
Cartoon – Sign of the Times (Back to School)



Riot fencing and razor wire reinforce the security zone on Capitol Hill in D.C.

The first month of the pandemic was also supposed to be the month I got pregnant, but my clinic closed and plans changed. Doctors and nurses needed personal protective equipment to tend to patients with covid-19, not women with recurrent miscarriages.
When the clinic reopened several months later, it turned out my husband and I had only been delaying yet another loss: In late August, he obeyed the medical center’s strict coronavirus protocols by waiting anxiously in the car while I trudged inside, masked and hand-sanitized, to receive a miscarriage diagnosis alone. I searched the ultrasound screen for the rhythmic beat of a heart, and then accepted that whatever had once been there was now gone.
But that was 2020 for you, consistent only in its utter crappiness. For every inspiring video of neighbors applauding a shift change at the hospital, another video of a bone-tired nurse begging viewers to believe covid was real, it wasn’t a hoax, wear a mask.
For every protest organized by activists who understood racism is also a long-term crisis, an appearance by the Proud Boys; for every GoFundMe successfully raising money for a beloved teacher’s hospital bills, a bitter acknowledgment that online panhandling is our country’s version of a safety net.
Millions of citizens stood in line for hours to vote for the next president and then endured weeks of legal petitions arguing that their votes should be negated. The basis for these legal actions were conspiracy theories too wild to be believed, except that millions of other citizens believed them.
And that was 2020 for you, too: accepting the increasingly obvious reality that the country was in peril, built on iffy foundations that now buckled under pressure. My loved ones who worked as waiters or bartenders or physical therapists were choosing between health and paychecks, and even from the lucky safety of my work-from-home job, each day began to feel like watching America itself arrive at a hospital in bad shape, praying that doctors or clergy could find something they were able to save.
Is there a heartbeat?
You want the answer to be yes, but even so, it was hard to imagine how we would come back from this.
What kind of delusional person would even try to get pregnant in this world? In my case it would never be a happy accident; it would always be a herculean effort. And so it seemed I should have some answers.
How do you explain to a future child: Sorry, we can’t fix climate change; we can’t even get people to agree that we should wear masks in grocery stores? How do you explain the frustration of seeing brokenness, and then the wearying choice of trying to fix it instead of abandoning it? How do you say, Love it anyway. You’re inheriting an absolute mess, but love it anyway?
I found myself asking a lot of things like this in 2020, but really they were all variations of the same question: What does it mean to have hope?
But in the middle of this, scientists worked quietly in labs all over the world. They applied the scientific method with extraordinary discipline and speed. A vaccine was developed. Tens of thousands of volunteers rolled up their sleeves and said, Try it out on me.
It was approved, and a nurse from Long Island was the first American televised receiving it. Her name was Sandra Lindsay, an immigrant from Jamaica who had come to the United States 30 years ago and who had spent the last year overseeing critical care teams in back-to-back shifts. She said she had agreed to go first to show communities of color, long abused, brushed-off or condescended to by the medical system, that the vaccine was safe.
Here was hope. And more than that, here was hope from a woman who had more reason than most to be embittered: an exhausted health-care worker who knew too well America’s hideous racial past and present, who nonetheless also knew there was only one way out of the tunnel. Here she was, rolling up her own sleeve, and there were the lines of hospital employees ready to go after her, and there were the truck drivers ferrying shipments of syringes.
I can’t have been the only person to watch the video of those early inoculations, feeling elated and tired, and to then burst into tears. I can’t have been the only person to realize that even as 2020 revealed brokenness, it also contained such astounding undercurrents of good.
The scientific method works whether you accept it or not. Doctors try to save you whether you respected public-health guidelines or not. Voter turnout was astronomical because individual citizens realized they were all, every one of them, necessary pieces in a puzzle, even if they couldn’t see what the final picture was supposed to look like.
The way to believe in America is to believe those things are passed down, too.
Sometime in October, a couple of months after my last miscarriage — when the country was riding up on eight months of lonely and stoic birthdays, graduations, deaths and weddings — I went into the bathroom and saw a faint second line on a First Response pregnancy test. It was far from my first rodeo, so I knew better than to get excited. I mentioned it to my husband with studied nonchalance, I told him that I’d test again in a few days but that we should assume the worst would happen.
Two weeks after that, I had a doctor’s appointment, and then another a week later, each time assuming the worst, but each time scheduling another appointment anyway, until eventually I was further along than I’d ever gotten before — by one day, then three days, then thirty.
I am not a superstitious person. I don’t believe that good things always come to those who deserve them. I believe that stories regularly have sad endings and that it’s often nobody’s fault when they do, and that we should tell more stories with sad endings so that people who experience them know that they’re not alone.
But 2020 has taught me that I am, for better or worse, someone who wants to hope for things. To believe in the people who developed vaccines. In the people who administered them. In Sandra Lindsay. In the people who delivered groceries, who sewed masks, who have long cursed America’s imperfect systems and long fought to change them, who still donate $10 to a sick teacher’s GoFundMe.
At my most recent appointment, the doctor’s office was backed up in a holiday logjam. I sat in the exam room for nearly three hours while my husband again waited anxiously in the car. I texted him sporadic updates and tried to put hope in a process that so far had not seemed to warrant my hope.
It all felt precarious. The current reality always feels precarious.
And yet there we all are together, searching for signs of life, hoping that whatever we emerge to can be better than what we had before, and that whatever we build will become our new legacy. The sonographer finally arrived and turned on the machine.
There was a heartbeat. There was a heartbeat.

| Dean Baquet, The Times’s executive editor, believes that 2020 will go down as a signature year in history, alongside years like 1968, 1945 and 1865. “It will long be remembered and studied as a time when more than 1.5 million people globally died during a pandemic, racial unrest gripped the world, and democracy itself faced extraordinary tests,” he writes. |
| Those words come from Dean’s introduction to The Times’s annual Year in Pictures feature. Here, my colleagues on The Morning and I have chosen a dozen of those pictures that we think best summarize 2020. But we obviously have room here for only a fraction of the year’s photographs — so I encourage you to check out the full selection. |
| As you do, ask yourself which pictures you would have selected if you had to pick only 12 to sum up 2020. |











Again, you can find the full Year in Pictures here.


• Since April, the numbers of new cases and deaths from the coronavirus have been falling nationally, although the number of cases ticked slightly upward in the first week of June, a few weeks after many states ended their stay-at-home orders.
• The spread of the virus has varied significantly from state to state. Some states, especially those with longer-lasting stay-at-home orders, have seen cases fall since April. Others, including many that ended their closures earlier, have seen increases.
• Scientists expect to see a rise in coronavirus cases in the coming weeks due to continued reopenings and the racial justice protests. However, it’s unclear how large those increases will be.
However, scientists say that there’s lots of uncertainty about whether, and how much, the coronavirus will spread following the lifting of stay-at-home orders and the emergence of protest marches for racial justice.
We looked at the most recent data and interviewed several researchers to explain what we’re seeing already, and what might happen in the future.
Nationally, both cases and deaths have generally been falling since April, although cases saw a small uptick in early June.
Here’s a chart showing the number of new coronavirus cases confirmed each day since the outbreak began in late February. The blue bars show the number of new cases per day, while the orange line shows the seven-day rolling average, which smooths out technical differences in the daily reporting.
“The social distancing that resulted from the closures slowed cases,” said Tara C. Smith, a professor of epidemiology at Kent State University.
Smith cited a recent study that estimated that the shutdowns prevented an additional 4.8 million confirmed coronavirus cases in the U.S., and about 60 million infections in all. (The 60 million figure includes people who didn’t know they were infected and did not confirm their infection with a test.) So far, there have been roughly 2 million confirmed coronavirus cases.
The decline in cases has been driven by significant improvements in the hardest-hit area: the tri-state region of New York, New Jersey and Connecticut. Each of those states has seen the number of new cases decline consistently since April, as can be seen in this chart:
The national numbers mask considerable differences among the states in new caseloads.
Beyond New York, New Jersey and Connecticut, several other large states have seen declining caseloads over time.
Here’s a chart showing the patterns for Pennsylvania, Illinois, Ohio, Michigan and Virginia, all of which have seen declines in new cases in recent weeks:
But other states have seen increases in recent weeks. Here’s a look at the upward trends in California, Texas, Florida, Georgia, North Carolina and Arizona:
One notable difference between the states with rising and falling numbers of new cases is the date they lifted their stay-at-home orders.
Almost every state in our chart that’s seeing rising numbers of new cases reopened between April 30 and May 22. (The one exception is California, which is a mystery to the experts we asked.)
By contrast, the states in our charts with falling numbers of new cases opened no earlier than May 28.
Experts said there are too many variables to conclude that reopening will inevitably produce rising new case counts. For instance, the virus’ spread may be proceeding differently in urban areas than in the rest of the state, something that the state-level data wouldn’t capture.
Also, the data we used are not adjusted for the number of tests being conducted. The more tests that are done, the more positive cases will be found, everything else being equal.
That said, if there is a connection between reopening and a rise in new cases, the states that delayed their openings may see their new case loads rise in the coming weeks.
“Until we have a vaccine for prevention, our ‘people’ interventions are what stand between us and the virus spreading,” said Nicole Gatto, an associate professor in the School of Community and Global Health at Claremont Graduate University. “Reopening efforts and mixing of people again will reintroduce the potential for viral transmission.”
For now, the impact of the protests on new caseloads is not showing up in the data. Any impact would become evident only in the next few weeks, as participants get tested and the results are tabulated.
Some aspects of the protests could promote the spread, experts said.
“The protests have ingredients which we have been making efforts to avoid these last three months: large gatherings of people in close proximity to each other not always wearing protective face coverings,” Gatto said. “Add in tear gas, and the recipe becomes worse.”
People who were arrested at protests and had to spend time in jail could also be at higher risk for infection, scientists said.
The best-case scenario, scientists said, is that the marches’ outdoor locations and the precautions taken by participants will cut down on the spread.
“Outdoor gatherings may present less transmission risk, especially when everyone is wearing a mask,” said Forrest W. Crawford, a biostatistician at Yale University.
While emphasizing the uncertainties, Smith said she was surprised by the relatively modest impact of the state reopenings on the virus’ spread so far. So there may be reason for cautious optimism.
“I’m expecting cases to grow over the next two weeks, but it’s really tough to say if it will be a spike or a less dramatic increase,” she said.
https://www.insider.com/expert-us-is-in-an-unsure-moment-with-coronavirus-2020-6
Dr. Michael Osterholm, the director of the Center for Infectious Disease Research and Prevention, said Sunday that the US is in an “unsure moment” as states reopen and new cases emerge.
“We have to be humble and say we’re in an unsure moment,” Osterholm said on “Fox News Sunday,” adding that states across the country are in varied stages of the pandemic as 22 have recorded an increase in coronavirus cases, eight in plateaus, and 21 with decreasing cases.
Osterholm was speaking as states have been reopening businesses for weeks, Americans flocked to warm weather, and widespread protests drew people to the streets in cities across the country. The first few weeks of June have seen sharp rises in new cases and hospitalizations.
The US hit a grim milestone two weeks into June as it marked more than 2 million infected and 115,000 dead from the virus. Centers for Disease Control and Prevention predicted on June 12 that the US coronavirus death toll could increase to 130,000 by July 4.
“About 5% of the US population has been infected to date with the virus, this virus is not going to rest until it gets to about 60% or 70%,” Osterholm said. “When I say rest, I mean just slow down, so one way or another we’re going to see a lot of additional cases.”
The expert told host Chris Wallace that the increase cannot only be attributed to increasingly available testing, and it’s too early to tell if protests have been a source of widespread infections, but early data suggests not.
“These next weeks, the two weeks are going to be the telling time, we just don’t know,” he said. “We’re not driving this tiger, we’re riding it.”
“My biggest concern is if cases start to disappear across the country, suggesting we are in a trough” that would lead to a second wave of the virus, Osterholm said.
Dr. Anthony Fauci has recently downplayed concerns that the recent rise in cases of the novel coronavirus in the US doesn’t a “second spike” of infections, and a seasonal resurgence was “not inevitable.”
Though Fauci told CNN on June 12 that indicators like hospitalizations could still spell concern for officials, increased testing and CDC capabilities could counter a possible resurgence in cases.

AMY GOODMAN: I certainly look forward to the day you’re sitting here in the studio right next to me, but right now the numbers are grim. The number of confirmed U.S. coronavirus cases has officially topped 2 million in the United States, the highest number in the world by far, but public health officials say the true number of infections is certain to be many times greater. Officially, the U.S. death toll is nearing 113,000, but that number is expected to be way higher, as well.
This comes as President Trump has announced plans to hold campaign rallies in several states that are battling new surges of infections, including Florida, Texas, North Carolina and Arizona — which saw cases rise from nearly 200 a day last month to more than 1,400 a day this week.
On Tuesday, the country’s top infectious disease expert, Dr. Anthony Fauci, called the coronavirus his worst nightmare.
DR. ANTHONY FAUCI: Now we have something that indeed turned out to be my worst nightmare: something that’s highly transmissible, and in a period — if you just think about it — in a period of four months, it has devastated the world. … And it isn’t over yet.
AMY GOODMAN: This comes as Vice President Mike Pence tweeted — then deleted — a photo of himself on Wednesday greeting scores of Trump 2020 campaign staffers, all of whom were packed tightly together, indoors, wearing no masks, in contravention of CDC guidelines to stop the spread of the coronavirus.
Well, for more, we’re going directly to Dr. Craig Spencer, director of global health in emergency medicine at Columbia University Medical Center. His recent piece in The Washington Post is headlined “The strange new quiet in New York emergency rooms.”
Dr. Spencer, welcome back to Democracy Now! It’s great to have you with this, though this day is a very painful one. Cases in the United States have just topped 2 million, though that number is expected to be far higher, with the number of deaths at well over 113,000, we believe, Harvard University predicting that that number could almost double by the end of September. Dr. Craig Spencer, your thoughts on the reopening of this country and what these numbers mean?
DR. CRAIG SPENCER: That’s a really good question. So, when you think about those numbers, remember that very early on, in March, in April, when I was seeing this huge surge in New York City emergency departments, we weren’t testing. We were testing people that were only being admitted to the hospital, so we were knowingly sending home, all across the epicenter, people that were undoubtedly infected with coronavirus, that are not included in that case total. So you’re right: The likely number is much, much higher, maybe 5, 10 times higher than that.
In addition, we know that that’s true for the death count, as well. This has become this political flashpoint, talking about how many people have died. We know that it’s an incredible and incalculable toll, over 100,000. Within the next few days, we’ll have more people that have died from COVID than died during World War I here in the United States. So that’s absolutely incredible.
We know that, also, just because New York City was bad, other places across the country might not get as bad, but that doesn’t mean that they’re not bad. So, we had this huge surge, of a bunch of deaths in New York City, you know, over 200,000 cases, tens of thousands of deaths. What we’re seeing now is we’re seeing this virus continue to roll across this country, causing these localized outbreaks.
And this is, I think, going to be our reality, until we take this serious, until we actually take the actions necessary to stop this virus from spreading. Opening up, like we’ve seen in Arizona and many other places, is exactly counter to what we need to be doing to keep this virus under control. So, yeah, I worry that what we’ve seen so far is an undercount and what we’re seeing now is really just the beginning of another wave of infections spreading across the country.
NERMEEN SHAIKH: Well, Dr. Spencer, I want to ask — it’s not just in the U.S. that cases have hit this dreadful milestone. Worldwide, cases have now topped 7 million, although, like the U.S., the number is likely to be much higher because of inadequate testing all over the world. But I’d like to focus on the racial dimension of the impact of coronavirus, not just in the U.S., but also worldwide. Just as one example, in Brazil — and this is a really stunning statistic — that in Rio’s favelas, more people have died than in 15 states in Brazil combined. So, could you talk about this, both in the context of the U.S., and explain whether that is still the case, and what you expect in terms of this racial differential, how it will play out as this virus spreads?
DR. CRAIG SPENCER: Absolutely. What we’re seeing, not just in the United States, but all over the world, is coronavirus is amplifying these racial and ethnic inequities. It is impacting disproportionately vulnerable and already marginalized populations.
Starting here in the U.S., if you think about the fact, in New York City, the likelihood of dying from coronavirus was double if you’re Black or African American or Latino or Hispanic, double than what it was for white or Asian New Yorkers, so we already know that this disproportionate impact on already marginalized and vulnerable communities exists here in the United States, in the financial capital of the world. It’s the same throughout the U.S. A lot of the data that we’re seeing over the past few days, as we’re getting this disaggregated data by race and ethnic background, is that it is hitting these communities much harder than it is hitting white and other communities in the United States.
The statistics that you give for Brazil are being played out all over the world. We know that communities that already lack access to good healthcare or don’t have the same economic ability to stay home and participate in social distancing are being disproportionately impacted.
That is why we need to focus on and think about, in our public health messaging and in our public health efforts, to think about those communities that are already on the margins, that are already vulnerable, that are already suffering from chronic health conditions that may make them more likely to get infected with and die from this disease. We need to think about that as part of our response, not just in New York, not just in the U.S., but in Brazil, in Peru, in Ecuador, in South Africa, in many other countries, where we’re seeing the disproportionate number of cases coming from now.
We’re seeing — you know, I think it was just pointed out that three-quarters of all the new cases, the record-high cases, over 136,000 this past weekend on one day, three-quarters of those are coming from just 10 countries. And we know that that will continue, and it will burn through those countries and will continue through many more.
As of right now, we haven’t seen huge numbers in places like West Africa and East Africa, sub-Saharan Africa, where many people were concerned about initially. Part of that is because they have in place a lot of the tools from previous outbreaks, especially in West Africa around Ebola. But it may be that we need more testing. It may be that we’re still waiting to see the big increase in cases that may eventually hit there, as well.
NERMEEN SHAIKH: Dr. Spencer, you mentioned that on Sunday — it was Sunday where there were 136,000 new infections, which was a first. It was the highest number since the virus began. But even as the virus is spreading, much like states opening in the U.S., countries are also starting to reopen around the world, including countries that have now among the highest outbreaks. Brazil is now second only to the U.S. in the number of infections, and Russia is third, and these countries are opening, along with India and so on. So, could you — I mean, there are various reasons that countries are opening. A lot of them are not able — large numbers of people are not able to survive as long as the country is closed, like, in fact, Brazil and India. So what are the steps that countries can take to reopen safely? What is necessary to arrest the spread of the virus and allow people at the same time to be out?
DR. CRAIG SPENCER: It’s tough, because we know that this virus cannot infect you if this virus does not find you. If there’s going to be people in close proximity, whether it’s in India or Illinois, this virus will pass and will infect you. I have a lot of concern, much as you pointed out, places like India, 1.3 billion people, where they’re starting to open up after a longer period of being locked down, and case numbers are steadily increasing.
You’re right that a lot of people around the world don’t have access to multitrillion-dollar stimulus plans like we do in the United States, the ability to provide at least some sustenance during this time that people are being forced at home. Many people, if they don’t go outside, don’t eat. If they don’t work, you know, their families can’t pay rent or really just can’t live.
What do we do? We rely on the exact same tools that we should be relying on here, which is good public health principles. You need to be able to locate those people who are sick, isolate them, remove them from the community, and try to do contact tracing to see who they potentially have exposed. Otherwise, we’re going to continue to have people circulating with this virus that can continue to infect other people.
It’s much harder in places where people may not have access to a phone or may not have an address or may not have the same infrastructure that we have here in the United States. But it’s absolutely possible. We’ve done this with smallpox eradication decades ago. We need to be doing this good, simple, bread-and-butter, basic public health work all around the world. But that takes a lot of commitment, it takes a lot of money, and it takes a lot of time.
AMY GOODMAN: It looks like President Trump is reading the rules and just doing the opposite — I mean, everything from pulling out of the World Health Organization, which — and if you could talk about the significance of this? You’re a world health expert. You yourself survived Ebola after working in Africa around that disease. And also here at home, I mean, pulling out of Charlotte, the Republican convention, because the governor wouldn’t agree to no social distancing, and he didn’t want those that came to the convention to wear masks. If you can talk about the significance, what might seem trite to some people, but what exactly masks do? And also, in this country, the states we see that have relaxed so much — he might move, announce tomorrow, the convention to Florida. There’s surges there. There’s surges in Arizona, extremely desperate question of whether a lockdown will be reimposed there. What has to happen? What exactly, when we say testing, should be available? And do you have enough masks even where you work?
DR. CRAIG SPENCER: Great. Yes. So, let me answer each of those. I think, first, on the World Health Organization, and really the rhetoric that is coming from the White House, it needs to be one of global solidarity right now. We are not going to beat this alone. I think that that’s been proven. This idea of American exceptionalism now is only true in that we have the most cases of anywhere in the world. We are not going to beat this alone. No country is going to beat this alone. As Dr. Fauci said, this is his worst nightmare. It’s my worst nightmare, as well. This is a virus that was first discovered just months ago, and has now really taken over the world. We need organizations like the World Health Organization, even if it isn’t perfect. And I’ve had qualms with it in the past. I’ve written about it, I’ve spoken about it, about the response as part of the West Africa Ebola outbreak that I witnessed firsthand. But at the end of the day, they do really, really good work, and they do the work that other organizations, including the United States, are not doing around the world, and that protects us. So, we absolutely, despite their imperfections, need to further invest and support them.
In terms of masks, masks may be, in addition to social distancing, one of the few things that really, really helps us and has proven to decrease transmission. We know that if a significant proportion of society — you know, 60, 70, 80% of people — are wearing masks, that will significantly decrease the amount of transmission and can prevent this virus from spreading very rapidly. Everyone should be wearing masks. I think, in the United States right now, we should consider the whole country as a hot zone. And the risk of transmission being very high, regardless of whether you’re in New York or North Dakota, people should be wearing a mask when they’re going outside and when they’re interacting with others that they generally don’t interact with.
We know the science is good. I will say that from a public health perspective, there was some initial reluctance and, really, I guess, some confusion early on about whether people should be using masks. We didn’t have a lot of the science to know whether it would help. We do now. And thankfully, we’re changing our recommendations.
We also were concerned about the availability of masks early on. As you mentioned, there was questions around availability of personal protective equipment, whether we had enough in hospitals to provide care while keeping providers safe. It’s better now, but there are still a lot of people who are saying that they’re reusing masks, that we still need more personal protective equipment. So, for the moment, everyone should be wearing a mask.
AMY GOODMAN: And for the protests outside?
DR. CRAIG SPENCER: Absolutely. Yeah, of course. Just because I think we have personal passions around public health crises, that doesn’t prevent us from being infected. From a public health perspective, of course I have concerns that people who are close and are yelling and are being tear-gassed and are not wearing masks, if that’s all the case, it’s certainly an environment where the coronavirus could spread.
So, what I’ve been telling everyone that’s protesting is exercise your right to protest — I think that’s great — but be safe. We are in a pandemic. We’re in a public health emergency. Wear a mask. Socially distance as much as you possibly can. Wash your hands.
AMY GOODMAN: And are you telling the authorities to stop tear-gassing and pepper-spraying the protesters?
DR. CRAIG SPENCER: I mean, well, one, it’s illegal. You should definitely stop tear-gassing. We know that what happens when people get tear-gassed is they cough, and it increases the secretions, which increases the risk. It increases the transmissibility of this virus.
In addition to that, you know, holding people and arresting them and putting them into small cells with others without masks is also, as we’ve seen from this huge number of cases in places like meatpacking plants or in jails, in prisons, the number of cases have been extremely high in those places. Putting people into holding cells for a prolonged period of time is not going to help; it’s definitely going to increase the transmissibility of this virus.
So, yes, everyone should be wearing a mask. I think everyone should have a mask on when you’re anywhere that your interacting with others can potentially spread this.
I think your other question was around testing. We know that right now testing has significantly increased in the U.S. Is it adequate? No, I don’t think so. I know I hear from a lot of people who say they still have to drive two to three hours to get a test. We still have questions around the reliability of some of serology tests, or the antibody tests. Those are the tests that will tell you whether or not you’ve been previously exposed and now have antibodies to the disease. Some of the more readily available tests just aren’t that great. And so, we can’t use them yet to make really widespread decisions on who might have antibodies, who might have protection and who can maybe more safely go back into society without the fear of being infected.
NERMEEN SHAIKH: Dr. Spencer, we just have 30 seconds. Very quickly, there are 135 vaccines in development. What’s your prognosis? When will there be a vaccine or a drug treatment?
DR. CRAIG SPENCER: We have one drug that shortens the time that people are sick. We don’t know about the impact on mortality. There are other treatments that are in process now. Hopefully some of them work.
In terms of vaccines, we will have a vaccine, very likely, that we know is effective, probably at some time later this year. The bigger process is going to be how do we scale it up to make hundreds of millions of doses; how do we do it in a way that we can get it to all of the people that deserve it, not just the people that can pay for it. I think these are going to be some of the bigger questions and bigger problems that we’re going to face, going forward. But I’m optimistic that we’ll have a vaccine or many vaccines, hopefully, in the next year.
AMY GOODMAN: Dr. Craig Spencer, we want to thank you so much for being with us, director of global health in emergency medicine at Columbia University Medical Center. And thank you so much for your work as an essential worker. Dr. Spencer’s recent piece, we’ll link to at democracynow.org. It’s in The Washington Post, headlined “The strange new quiet in New York emergency rooms.”
When we come back, George Floyd’s brother testifies before Congress, a day after he laid his brother to rest. Stay with us.
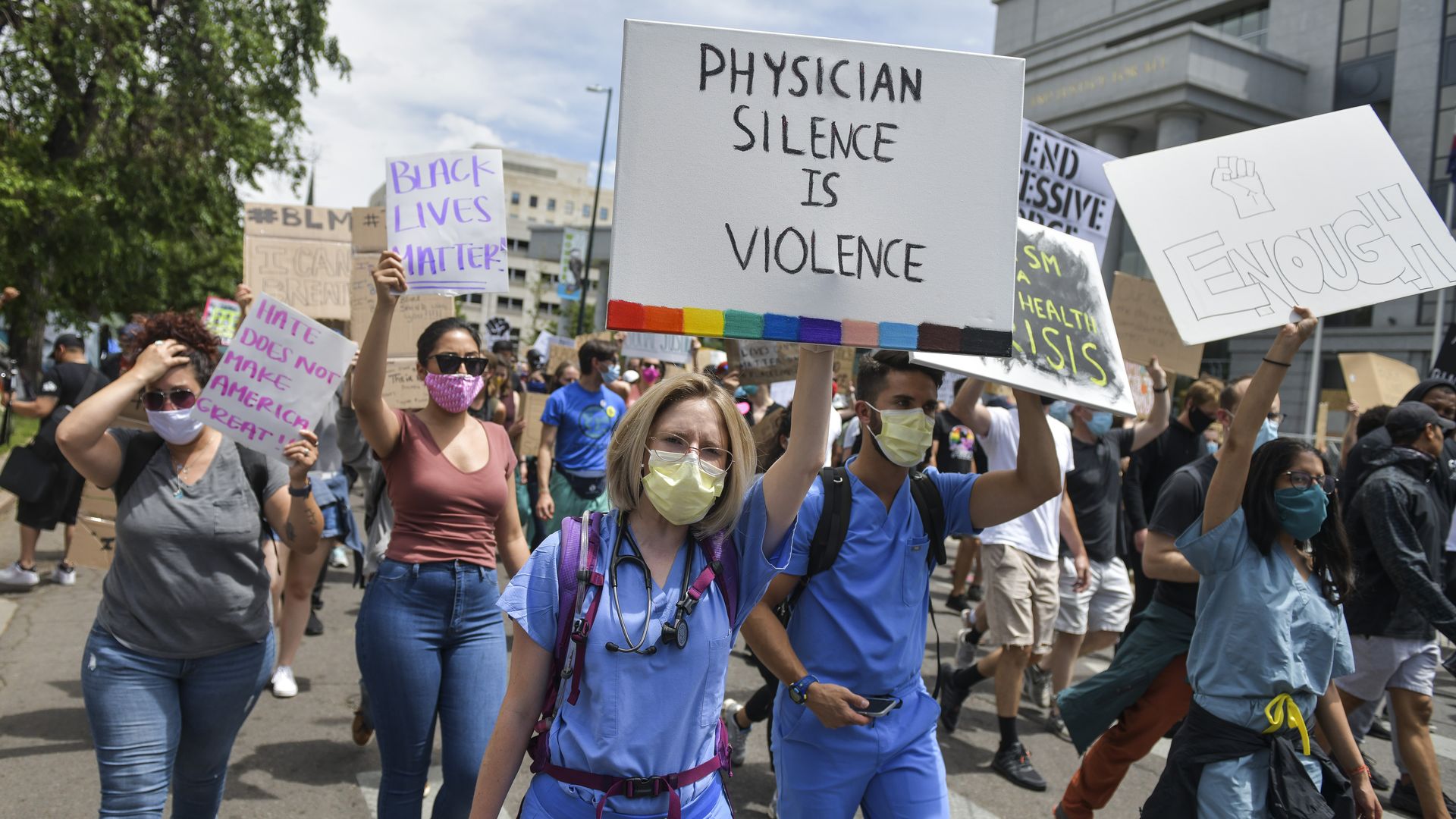
When protests broke out against the coronavirus lockdown, many public health experts were quick to warn about spreading the virus. When protests broke out after George Floyd’s death, some of the same experts embraced the protests. That’s led to charges of double standards among scientists.
Why it matters: Scientists who are seen as changing recommendations based on political and social priorities, however important, risk losing public trust. That could cause people to disregard their advice should the pandemic require stricter lockdown policies.
What’s happening: Many public health experts came out against public gatherings of almost any sort this spring — including protests over lockdown policies and large religious gatherings.
Yes, but: Spending time in a large group, even outdoors and wearing masks — as many of the protesters are — does raise the risk of coronavirus transmission, says Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota.
The difference in tone between how some public health experts are viewing the current protests and earlier ones focused on the lockdowns themselves was seized upon by a number of critics, as well as the Trump campaign.
The current debate underscores a larger question: What role should scientists play in policymaking?
The big picture: The debate risks exacerbating a partisan divide among Americans in their reported trust in scientists.
What to watch: If there is a rise in new cases in the coming weeks, there will be pressure to trace them — to protests, rallies and the reopening of states. How experts weigh in could affect how their recommendations will be viewed in the future — and whether the public, whatever their political leanings, will follow them again.