
Cartoon – Political and Economic Uncertainties


https://mailchi.mp/d57e5f7ea9f1/the-weekly-gist-january-21-2022?e=d1e747d2d8

It feels like a precarious moment in health systems’ relationships with their doctors. The pandemic has accelerated market forces already at play: mounting burnout, the retirement of Baby Boomer doctors, pressure to grow virtual care, and competition from well-funded insurers, investors and disruptors looking to build their own clinical workforces.
Many health systems have focused system strategy around deepening consumer relationships and loyalty, and quite often we’re told that physicians are roadblocks to consumer-centric offerings (problematic since doctors hold the deepest relationships with a health system’s patients).
When debriefing with a CEO after a health system board meeting, we pointed out the contrast between the strategic level of discussion of most of the meeting with the more granular dialogue around physicians, which focused on the response to a private equity overture to a local, nine-doctor orthopedics practice. It struck us that if this level of scrutiny was applied to other areas, the board would be weighing in on menu changes in food services or selecting throughput metrics for hospital operating rooms.
The CEO acknowledged that while he and a small group of physician leaders have tried to focus on a long-term physician network strategy, “it has been impossible to move beyond putting out the ‘fire of the week’—when it comes to doctors, things that should be small decisions rise to crisis level, and that makes it impossible to play the long game.”
It’s obvious why this happens: decisions involving a small number of doctors can have big implications for short-term, fee-for-service profits, and for the personal incomes of the physicians involved. But if health systems are to achieve ambitious goals, they must find a way to play the long game with their doctors, enfranchising them as partners in creating strategy, and making (and following through on) tough decisions. If physician and system leaders don’t have the fortitude to do this, they’ll continue to find that doctors are a roadblock to transformation.
https://mailchi.mp/d57e5f7ea9f1/the-weekly-gist-january-21-2022?e=d1e747d2d8

Overall health sector M&A activity bounced back in 2021 across nearly every subsector except one: hospitals, which saw a significant decrease in deal volume. Drawing on data from Kaufman Hall, the graphic above shows the scale of the most recent wave of health system consolidation, driven by last year’s eight “mega-mergers” between entities with over $1B in annual revenue each.
While the total number of hospital transactions decreased, the average seller size increased, with the total valuation of all hospital M&A activity nearly tripling from 2020 to 2021. With a dwindling number of independent hospitals left, health systems are pursuing larger combinations with their peers, to achieve greater scale and maintain economic “relevance.”
But as systems who have struggled to complete such mergers can attest, getting a larger deal across the finish line isn’t easy. The path to hospital consolidation now hinges on navigating complex organizational structures and issues of cultural compatibility, in addition to simply identifying “synergies” and avoiding antitrust pitfalls.
https://mailchi.mp/d57e5f7ea9f1/the-weekly-gist-january-21-2022?e=d1e747d2d8

A study of 10M blood samples from active-duty military members, published in the journal Science, found that contracting the Epstein-Barr virus (EBV), best known for causing mononucleosis, was associated with a 32-fold increase in getting an MS diagnosis. While experts were cautious not to conclude that EBV causes MS, it appears to at least be a trigger. What’s left unanswered is how EBV, which is infects an estimated 90 percent of Americans by age 35, leads some to develop MS, while the vast majority do not.
The Gist: It’s rare to have such a large, well-designed epidemiological study show a definitive and clear link between two diseases. Several viruses, including EBV and the human papillomavirus (HPV), have been linked with cancer; while more research is needed, it is theoretically possible vaccines targeted at EBV could reduce the risk of multiple sclerosis and certain cancers, similar to how HPV vaccines have successfully in lowered cervical cancer risk.
And with such a large portion of the global population expected to be infected with COVID-19, it will be critical to monitor whether that virus, too, is linked to the development of other diseases years later.
https://mailchi.mp/d57e5f7ea9f1/the-weekly-gist-january-21-2022?e=d1e747d2d8

The digital health company Babylon recently completed a deal to acquire health kiosk manufacturer Higi Health, followed by an announcement this week that it is also buying episodic care management company DaytoDay Health. London-based Babylon, which went public last October, has moved quickly into the US market, acquiring two independent physician associations in California last year, and expanding its at-risk Medicaid contracts across five states.
The Gist: Babylon has long rejected being called a “virtual care” or “telehealth” company in favor of being called a “digital-first value-based care” company. It now claims to manage more than 350,000 lives worldwide, which are the driving force behind its strong financials.
We’d expect Babylon and other digital-first companies to seek out avenues to “own” attributable lives, as pure-play telemedicine services become increasingly commoditized.
https://mailchi.mp/d57e5f7ea9f1/the-weekly-gist-january-21-2022?e=d1e747d2d8

This week the Biden Administration unveiled actions to make at-home COVID tests and N95 masks available, free of charge, to hundreds of millions of Americans. However, even as US COVID hospitalizations have now surpassed last winter’s previous peak, two newly-approved COVID antiviral drugs remain scarce. Just as fast as Omicron has surged across the country, it may be starting to recede, with cases beginning to drop in several states in the Northeast. Modelers now project the incredibly contagious variant will infect 40 percent of Americans and more than half the human race by the end of March.
The Gist: Absent another significant variant, experts are cautiously optimistic that enough of the US population will soon have either infection-acquired or vaccine-induced immunity that we may be nearing the end of the pandemic, and the beginning of “endemic COVID.”
The US must now shift from COVID “war footing” to learning how to live with the virus long term. That will mean tackling difficult and politically-charged decisions, such as what level of testing and masking are sustainable, and how many COVID deaths we are willing to tolerate.


Net prices of brand-name drugs have increased significantly over the last decade. But savings from generics have driven average prescription prices down in Medicare and Medicaid, Axios’ Caitlin Owens writes about a new analysis by the Congressional Budget Office.
Why it matters: The analysis reiterates that the generic market is largely working as it’s intended to.
By the numbers: The average net price of a prescription fell from $57 in 2009 to $50 in 2018 in Medicare Part D, and from $63 to $48 in Medicaid.

The second year of the pandemic did not dampen UnitedHealth Group’s finances, and the company actually surpassed its initial 2021 revenue and profit projections, Bob writes.
The big picture: UnitedHealth’s revenue has tripled from 2010 to 2021, and profit has almost quadrupled. The company continues to make more of its money from owning doctor groups and controlling pharmacy benefits instead of relying on health insurance.
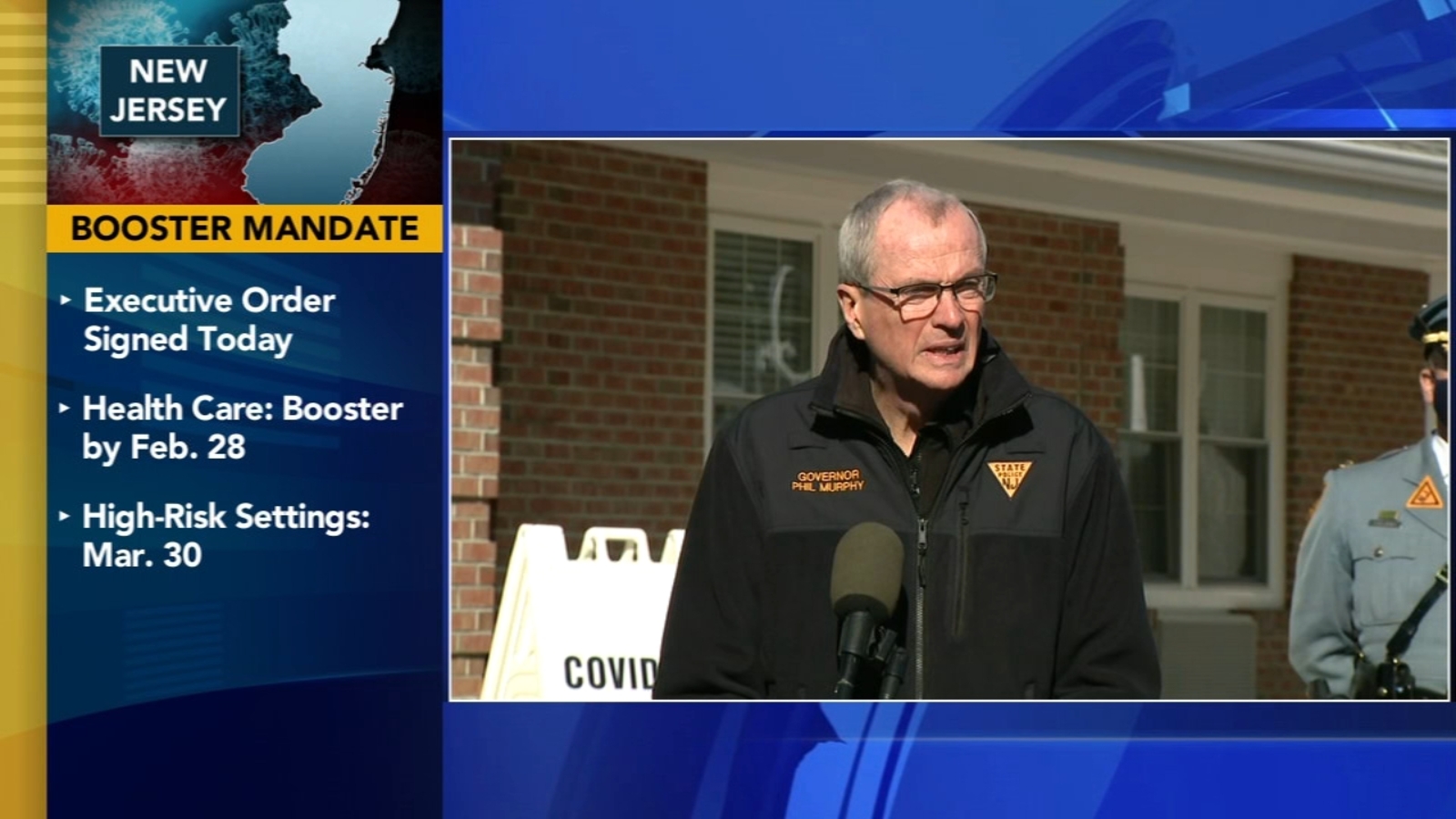
Workers in New Jersey healthcare facilities and high-risk congregate settings like hospitals and nursing homes will be required to be up to date with their COVID-19 vaccinations, including a booster, Gov. Phil Murphy announced Jan. 19.
Mr. Murphy said there would no longer be an option to opt out of vaccination through testing, except for the purposes of providing an accommodation for people exempt from vaccination.
New Jersey healthcare facilities’ covered workers subject to the CMS vaccination mandate for healthcare settings were already required to ensure covered employees received at least one vaccine by Jan. 27 and completed their primary vaccine series by Feb. 28. Mr. Murphy said the state is now requiring proof that these workers are up to date with their vaccination by Feb. 28, which also includes any booster shots for which they are eligible. Noncompliant workers risk losing their jobs.
Workers at covered healthcare settings not subject to the CMS mandate and covered high-risk congregate settings like prisons and jails have until Feb. 16 to receive their first dose of the primary vaccine series and must submit proof that they are up to date with their vaccination by March 30. Mr. Murphy said workers who become newly eligible for a booster after the two deadlines must submit proof of their booster shot within three weeks of becoming eligible.
“With the highly transmissible omicron variant spreading across the country and New Jersey, it is essential that we do everything we can to protect our most vulnerable populations,” Mr. Murphy said in a news release. “With immunity waning approximately five months after a primary COVID-19 vaccination, receiving a booster dose is necessary to protect yourself and those around you. It is critically important that we slow the spread throughout our healthcare and congregate settings in order to protect our vulnerable populations and the staff that care for them.”
The rule in New Jersey, which was issued through an executive order, comes after New York and California also announced booster requirements for healthcare staff.