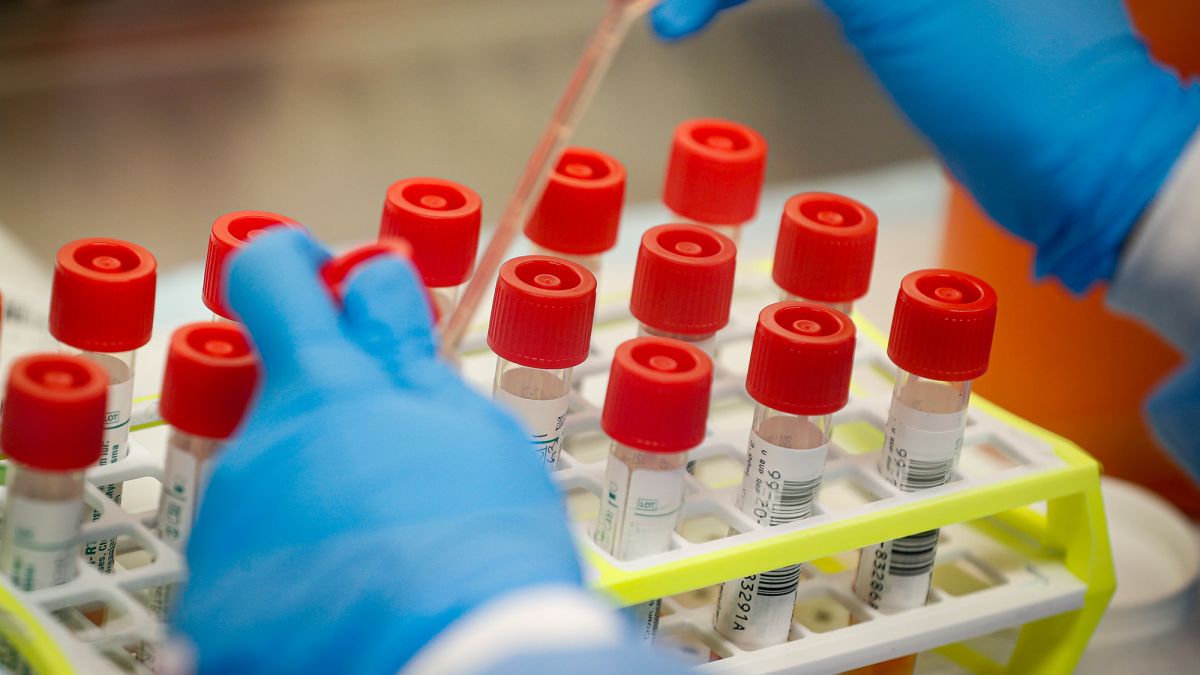
Nations fighting in World War I were reluctant to report their flu outbreaks.
“Spanish flu” has been used to describe the flu pandemic of 1918 and 1919 and the name suggests the outbreak started in Spain. But the term is actually a misnomer and points to a key fact: nations involved in World War I didn’t accurately report their flu outbreaks.
Spain remained neutral throughout World War I and its press freely reported its flu cases, including when the Spanish king Alfonso XIII contracted it in the spring of 1918. This led to the misperception that the flu had originated or was at its worst in Spain.
“Basically, it gets called the ‘Spanish flu’ because the Spanish media did their job,” says Lora Vogt, curator of education at the National WWI Museum and Memorial in Kansas City, Missouri. In Great Britain and the United States—which has a long history of blaming other countries for disease—the outbreak was also known as the “Spanish grip” or “Spanish Lady.”
Historians aren’t actually sure where the 1918 flu strain began, but the first recorded cases were at a U.S. Army camp in Kansas in March 1918. By the end of 1919, it had infected up to a third of the world’s population and killed some 50 million people. It was the worst flu pandemic in recorded history, and it was likely exacerbated by a combination of censorship, skepticism and denial among warring nations.
“The viruses don’t care where they come from, they just love taking advantage of wartime censorship,” says Carol R. Byerly, author of Fever of War: The Influenza Epidemic in the U.S. Army during World War I. “Censorship is very dangerous during a pandemic.”
The Flu in Europe

Patients lie in an influenza ward at the U.S. Army Camp Hospital No. 45 in Aix-les-Baines, France, during World War I.
Corbis/Getty Images
When the flu broke out in 1918, wartime press censorship was more entrenched in European countries because Europe had been fighting since 1914, while the United States had only entered the war in 1917. It’s hard to know the scope of this censorship, since the most effective way to cover something up is to not leave publicly-accessible records of its suppression. Discovering the impact of censorship is also complicated by the fact that when governments pass censorship laws, people often censor themselves out of fear of breaking the law.
In Great Britain, which fought for the Allied Powers, “the Defense of the Realm Act was used to a certain extent to suppress…news stories that might be a threat to national morale,” says Catharine Arnold, author of Pandemic 1918: Eyewitness Accounts from the Greatest Medical Holocaust in Modern History. “The government can slam what’s called a D-Notice on [a news story]—‘D’ for Defense—and it means it can’t be published because it’s not in the national interest.”
Both newspapers and public officials claimed during the flu’s first wave in the spring and early summer of 1918 that it wasn’t a serious threat. The Illustrated London News wrote that the 1918 flu was “so mild as to show that the original virus is becoming attenuated by frequent transmission.” Sir Arthur Newsholme, chief medical officer of the British Local Government Board, suggested it was unpatriotic to be concerned with the flu rather than the war, Arnold says.
The flu’s second wave, which began in late summer and worsened that fall, was far deadlier. Even so, warring nations continued to try to hide it. In August, the interior minister of Italy—another Allied Power—denied reports of the flu’s spread. In September, British officials and newspaper barons suppressed news that the prime minister had caught the flu while on a morale-boosting trip to Manchester. Instead, the Manchester Guardian explained his extended stay in the city by claiming he’d caught a “severe chill” in a rainstorm.
Warring nations covered up the flu to protect morale among their own citizens and soldiers, but also because they didn’t want enemy nations to know they were suffering an outbreak. The flu devastated General Erich Ludendorff’s German troops so badly that he had to put off his last offensive. The general, whose empire fought for the Central Powers, was anxious to hide his troops’ flu outbreaks from the opposing Allied Powers.
“Ludendorff is famous for observing [flu outbreaks among soldiers] and saying, oh my god this is the end of the war,” Byerly says. “His soldiers are getting influenza and he doesn’t want anybody to know, because then the French could attack him.”
The Pandemic in the United States

Patients at U. S. Army Hospital No. 30 at a movie wear masks because of an influenza epidemic.
The National Library of Medicine
The United States entered WWI as an Allied Power in April 1917. A little over a year later, it passed the 1918 Sedition Act, which made it a crime to say anything the government perceived as harming the country or the war effort. Again, it’s difficult to know the extent to which the government may have used this to silence reports of the flu, or the extent to which newspapers self-censored for fear of retribution. Whatever the motivation, some U.S. newspapers downplayed the risk of the flu or the extent of its spread.
In anticipation of Philadelphia’s “Liberty Loan March” in September, doctors tried to use the press to warn citizens that it was unsafe. Yet city newspaper editors refused to run articles or print doctors’ letters about their concerns. In addition to trying to warn the public through the press, doctors had also unsuccessfully tried to convince Philadelphia’s public health director to cancel the march.
The war bonds fundraiser drew several thousand people, creating the perfect place for the virus to spread. Over the next four weeks, the flu killed 12,191 people in Philadelphia.
Similarly, many U.S. military and government officials downplayed the flu or declined to implement health measures that would help slow its spread. Byerly says the Army’s medical department recognized the threat the flu posed to the troops and urged officials to stop troop transports, halt the draft and quarantine soldiers; but they faced resistance from the line command, the War Department and President Woodrow Wilson.
Wilson’s administration eventually responded to their pleas by suspending one draft and reducing the occupancy on troop ships by 15 percent, but other than that it didn’t take the extensive measures medical workers recommended. General Peyton March successfully convinced Wilson that the U.S. should not stop the transports, and as a result, soldiers continued to get sick. By the end of the year, about 45,000 U.S. Army soldiers had died from the flu.
The pandemic was so devastating among WWI nations that some historians have suggested the flu hastened the end of the war. The nations declared armistice on November 11 amid the pandemic’s worst wave.
In April 1919, the flu even disrupted the Paris Peace Conference when President Wilson came down with a debilitating case. As when the British prime minister had contracted the flu back in September, Wilson’s administration hid the news from the public. His personal doctor instead told the press the president had caught a cold from the Paris rain.