
Cartoon – Career Counseling




Dubai is proud to introduce its impressive fleet of the “world’s largest ambulances,” or “Mercedes-Benz large-capacity ambulances” which were created to give rapid medical assistance in the event of major emergencies with large numbers of causalities. These new emergency vehicles offer a fully-equipped, mobile clinic with an intensive-care unit and an operating room.
Equipped with an X-ray unit and ultrasonic equipment for further evaluation, each super ambulance bus carries 12,000 liters of oxygen, which ensures a dependable supply for up to three days. With the press of a button, oxygen masks fall from special holders, and the oxygen flow to each mask can be individually controlled.
They’re also equipped with an ECG and an InSpectra shock monitor, which monitors the oxygen saturation in tissue-matter and warns doctors of the onset of shock minutes before it occurs. This unit can also detect and monitor internal bleeding. If an emergency caesarian birth is needed, essential obstetrical instruments, including an incubator, are on board.


Novant Health presented its proposal June 10 to partner with New Hanover Regional Medical Center, a county-owned hospital in Wilmington, N.C. The Winston-Salem, N.C.-based health system is one of three organizations interested in securing the deal.
During the public presentation, Novant Health President and CEO Carl Armato highlighted the system’s financial strength and its potential partnership with Chapel Hill, N.C.-based UNC Health, according to WilmingtonBiz.
In May, Novant, UNC Health and UNC School of Medicine signed a letter of intent to enhance clinical services and medical education at New Hanover Regional if the hospital chooses to form a joint venture with, affiliate with or sell to Novant.
“We are binging, I believe, the best of both worlds: one of the largest not-for-profit health care systems in the country, that’s financially strong, along with UNC Health Care and UNC medical school to really enhance and grow the economic development of Wilmington,” Mr. Armato said, according to WilmingtonBiz.
The 15-hospital system is offering up to $2 billion to New Hanover County, $50 million to the hospital’s foundation to fund unmet community needs and an investment of $3.1 billion in capital projects over the next decade, according to the report.
“We actually proposed a very significant financial commitment to New Hanover Regional Medical Center, that local board, that management team, that community — your community,” Mr. Armato said, according to the report. “And we want you to know that we have the resources to back that up.”
Novant made its proposal the day after Durham, N.C.-based Duke Health pitched its deal for New Hanover Regional. Charlotte, N.C.-based Atrium Health, the third health system trying to secure a deal with the hospital, will make its presentation June 11.

Trinity Health saw revenue decline in the first nine months of fiscal year 2020, and the Livonia, Mich.-based health system ended the period with an operating loss, according to unaudited financial documents.
Trinity Health saw revenue decline less than 1 percent year over year to $14.2 billion in the first nine months of the fiscal year, which ended March 31. The health system attributed the drop in revenue to the COVID-19 pandemic and the divestiture of Camden, N.J.-based Lourdes Health System in June 2019.
The 92-hospital system’s expenses were also up 1.2 percent year over year. Trinity Health ended the first three quarters of fiscal 2020 with expenses of $14.3 billion. Same-hospital expense growth was driven by increases in labor and supply costs, purchased services and costs related to its conversion to the Epic EHR platform in the Michigan region. The health system said the pandemic added $14.1 million of costs in March.
Trinity Health has taken several steps to reduce operating and capital spending in response to the pandemic, including implementing furloughs and reducing salaries for executives. In early April, Trinity Health announced plans to furlough 2,500 employees, most of whom are in nonclinical roles.
Trinity Health reported an operating loss of $103.5 million for the first nine months of the current fiscal year, compared to operating income of $115.2 million in the same period a year earlier.
After factoring in investments and other nonoperating items, Trinity Health posted a net loss of $883.5 million in the first three quarters of fiscal 2020, down from net income of $457.9 million a year earlier. Nonoperating losses in the first nine months of fiscal 2020 were primarily driven by the pandemic’s effect on global investment market conditions in March, the health system said.
To help offset financial damage, Trinity Health received funds from the $175 billion in relief aid Congress has allocated to hospitals and other healthcare providers to cover expenses and lost revenue tied to the pandemic. The health system said it received a total of $600 million in federal grants in April and May.
Trinity Health also applied for and received $1.6 billion of Medicare advance payments, which must be repaid.
Though Trinity Health is unable to forecast the pandemic’s impact on its financial position, it said the ultimate effect of COVID-19 on its operating margins and financial results “is likely to be adverse and significant.”

The effects of racism are often inseparable from black Americans’ health and well-being, as “black communities bear the physical burdens of centuries of injustice, toxic exposures, racism, and white supremacist violence,” Rachel Hardeman, Eduardo Medina and Rhea Boyd write in the New England Journal of Medicine:
Any solution to racial health inequities must be rooted in the material conditions in which those inequities thrive. Therefore, we must insist that for the health of the black community and, in turn, the health of the nation, we address the social, economic, political, legal, educational, and health care systems that maintain structural racism. Because as the Covid-19 pandemic so expeditiously illustrated, all policy is health policy…
The response to the pandemic has made at least one thing clear: systemic change can in fact happen overnight.
The inequalities in American health care extend right into the hospital: Cash-strapped safety-net hospitals treat more people of color, while wealthier facilities treat more white patients.
Why it matters: Safety-net hospitals lack the money, equipment and other resources of their more affluent counterparts, which makes providing critical care more difficult and exacerbates disparities in health outcomes.
The big picture: A majority of patients who go to safety-net hospitals are black or Hispanic; 40% are either on Medicaid or uninsured.
The other side: Wealthy hospitals, including many prominent academic medical centers, are “far less likely to serve or treat black and low-income patients even though those patients may live in their backyards,” said Arrianna Planey, an incoming health policy professor at the University of North Carolina.
Between the lines: The way the federal government is bailing out hospitals for the revenues they’ve lost during coronavirus is exacerbating this inequality. More money is flowing to richer hospitals.
The bottom line: Poor hospitals that treat minorities have had to rely on GoFundMe pages and beg for ventilators during the pandemic, while richer systems move ahead with new hospital construction plans.
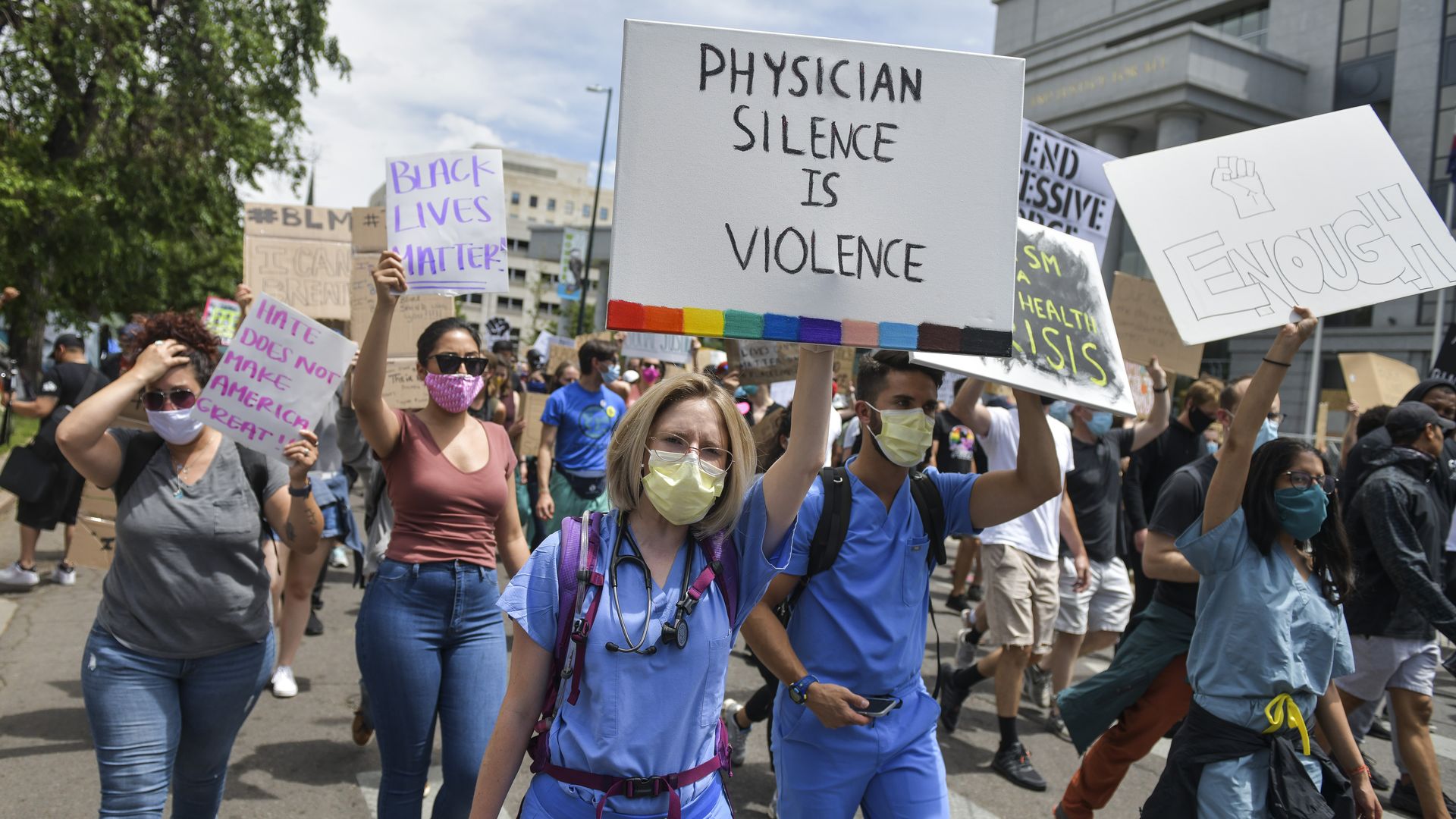
When protests broke out against the coronavirus lockdown, many public health experts were quick to warn about spreading the virus. When protests broke out after George Floyd’s death, some of the same experts embraced the protests. That’s led to charges of double standards among scientists.
Why it matters: Scientists who are seen as changing recommendations based on political and social priorities, however important, risk losing public trust. That could cause people to disregard their advice should the pandemic require stricter lockdown policies.
What’s happening: Many public health experts came out against public gatherings of almost any sort this spring — including protests over lockdown policies and large religious gatherings.
Yes, but: Spending time in a large group, even outdoors and wearing masks — as many of the protesters are — does raise the risk of coronavirus transmission, says Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota.
The difference in tone between how some public health experts are viewing the current protests and earlier ones focused on the lockdowns themselves was seized upon by a number of critics, as well as the Trump campaign.
The current debate underscores a larger question: What role should scientists play in policymaking?
The big picture: The debate risks exacerbating a partisan divide among Americans in their reported trust in scientists.
What to watch: If there is a rise in new cases in the coming weeks, there will be pressure to trace them — to protests, rallies and the reopening of states. How experts weigh in could affect how their recommendations will be viewed in the future — and whether the public, whatever their political leanings, will follow them again.