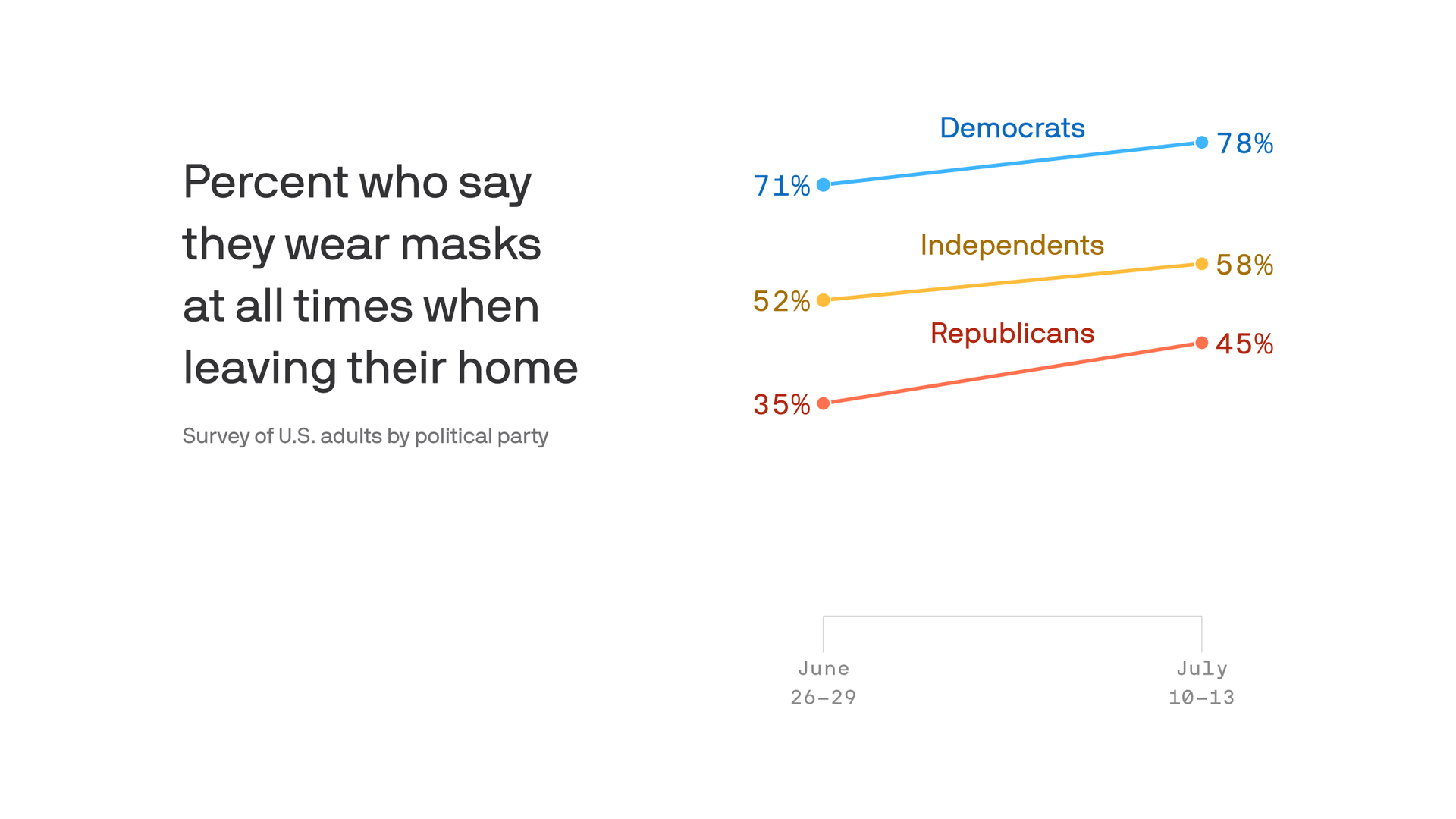
Nearly two-thirds of Americans — and a noticeably increasing number of Republicans — say they’re wearing a face mask whenever they leave the house, according to the Axios-Ipsos Coronavirus Index.
Why it matters: A weakening partisan divide over masks, and a broad-based increase in the number of people wearing them, would be a welcome development as most of the country tries to beat back a rapidly growing outbreak, Axios’ Sam Baker writes.
By the numbers: 62% of those surveyed said they’re wearing a mask “all the time” when they leave the house — up from 53% when we asked the same question two weeks ago.
Between the lines: These numbers may seem high — do two-thirds of the people you pass on the street have a mask on? But the fact that more people are claiming to wear them is at least a sign that masks are increasingly seen as important.
https://www.ipsos.com/en-us/news-polls/axios-ipsos-coronavirus-index
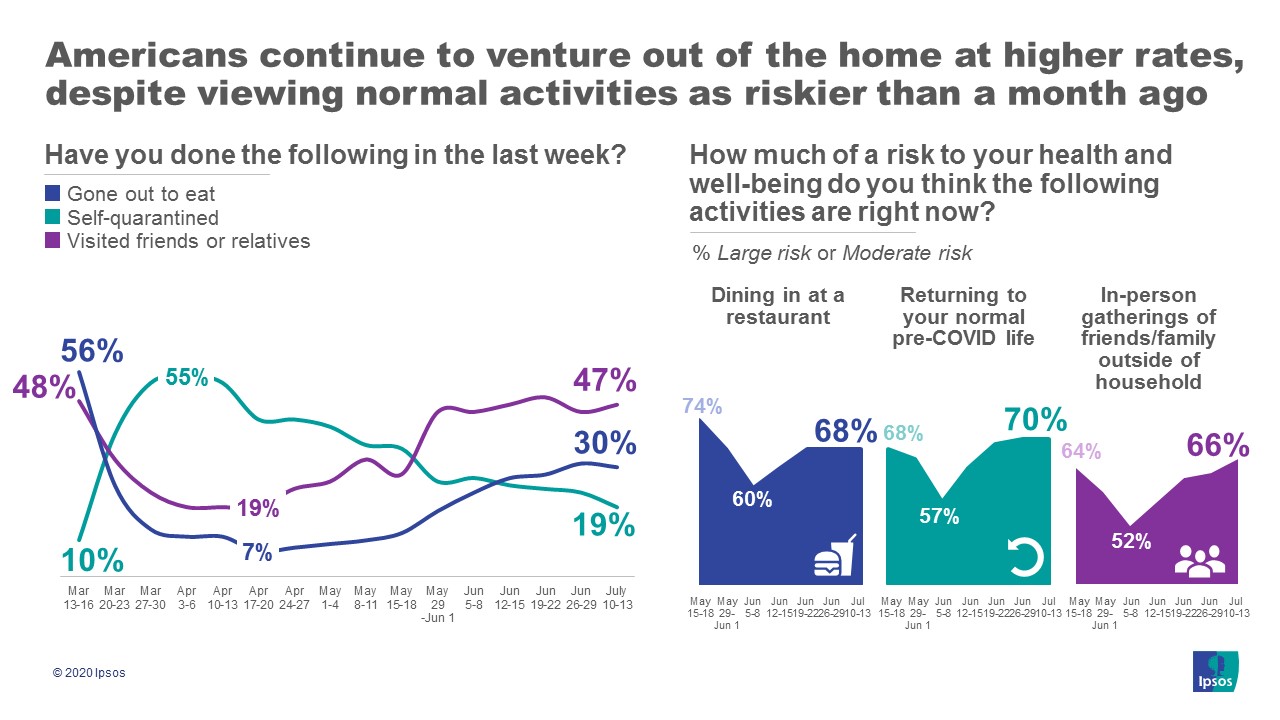
New Axios-Ipsos Coronavirus Index study finds that social distancing continues to decline except for mask use.
Fewer Americans report self-quarantining now than any point since the start of the pandemic according to our latest Axios-Ipsos Coronavirus Index. This corresponds with socializing and commercial activity remaining high, if not quite to pre-pandemic levels. However, more Americans see returning to a pre-coronavirus life as a large risk now than at any time since the high-point of the initial wave in mid-April.
Detailed findings:
1. Despite the surge in cases across the South and West, Americans continue to venture out of the home at higher rates and do not re-embrace major social distancing.
2. However, as cases surge, Americans are increasingly seeing normal activities as posing large risks.
3. Most Americans appear to be embracing mask use as a tool to cope with the coronavirus pandemic.
4. As the pandemic continues, public trust in both the federal government and state governments has fallen to a low in this tracking.
As June ends, the latest wave of the Axios-Ipsos Coronavirus Index finds that American fears of the coronavirus pandemic have resurged to levels last seen during the acute parts of the initial wave. This comes, however, as Americans continue to leave the home more frequently, albeit while taking protective measures.
Detailed Findings:
1. Levels of concerns have returned to levels last seen in early May as the pandemic spreads across the South and West.
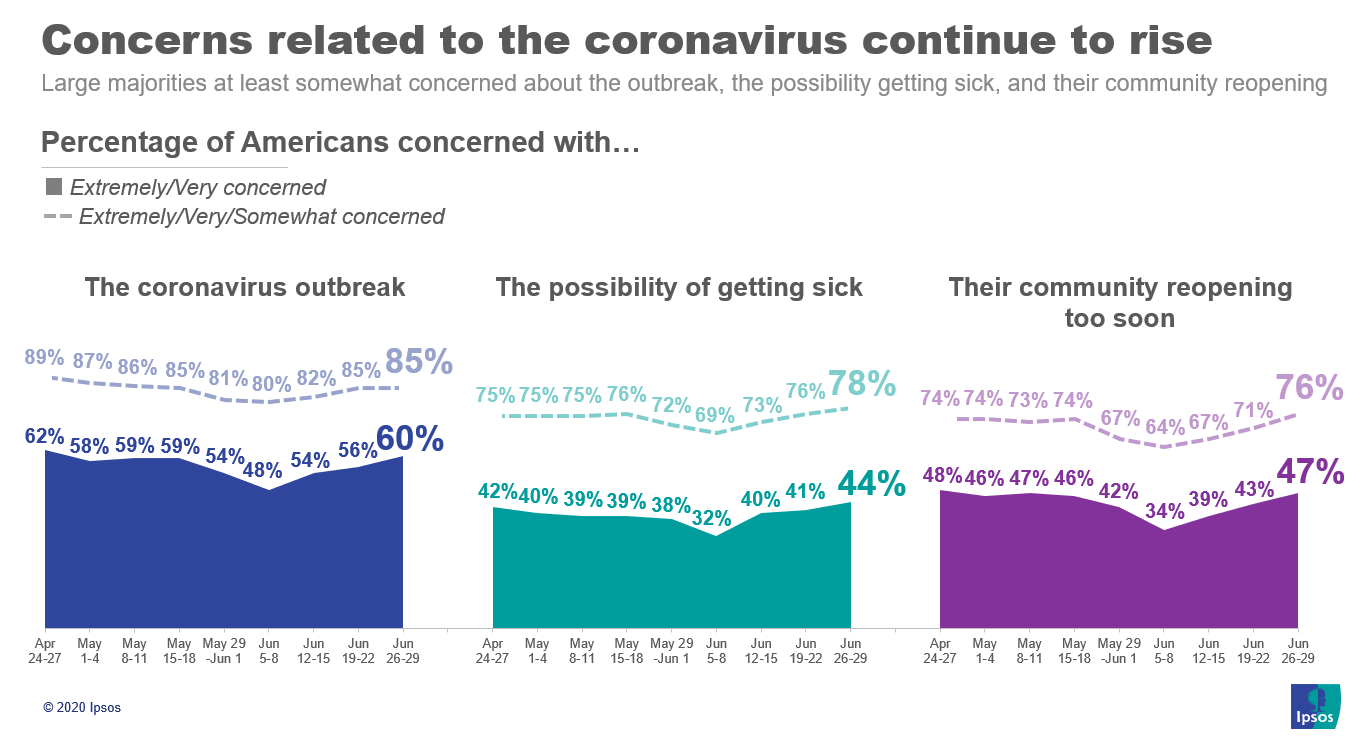
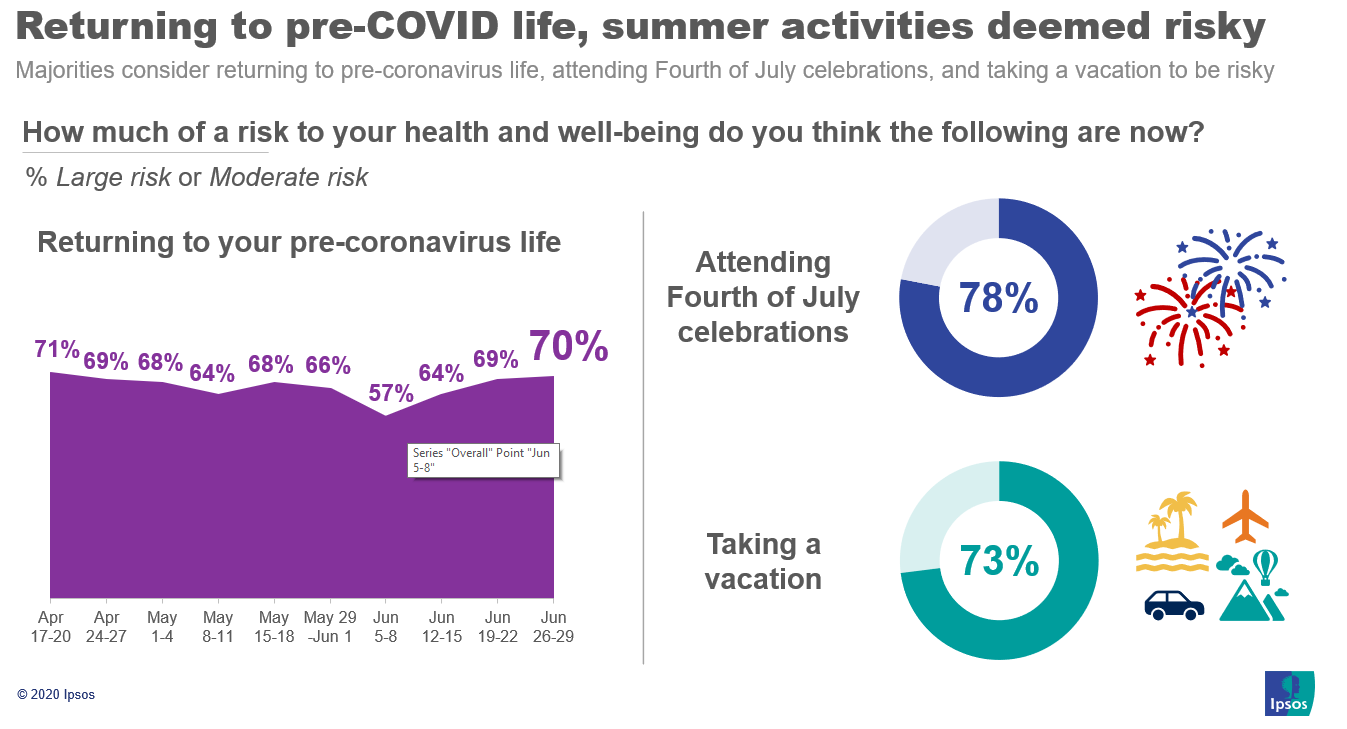
2. Correspondingly, perceptions of risk also continue to increase, particularly views of activities that may bring the respondent into contact with large groups of people.
3. Risk aversion may also put a damper on the upcoming Fourth of July holiday with 78% saying attending celebrations is a large or moderate risk.
4. Americans have started curtailing social engagement, however the number engaging in out of home commercial activities remains stable or continues to increase.
Our latest Axios-Ipsos Coronavirus Index finds that Americans are increasingly concerned about coronavirus and seeing ‘regular’ activities as increasingly risky after sentiment moderated earlier in June. This uptick in fears comes as Americans address a possible second wave and reflect on their potential to re-enter social distance quarantines if major warning thresholds are met.
Detailed Findings:
1. American concern with the coronavirus outbreak, while not as widespread as during early April, has increased notably over the past two weeks.
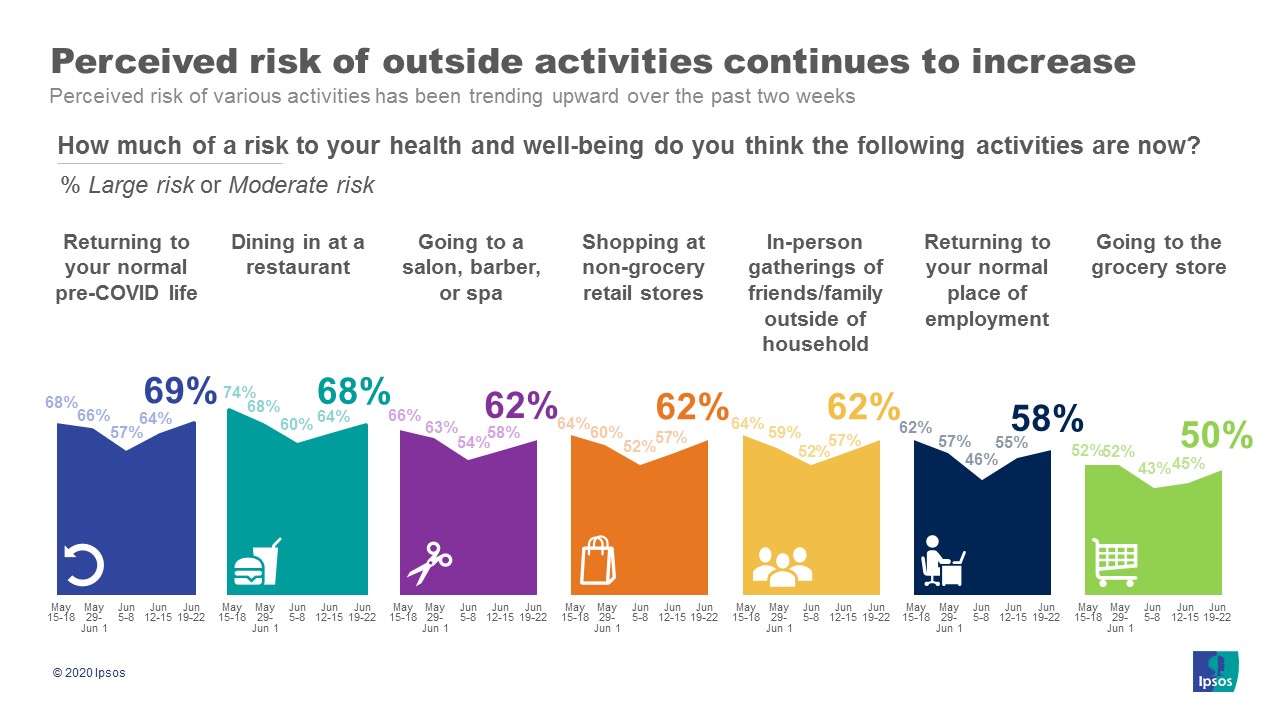
2. “Normal” activities are seen as increasingly risky by many including doing their job, going to the grocery store, or socializing with friends after multiple weeks of minimizing concerns.
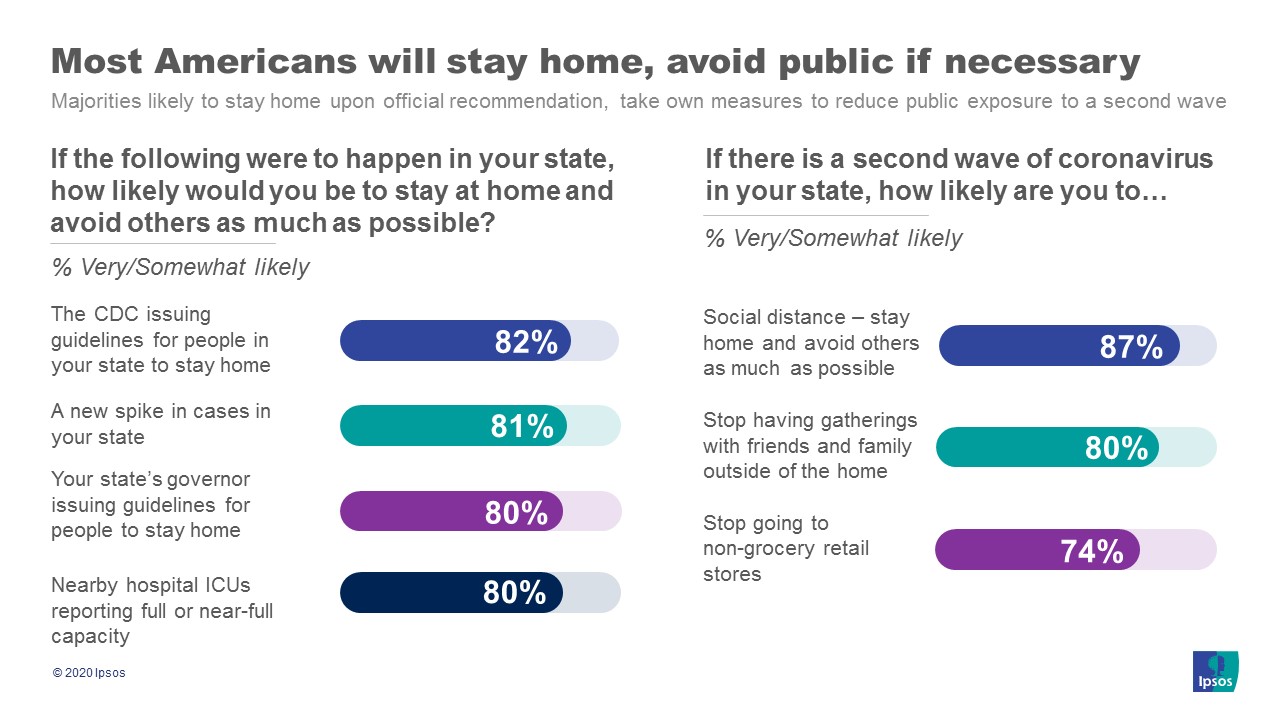
3. Americans continue to report that if a second wave hits their state, they will substantially withdraw to protect their health. They also express that they are watching for a wide range of signals of a second wave indicating it may not be official announcements that trigger a rebound in behavior.
4. Social distancing behaviors continue to subside, but geographical differences remain in people’s experiences.
5. One percent of the U.S. population has tested positive for coronavirus at this point.
At the end of our third month of tracking America’s response to the coronavirus pandemic, the Axios-Ipsos Coronavirus Index finds that even while Americans are increasingly engaging with each other outside the home, concerns about a second wave and perceived risks of regular activities mount.
Detailed Findings:
1. More Americans are very concerned about the overall COVID-19 outbreak than last week as a majority express high levels of concern about a second wave of the coronavirus.
2. If there is a second wave, large majorities of Americans report that they are likely to pull back into more socially distancing behaviors.
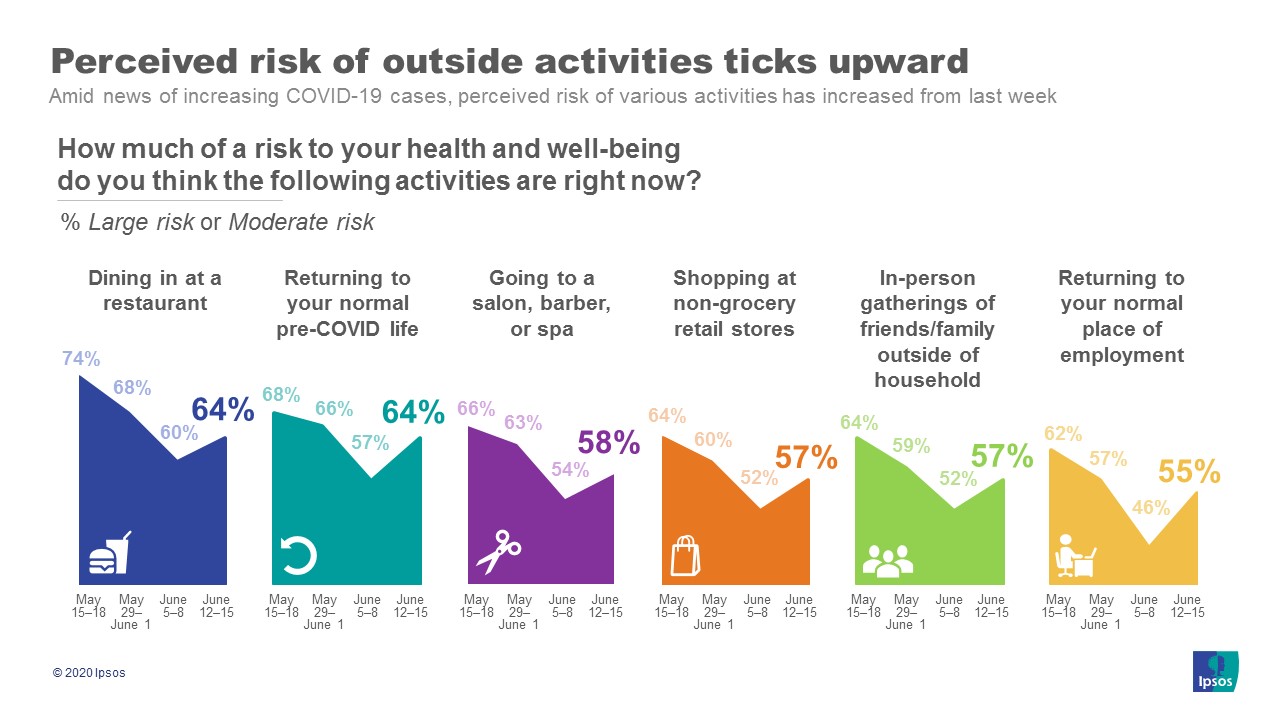
3. As discussion of a second wave mounts, Americans report seeing many ‘normal’ activities as being more risky than just a week ago.
4. Over a third of Americans know someone who has tested positive for coronavirus.

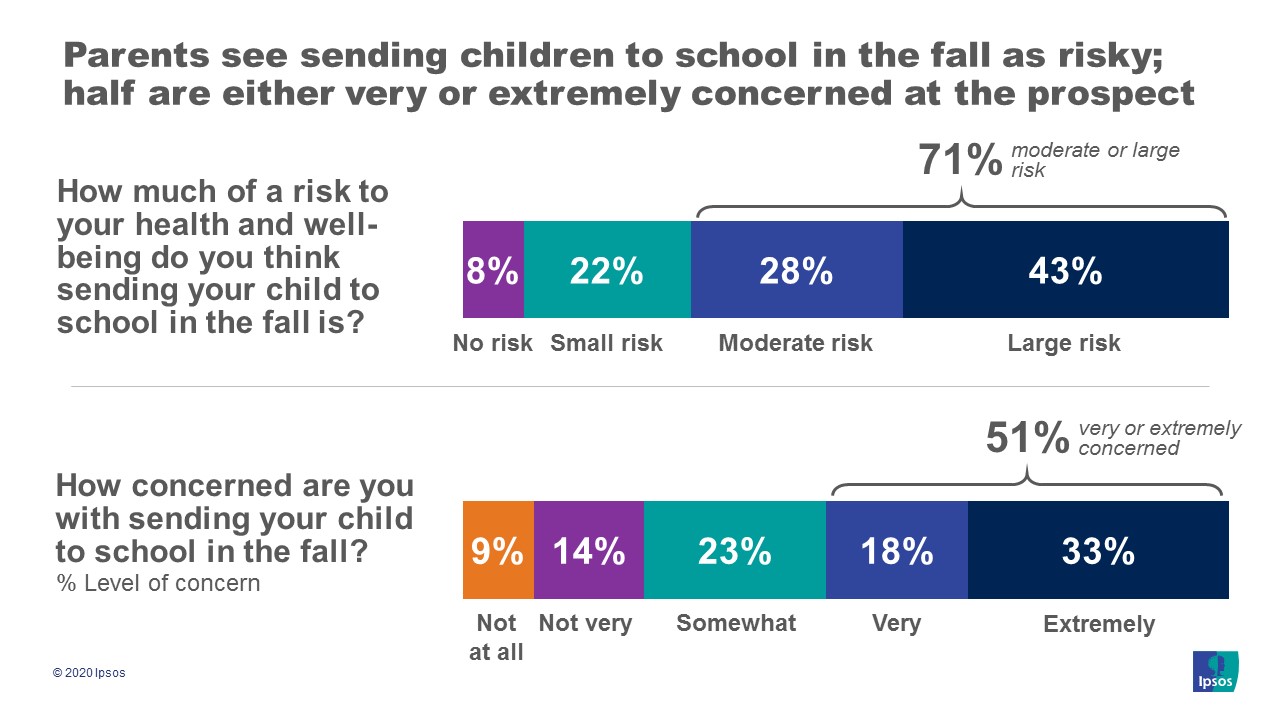
Most U.S. parents say it would be risky to send their children back to school in the fall — including a slim majority of Republicans and a staggering nine in 10 Black Americans — in this week’s installment of the Axios-Ipsos Coronavirus Index, Axios’ Margaret Talev reports.
Why it matters: President Trump and Education Secretary Betsy DeVos have threatened to withhold federal funds from schools that don’t reopen. The new findings suggest that this pressure campaign could backfire with many of the voters to whom Trump is trying to appeal ahead of the election.
What they’re saying: “Americans at this point, and parents more specifically, can’t be force-fed policies that go against what they think,” says Cliff Young, president of Ipsos U.S. Public Affairs.
Driving the news: Officials on Monday began announcing decisions impacting schools in some major metro areas, erring on the side of caution in response to health concerns and parents’ anxieties.

