
Cartoon – The Mark of True Leadership




The coronavirus pandemic is shaking bedrock assumptions about U.S. exceptionalism. This is perhaps the first global crisis in more than a century where no one is even looking for Washington to lead.
As images of America’s overwhelmed hospital wards and snaking jobless lines have flickered across the world, people on the European side of the Atlantic are looking at the richest and most powerful nation in the world with disbelief.
“When people see these pictures of New York City they say, ‘How can this happen? How is this possible?’” said Henrik Enderlein, president of the Berlin-based Hertie School, a university focused on public policy. “We are all stunned. Look at the jobless lines. Twenty-two million,” he added.
“I feel a desperate sadness,” said Timothy Garton Ash, a professor of European history at Oxford University and a lifelong and ardent Atlanticist.
The pandemic sweeping the globe has done more than take lives and livelihoods from New Delhi to New York. It is shaking fundamental assumptions about American exceptionalism — the special role the United States played for decades after World War II as the reach of its values and power made it a global leader and example to the world.
Today it is leading in a different way: More than 840,000 Americans have been diagnosed with Covid-19 and at least 46,784 have died from it, more than anywhere else in the world.
As the calamity unfolds, President Trump and state governors are not only arguing over what to do, but also over who has the authority to do it. Mr. Trump has fomented protests against the safety measures urged by scientific advisers, misrepresented facts about the virus and the government response nearly daily, and this week used the virus to cut off the issuing of green cards to people seeking to emigrate to the United States.
“America has not done badly, it has done exceptionally badly,” said Dominique Moïsi, a political scientist and senior adviser at the Paris-based Institut Montaigne.
The pandemic has exposed the strengths and weaknesses of just about every society, Mr. Moïsi noted. It has demonstrated the strength of, and suppression of information by, an authoritarian Chinese state as it imposed a lockdown in the city of Wuhan. It has shown the value of Germany’s deep well of public trust and collective spirit, even as it has underscored the country’s reluctance to step up forcefully and lead Europe.
And in the United States, it has exposed two great weaknesses that, in the eyes of many Europeans, have compounded one another: the erratic leadership of Mr. Trump, who has devalued expertise and often refused to follow the advice of his scientific advisers, and the absence of a robust public health care system and social safety net.
“America prepared for the wrong kind of war,” Mr. Moïsi said. “It prepared for a new 9/11, but instead a virus came.”
“It raises the question: Has America become the wrong kind of power with the wrong kind of priorities?” he asked.
Ever since Mr. Trump moved into the White House and turned America First into his administration’s guiding mantra, Europeans have had to get used to the president’s casual willingness to risk decades-old alliances and rip up international agreements. Early on, he called NATO “obsolete” and withdrew U.S. support from the Paris climate agreement and the Iran nuclear deal.
But this is perhaps the first global crisis in more than a century where no one is even looking to the United States for leadership.
In Berlin, Germany’s foreign minister, Heiko Maas, has said as much.
China took “very authoritarian measures, while in the U.S., the virus was played down for a long time,” Mr. Maas recently told Der Spiegel magazine.
“These are two extremes, neither of which can be a model for Europe,” Mr. Maas said.
America once told a story of hope, and not just to Americans. West Germans like Mr. Maas, who grew up on the front line of the Cold War, knew that story by heart, and like many others in the world, believed it.
But nearly three decades later, America’s story is in trouble.
The country that helped defeat fascism in Europe 75 years ago next month, and defended democracy on the continent in the decades that followed, is doing a worse job of protecting its own citizens than many autocracies and democracies.
There is a special irony: Germany and South Korea, both products of enlightened postwar American leadership, have become potent examples of best practices in the coronavirus crisis.
But critics now see America failing not only to lead the world’s response, but letting down its own people as well.
“There is not only no global leadership, there is no national and no federal leadership in the United States,” said Ricardo Hausmann, director of the Growth Lab at Harvard’s Center for International Development. “In some sense this is the failure of leadership of the U.S. in the U.S.”
Of course, some countries in Europe have also been overwhelmed by the virus, with the number of dead from Covid-19 much higher as a percentage of the population in Italy, Spain and France than in the United States. But they were struck sooner and had less time to prepare and react.
The contrast between how the United States and Germany responded to the virus is particularly striking.
While Chancellor Angela Merkel has been criticized for not taking a forceful enough leadership role in Europe, Germany is being praised for a near-textbook response to the pandemic, at least by Western standards. That is thanks to a robust public health care system, but also a strategy of mass testing and trusted and effective political leadership.
Ms. Merkel has done what Mr. Trump has not. She has been clear and honest about the risks with voters and swift in her response. She has rallied all 16 state governors behind her. A trained physicist, she has followed scientific advice and learned from best practice elsewhere.
Not long ago, Ms. Merkel was considered a spent force, having announced that this would be her last term. Now her approval ratings are at 80 percent.
“She has the mind of a scientist and the heart of a pastor’s daughter,” Mr. Garton Ash said.
Mr. Trump, in a hurry to restart the economy in an election year, has appointed a panel of business executives to chart a course out of the lockdown.
Ms. Merkel, like everyone, would like to find a way out, too, but this week she warned Germans to remain cautious. She is listening to the advice of a multidisciplinary panel of 26 academics from Germany’s national academy of science. The panel includes not just medical experts and economists but also behavioral psychologists, education experts, sociologists, philosophers and constitutional experts.
“You need a holistic approach to this crisis,” said Gerald Haug, the academy’s president, who chairs the German panel. “Our politicians get that.”
A climatologist, Mr. Haug used to do research at Columbia University in New York.
The United States has some of the world’s best and brightest minds in science, he said. “The difference is, they’re not being listened to.”
“It’s a tragedy,” he added.
Some cautioned that the final history of how countries fare after the pandemic is still a long way from being written.
A pandemic is a very specific kind of stress test for political systems, said Mr. Garton Ash, the history professor. The military balance of power has not shifted at all. The United States remains the world’s largest economy. And it was entirely unclear what global region would be best equipped to kick-start growth after a deep recession.
“All of our economies are going to face a terrible test,” he said. “No one knows who will come out stronger at the end.”
Benjamin Haddad, a French researcher at the Atlantic Council, wrote that while the pandemic was testing U.S. leadership, it is “too soon to tell” if it would do long-term damage.
“It is possible that the United States will resort to unexpected resources, and at the same time find a form of national unity in its foreign policy regarding the strategic rivalry with China, which it has been lacking until now,” Mr. Haddad wrote.
There is another wild card in the short term, Mr. Moïsi pointed out. The United States has an election in November. That, and the aftermath of the deepest economic crisis since the 1930s, might also affect the course of history.
The Great Depression gave rise to America’s New Deal. Maybe the coronavirus will lead the United States to embrace a stronger public safety net and develop a national consensus for more accessible health care, Mr. Moïsi suggested.
“Europe’s social democratic systems are not only more human, they leave us better prepared and fit to deal with a crisis like this than the more brutal capitalistic system in the United States,” Mr. Moïsi said.
The current crisis, some fear, could act like an accelerator of history, speeding up a decline in influence of both the United States and Europe.
“Sometime in 2021 we come out of this crisis and we will be in 2030,” said Mr. Moïsi. “There will be more Asia in the world and less West.”
Mr. Garton Ash said that the United States should take an urgent warning from a long line of empires that rose and fell.
“To a historian it’s nothing new, that’s what happens,” said Mr. Garton Ash. “It’s a very familiar story in world history that after a certain amount of time a power declines.”
“You accumulate problems, and because you’re such a strong player, you can carry these dysfunctionalities for a long time,” he said. “Until something happens and you can’t anymore.”
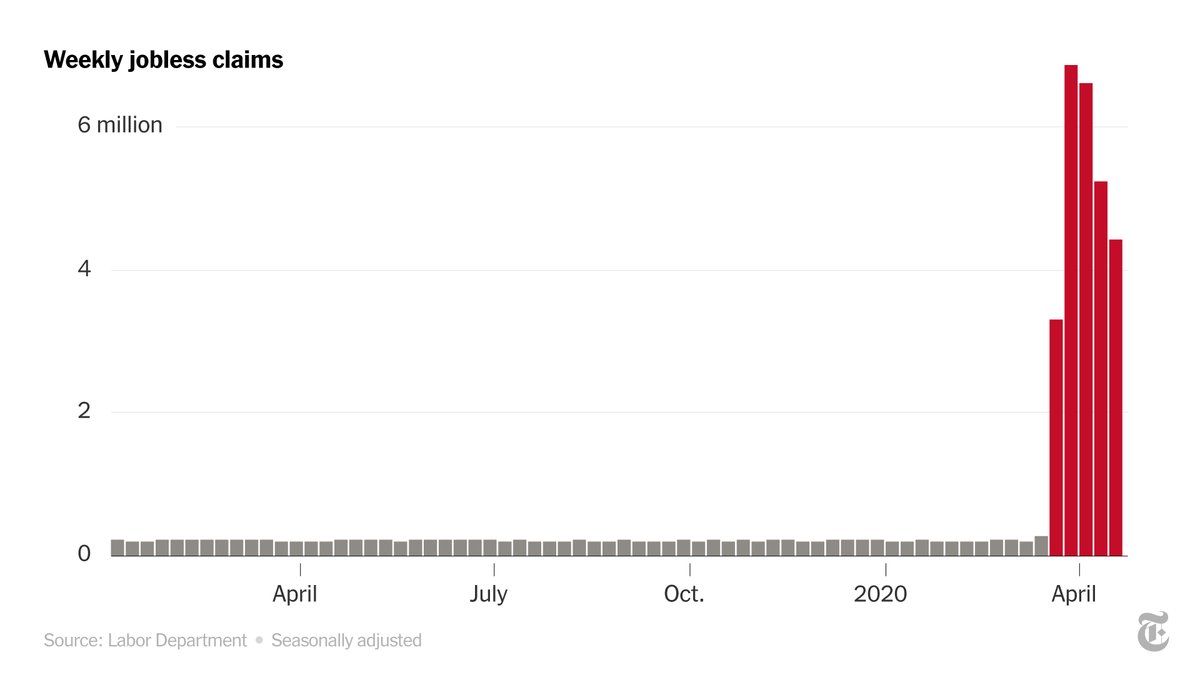
With 4.4 million added last week, the five-week total passed 26 million. The struggle by states to field claims has hampered economic recovery.
Nearly a month after Washington rushed through an emergency package to aid jobless Americans, millions of laid-off workers have still not been able to apply for those benefits — let alone receive them — because of overwhelmed state unemployment systems.
Across the country, states have frantically scrambled to handle a flood of applications and apply a new set of federal rules even as more and more people line up for help. On Thursday, the Labor Department reported that another 4.4 million people filed initial unemployment claims last week, bringing the five-week total to more than 26 million.
“At all levels, it’s eye-watering numbers,” Torsten Slok, chief international economist at Deutsche Bank Securities, said. Nearly one in six American workers has lost a job in recent weeks.
Delays in delivering benefits, though, are as troubling as the sheer magnitude of the figures, he said. Such problems not only create immediate hardships, but also affect the shape of the recovery when the pandemic eases.
Laid-off workers need money quickly so that they can continue to pay rent and credit card bills and buy groceries. If they can’t, Mr. Slok said, the hole that the larger economy has fallen into “gets deeper and deeper, and more difficult to crawl out of.”
Hours after the Labor Department report, the House passed a $484 billion coronavirus relief package to replenish a depleted small-business loan program and fund hospitals and testing. The Senate approved the bill earlier this week.
Even as Congress continues to provide aid, distribution has remained challenging. According to the Labor Department, only 10 states have started making payments under the federal Pandemic Unemployment Assistance program, which extends coverage to freelancers, self-employed workers and part-timers. Most states have not even completed the system needed to start the process.
Ohio, for example, will not start processing claims under the expanded federal eligibility criteria until May 15. Recipients whose state benefits ran out, but who can apply for extended federal benefits, will not begin to have their claims processed until May 1.
Pennsylvania opened its website for residents to file for the federal program a few days ago, but some applicants were mistakenly told that they were ineligible after filling out the forms. The state has given no timetable for when benefits might be paid.
Reports of delays, interruptions and glitches continue to come in from workers who have been unable to get into the system, from others who filed for regular state benefits but have yet to receive them, and from applicants who say they have been unfairly turned down and unable to appeal.
Florida has paid just 17 percent of the claims filed since March 15, according to the state’s Department of Economic Opportunity.
“Speed matters” when it comes to government assistance, said Carl Tannenbaum, chief economist at Northern Trust. Speed can mean the difference between a company’s survival and its failure, or between making a home mortgage payment and facing foreclosure.
There is “a race between policy and a pandemic,” Mr. Tannenbaum said, and in many places, it is clear that the response has been “very uneven.”
Using data reported by the Labor Department for March 14 to April 11, the Economic Policy Institute, a liberal research group, estimated that seven in 10 applicants were receiving benefits. That left seven million other jobless workers who had filed claims but were still waiting for relief.
States manage their own unemployment insurance programs and set the level of benefits and eligibility rules. Now they are responsible for administering federal emergency benefits that provide payments for an additional 13 weeks, cover previously ineligible workers and add $600 to the regular weekly check.
So far, 44 states have begun to send the $600 supplement to jobless workers who qualified under state rules, the Labor Department said. Only two — Kentucky and Minnesota — have extended federal benefits to workers who have used up their state allotment.
With government phones and websites clogged and drop-in centers closed, legal aid lawyers around the country are fielding complaints from people who say they don’t know where else to turn.
“Our office has received thousands of calls,” said John Tirpak, a lawyer with the Unemployment Law Project, a nonprofit group in Washington.
People with disabilities and nonnative English speakers have had particular problems, he said.
Even those able to file initially say they have had trouble getting back into the system as required weekly to recertify their claims.
Colin Harris of Marysville, Wash., got a letter on March 31 from the state’s unemployment insurance office saying he was eligible for benefits after being laid off as a quality inspector at Safran Cabin, an aerospace company. He submitted claims two weeks in a row and heard nothing. When he submitted his next claim, he was told that he had been disqualified. He has tried calling more than 200 times since then, with no luck.
“And that’s still where I am right now,” he said, “unable to talk to somebody to find out what the issue is.” If he had not received a $1,200 stimulus check from the federal government, he said, he would not have been able to make his mortgage payment.
Last week’s tally of new claims was lower than each of the previous three weeks. But millions of additional claims are still expected to stream in from around the country over the next month, while hiring remains piddling.
States are frantically trying to catch up. California, which has processed 2.7 million claims over the last four weeks, opened a second call center on Monday. New York, which has deployed 3,100 people to answer the telephone, said this week that it had reduced the backlog that accumulated by April 8 to 4,305 from 275,000.
Florida had the largest increase in initial claims last week, although the state figures, unlike the national total, are not seasonally adjusted. That increase could be a sign that jobless workers finally got access to the system after delays, but it is impossible to assess how many potential applicants have still failed to get in.
The 10 states that have started making Pandemic Unemployment Assistance payments to workers who would not normally qualify under state guidelines are Alabama, Colorado, Iowa, Kentucky, Louisiana, Massachusetts, Rhode Island, Tennessee, Texas and Utah.
Pain is everywhere, but it is most widespread among the most vulnerable.
In a survey that the Pew Research Center released on Tuesday, 52 percent of low-income households — below $37,500 a year for a family of three — said someone in the household had lost a job because of the coronavirus, compared with 32 percent of upper-income ones (with earnings over $112,600). Forty-two percent of families in the middle have been affected as well.
Those without a college education have taken a disproportionate hit, as have Hispanics and African-Americans, the survey found.
An outsize share of jobless claims have also been filed by women, according to an analysis from the Fuller Project, a nonprofit journalism organization that focuses on women.
Josalyn Taylor, 31, learned that she was out of a job on March 16. “I clocked in at 3 o’clock, and by 3:30 my boss called me and told me we were going to shut down for three weeks,” said Ms. Taylor, an assistant manager at Cicis Pizza in Galveston, Tex. The restaurant has yet to reopen.
Two days later, she applied for unemployment insurance, but she kept receiving a message that a claim was already active for her Social Security number and that she could not file. She has tried to clear up the matter hundreds of times — online, by phone and through the Texas Workforce Commission’s site on Facebook — with no luck.
“I used my stimulus check to pay my light bill, and I’m using that to keep groceries and stuff in the house,” said Ms. Taylor, who is five months pregnant. “But other than that, I don’t have any other income, and I’m almost out of money.”
The first wave of layoffs most heavily whacked the restaurant, travel, personal care, retail and manufacturing industries, but the damage has spread to a much broader range of sectors.
At the online job site Indeed, for example, postings for software development jobs are down nearly 30 percent from last year, while listings for finance and banking openings are down more than 40 percent.
New layoffs are expected to ease over the next couple of months, but the damage to the economy is likely to last much longer. In a matter of weeks, the shutdown has more than erased 10 years of net job gains — more than 19 million jobs.
Health and education are going to revive relatively quickly, said Rick Rieder, chief investment officer for global fixed income at BlackRock, but leisure and hospitality are going to take a lot longer.
“A lot of the people who have been furloughed won’t come back,” he said. “Companies will either close or decide not to take back those workers.”
Over the past decade, the employment landscape has shifted substantially as new types of jobs have appeared and old categories have disappeared. The U.S. economy, Mr. Rieder said, is “going to go through another period of evolution.”
https://mailchi.mp/0d4b1a52108c/the-weekly-gist-april-24-2020?e=d1e747d2d8

It’s entirely understandable that consumers would be reticent to visit in-person care settings right now. Given that doctors’ offices and urgent care facilities are where sick people congregate, a patient might well assume their chances of contracting COVID-19 would be higher there than in almost any other public space. But a story we heard this week from a health system chief strategy officer (CSO) reveals just how frightened patients may be to return.
Last week the system began to reach out to patients who had positive screening mammograms in February, before elective procedures and tests were cancelled, and who now needed to return for more detailed diagnostic images. A full 75 percent of these patients were unwilling to schedule a diagnostic mammogram within the next month, with one patient even saying, “I’ll take my chances with breast cancer over COVID!”.
Women with a concerning mammogram finding are typically among the most motivated patients in seeking follow-up care. If a majority of them are unwilling to pursue in-person follow-up, the same will likely be true of scores of patients with other possible cancers, heart disease, and other serious conditions. As fear delays needed care, patients are likely to end up much sicker, with more advanced disease, when they do return. With rigorous attention to symptom and temperature screening, visiting a doctor’s office should be less risky than going to the grocery store—but providers will have to publicly communicate the steps they are taking to keep patients safe before many will be willing to come in the door.
https://mailchi.mp/0d4b1a52108c/the-weekly-gist-april-24-2020?e=d1e747d2d8
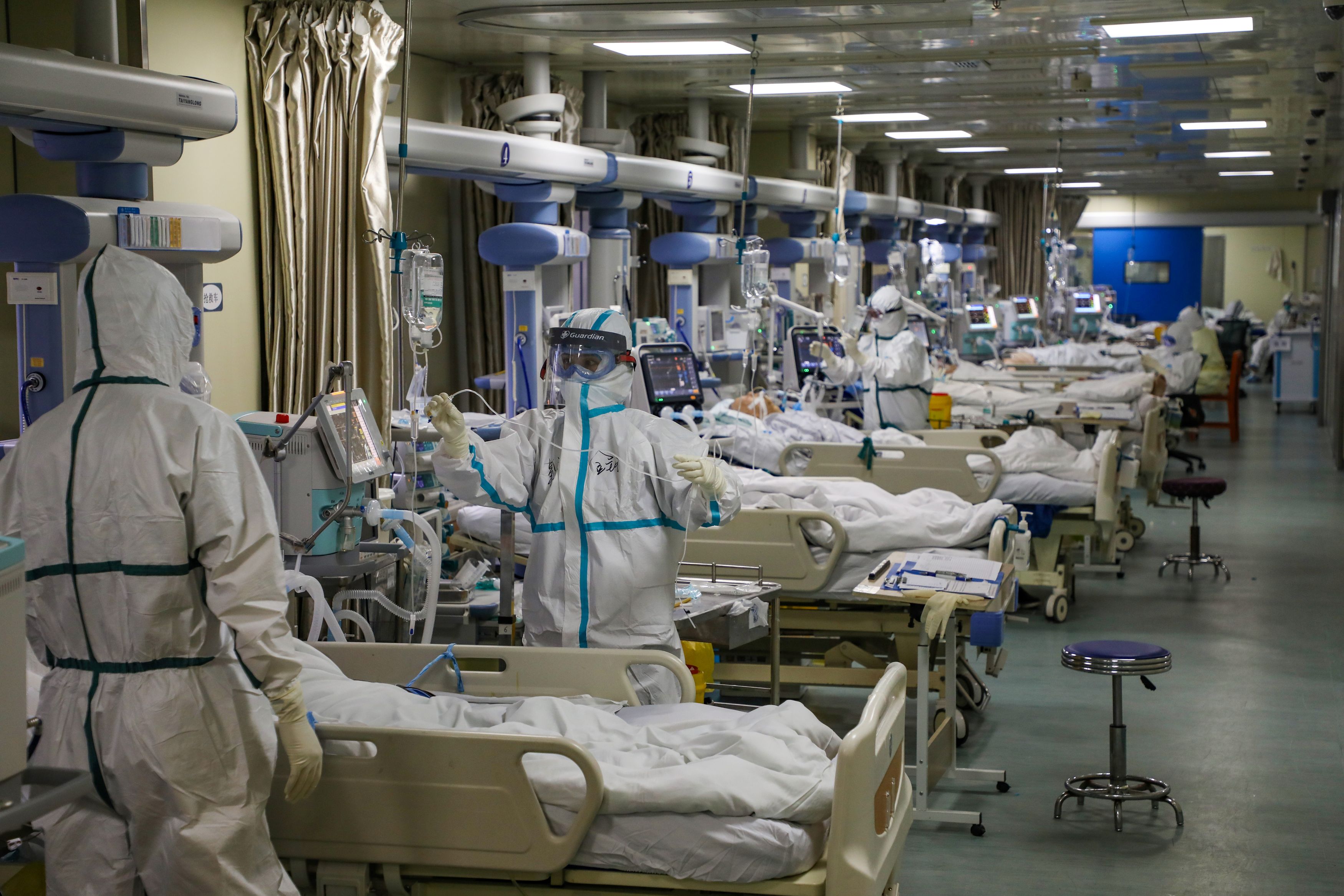
A study published this week in JAMA provides a look at the largest series of COVID-19 hospitalized patients studied to date in the US, reporting that almost all patients treated had at least one underlying condition. Physicians from Northwell Health evaluated the outcomes, comorbidities and clinical course of 5,700 confirmed coronavirus patients hospitalized between March 1st and April 4th across the New York City area. Hospitalized patients, 60 percent of whom were men, had a high burden of chronic disease.
Similar to other reports, older patients, and those with a higher chronic disease burden (especially diabetes) were both more likely to require mechanical ventilation, and more likely to die. Only nine of the 436 patients under age 50 who had no significant cormorbidities (as measured by the Charlson Comorbidity Index) had died. One number received the most press coverage: as reported in the abstract, 88 percent of patients who received mechanical ventilation died. Digging into the details of the series, this may end up being an overestimation, as the statistic is based on a subset of 320 ventilated patients who either died or were discharged by April 4th. At that time, 831 patients remained in the hospital on ventilators, with outcomes still to be determined. Ultimately, the mortality rate of full cohort of ventilated patients could fall nearer to the 50-60 percent range seen in other studies.
Regardless, the rich dataset of the Northwell report adds to the body of evidence that severe COVID-19 infections and deaths involve several organ systems. This Science article provides a thorough (and comprehensible to the non-clinician) review of how the virus invades the body. While the lungs remain “ground zero” for infection, critically ill patients may experience serious kidney, cardiac, or even nervous system involvement. A host of chronic diseases predispose patients for worse outcomes—yet doctors remain puzzled that they aren’t seeing “a huge number of asthmatics” in ICUs. Patients are presenting with dangerously low oxygen levels but less distress than expected, likely because they are able to still “blow off” carbon dioxide, limiting the body’s ability to sense the seriousness of their condition.
Many dying patients are overwhelmed by a “cytokine storm”—an overreaction of the immune system that compounds organ failure. And new evidence suggests that large numbers of critically ill patients may experience abnormal blood clotting, contributing to the high mortality rates of the disease. The more doctors and scientists learn about coronavirus, the more complex the disease process seems—leaving doctors with work to do to understand, manage, and treat the tens of thousands of these seriously ill patients.
https://mailchi.mp/0d4b1a52108c/the-weekly-gist-april-24-2020?e=d1e747d2d8

National physician staffing firm Envision Healthcare is considering filing for bankruptcy, according a report from Bloomberg. Sources say the company, backed by private equity (PE) firm KKR, which acquired Envision for $9.9B in June 2018, has hired restructuring advisors and is working with an investment bank. The abrupt halt to elective surgeries and reduction in emergency room volumes due to COVID-19 has caused Envision’s business to shrink by 65 to 75 percent in just two weeks at its 168 open ambulatory surgery centers (ASCs), compared to the same time period last year.
The Nashville-based company, which employs over 25,000 physicians and advanced practitioners, has already been reducing pay for providers and executives, in addition to implementing temporary furloughs. Envision is also struggling with a debt load of more than $7B, resulting from its 2018 leveraged buyout, and has been unable to convince its bondholders to approve a debt swap.
It remains to be seen whether Envision will be a bellwether for how other PE-backed physician groups will weather the ongoing COVID crisis. While Envision’s composition of mainly hospital- and ASC-based providers, coupled with its huge debt load, leave it on especially shaky financial footing, many PE-backed physician groups will struggle this year to achieve anything close to the 20 percent annual rate of return often promised to investors.
If high-profile PE-backed groups like Envision end up declaring bankruptcy, it will likely impact the calculus of the many independent practices which may have previously looked to PE firms for acquisition, and temper the enthusiasm of investors, who might see physician staffing and practice roll-ups as less attractive as volumes continue to fluctuate.
https://mailchi.mp/0d4b1a52108c/the-weekly-gist-april-24-2020?e=d1e747d2d8

The death toll from the novel coronavirus continued to mount this week, with more than 50,000 deaths reported in the US, and over 900,000 confirmed cases nationwide. Globally, the disease has infected more than 2.7M people and killed nearly 200,000. On Tuesday, public health officials in California announced that two people who died in Santa Clara County in early February were victims of COVID-19, making them the earliest known fatalities in the US, and altering experts’ understanding of how long the disease has been spreading in the country. New modeling from researchers at Northeastern University this week suggested that the virus may have been spreading widely in several cities by early February, but went undetected because of restrictions on testing.
National attention has remained focused on the subject of testing, as states and localities scramble to secure enough testing supplies and equipment to allow them to understand community spread and identify new cases. President Trump signed an emergency $484B relief bill on Friday that will provide $25B to ramp up testing, give additional aid to businesses forced to shutter, and send hospitals $75B in additional emergency funding.
The new money for hospitals is in addition to $100B already approved by Congress for a “provider relief fund” as part of the CARES Act. Having already distributed $30B of the initial grant money to hospitals, the Department of Health and Human Services (HHS) was expected to pay out an additional $20B today, this time according to a formula based on the net patient revenue of each hospital, rather than the earlier approach based on Medicare billings. The shift is expected to address concerns among children’s hospitals, safety-net providers, and others who were disadvantaged by the Medicare-based approach. It is unclear how the newly approved $75B of additional funding will be allocated.
Meanwhile, states began to plan for the reopening of their economies, with most governors taking a measured approach in coordination with neighboring states. A handful of states moved to loosen stay-at-home restrictions in advance of meeting the Trump administration’s “gating” criteria, including Florida, which reopened some beaches for recreational use, Oklahoma, and Georgia, which controversially allowed gyms, bowling alleys, hair and nail salons, and tattoo parlors to reopen on Friday.
Many states began to put in place plans to restart elective surgeries, which had been curtailed by a patchwork of differing state and local directives. The Centers for Medicare and Medicaid Services (CMS) released guidelines this week to help local officials decide when and how to restart surgeries. Whether for healthcare services or other types of economic activity, states will (and should) be guided by the ability to conduct widespread testing, robust contact tracing, and isolation of those infected with the virus. Ensuring that ability will likely make the next phase of the pandemic a protracted and frustrating “dance” of fits and starts, likely to last into the summer months and beyond.

Oxley gasped when he got to the patient’s age and covid-19 status: 44, positive.
The man was among several recent stroke patients in their 30s to 40s who were all infected with the coronavirus. The median age for that type of severe stroke is 74.
As Oxley, an interventional neurologist, began the procedure to remove the clot, he observed something he had never seen before. On the monitors, the brain typically shows up as a tangle of black squiggles — “like a can of spaghetti,” he said — that provide a map of blood vessels. A clot shows up as a blank spot. As he used a needlelike device to pull out the clot, he saw new clots forming in real-time around it.
“This is crazy,” he remembers telling his boss.
Reports of strokes in the young and middle-aged — not just at Mount Sinai, but also in many other hospitals in communities hit hard by the novel coronavirus — are the latest twist in our evolving understanding of its connected disease, covid-19. Even as the virus has infected nearly 2.8 million people worldwide and killed about 195,000 as of Friday, its biological mechanisms continue to elude top scientific minds. Once thought to be a pathogen that primarily attacks the lungs, it has turned out to be a much more formidable foe — impacting nearly every major organ system in the body.
Until recently, there was little hard data on strokes and covid-19.
There was one report out of Wuhan, China, that showed that some hospitalized patients had experienced strokes, with many being seriously ill and elderly. But the linkage was considered more of “a clinical hunch by a lot of really smart people,” said Sherry H-Y Chou, a University of Pittsburgh Medical Center neurologist and critical care doctor.
Now for the first time, three large U.S. medical centers are preparing to publish data on the stroke phenomenon. The numbers are small, only a few dozen per location, but they provide new insights into what the virus does to our bodies.
A stroke, which is a sudden interruption the blood supply, is a complex problem with numerous causes and presentations. It can be caused by heart problems, clogged arteries due to cholesterol, even substance abuse. Mini-strokes often don’t cause permanent damage and can resolve on their own within 24 hours. But bigger ones can be catastrophic.
The analyses suggest coronavirus patients are mostly experiencing the deadliest type of stroke. Known as large vessel occlusions, or LVOs, they can obliterate large parts of the brain responsible for movement, speech and decision-making in one blow because they are in the main blood-supplying arteries.
Many researchers suspect strokes in covid-19 patients may be a direct consequence of blood problems that are producing clots all over some people’s bodies.
Clots that form on vessel walls fly upward. One that started in the calves might migrate to the lungs, causing a blockage called a pulmonary embolism that arrests breathing — a known cause of death in covid-19 patients. Clots in or near the heart might lead to a heart attack, another common cause of death. Anything above that would probably go to the brain, leading to a stroke.
Robert Stevens, a critical care doctor at Johns Hopkins Hospital in Baltimore, called strokes “one of the most dramatic manifestations” of the blood-clotting issues. “We’ve also taken care of patients in their 30s with stroke and covid, and this was extremely surprising,” he said.
Many doctors expressed worry that as the New York City Fire Department was picking up four times as many people who died at home as normal during the peak of infection that some of the dead had suffered sudden strokes. The truth may never be known because few autopsies were conducted.
Chou said one question is whether the clotting is because of a direct attack on the blood vessels, or a “a friendly-fire problem” caused by the patient’s immune response.
“In your body’s attempt to fight off the virus, does the immune response end up hurting your brain?” she asked. Chou is hoping to answer such questions through a review of strokes and other neurological complications in thousands of covid-19 patients treated at 68 medical centers in 17 countries.
Thomas Jefferson University Hospitals, which operates 14 medical centers in Philadelphia, and NYU Langone Health in New York City, found that 12 of their patients treated for large blood blockages in their brains during a three-week period had the virus. Forty percent were under 50, and they had few or no risk factors. Their paper is under review by a medical journal, said Pascal Jabbour, a neurosurgeon at Thomas Jefferson.
Jabbour and his co-author Eytan Raz, an assistant professor of neuroradiology at NYU Langone, said that strokes in covid-19 patients challenge conventional thinking. “We are used to thinking of 60 as a young patient when it comes to large vessel occlusions,” Raz said of the deadliest strokes. “We have never seen so many in their 50s, 40s and late 30s.”
Raz wondered whether they are seeing more young patients because they are more resistant than the elderly to the respiratory distress caused by covid-19: “So they survive the lung side, and in time develop other issues.”
Jabbour said many cases he has treated have unusual characteristics. Brain clots usually appear in the arteries, which carry blood away from the heart. But in covid-19 patients, he is also seeing them in the veins, which carry blood in the opposite direction and are trickier to treat. Some patients are also developing more than one large clot in their heads, which is highly unusual.
“We’ll be treating a blood vessel and it will go fine, but then the patient will have a major stroke” because of a clot in another part of the brain, he said.
At Mount Sinai, the largest medical system in New York City, physician-researcher J Mocco said the number of patients coming in with large blood blockages in their brains doubled during the three weeks of the covid-19 surge to more than 32, even as the number of other emergencies fell. More than half of were covid-19 positive.
It isn’t just the number of patients that was unusual. The first wave of the pandemic has hit the elderly and those with heart disease, diabetes, obesity or other preexisting conditions disproportionately. The covid-19 patients treated for stroke at Mount Sinai were younger and mostly without risk factors.
On average, the covid-19 stroke patients were 15 years younger than stroke patients without the virus.
“These are people among the least likely statistically to have a stroke,” Mocco said.
Mocco, who has spent his career studying strokes and how to treat them, said he was “completely shocked” by the analysis. He noted the link between covid-19 and stroke “is one of the clearest and most profound correlations I’ve come across.”
“This is much too powerful of a signal to be chance or happenstance,” he said.
In a letter to be published in the New England Journal of Medicine next week, the Mount Sinai team details five case studies of young patients who had strokes at home from March 23 to April 7. They make for difficult reading: The victims’ ages are 33, 37, 39, 44 and 49, and they were all home when they began to experience sudden symptoms, including slurred speech, confusion, drooping on one side of the face and a dead feeling in one arm.
One died, two are still hospitalized, one was released to rehabilitation, and one was released home to the care of his brother. Only one of the five, a 33-year-old woman, is able to speak.
Oxley, the interventional neurologist, said one striking aspect of the cases is how long many waited before seeking emergency care.
The 33-year-old woman was previously healthy but had a cough and headache for about a week. Over the course of 28 hours, she noticed her speech was slurred and that she was going numb and weak on her left side but, the researchers wrote, “delayed seeking emergency care due to fear of the covid-19 outbreak.”
It turned out she was already infected.
By the time she arrived at the hospital, a CT scan showed she had two clots in her brain and patchy “ground glass” in her lungs — the opacity in CT scans that is a hallmark of covid-19 infection. She was given two different types of therapy to try to break up the clots and by Day 10, she was well enough to be discharged.
Oxley said the most important thing for people to understand is that large strokes are very treatable. Doctors are often able to reopen blocked blood vessels through techniques such as pulling out clots or inserting stents. But it has to be done quickly, ideally within six hours, but no longer than 24 hours: “The message we are trying to get out is if you have symptoms of stroke, you need to call the ambulance urgently. ”
As for the 44-year-old man Oxley was treating, doctors were able to remove the large clot that day in late March, but the patient is still struggling. As of this week, a little over a month after he arrived in the emergency room, he is still hospitalized.
